Respiratory Diseases — MCQs

On this page
"Steeple sign" on X-ray in children is most likely indicative of which condition?
What is true regarding bronchiolitis obliterans without cyanosis?
A 2-year-old boy presented with cough, fever, and difficulty in breathing. His respiratory rate is 50/min. There is no chest indrawing. Auscultation of the chest reveals bilateral crepitations. What is the most probable diagnosis?
All of the following are useful for treating acute bronchial asthma in children except?
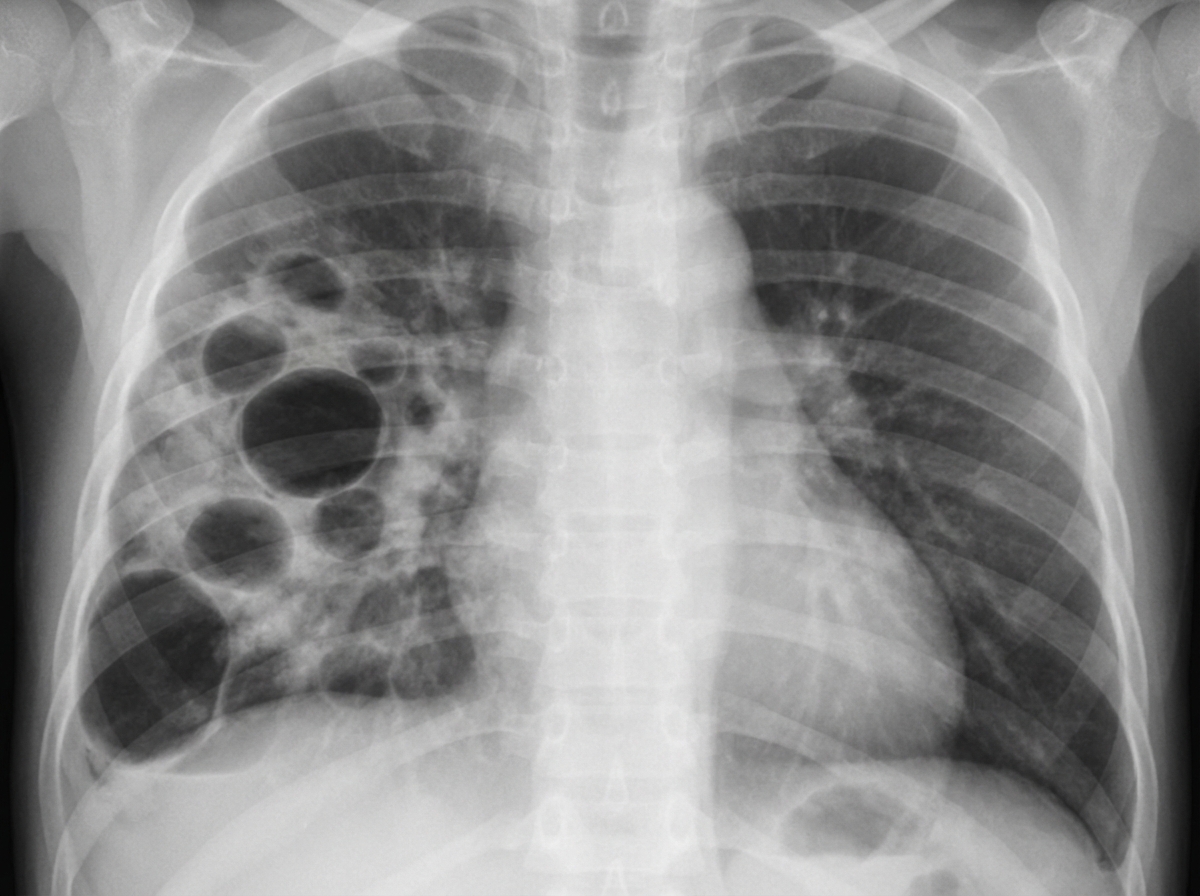
An infant presented to OPD with features of respiratory distress. The X-ray is shown below. The most probable organism is?
What is the most common mode of treatment for a 1-year-old child with asthma?
What is the drug of choice for the prophylaxis of Bronchiolitis in a child with heart disease?
The 'steeple sign' on a radiograph is characteristic of which condition?
An infant is admitted with respiratory distress and prolonged expiration with rhonchi in the chest. Chest X-ray shows hyperinflation. What is the diagnosis?
Crackles are frequently heard in which of the following conditions?
Practice by Chapter
Upper Respiratory Tract Infections
Practice Questions
Lower Respiratory Tract Infections
Practice Questions
Asthma Management
Practice Questions
Cystic Fibrosis
Practice Questions
Bronchiolitis
Practice Questions
Foreign Body Aspiration
Practice Questions
Sleep-Disordered Breathing
Practice Questions
Congenital Lung Malformations
Practice Questions
Pleural Diseases
Practice Questions
Tuberculosis in Children
Practice Questions
Chronic Lung Disease in Premature Infants
Practice Questions
Pulmonary Function Testing
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
