Respiratory Diseases — MCQs

On this page
A child presents with fever, stridor, and barking cough. An X-ray is provided below. Which of the following is true about the patient?
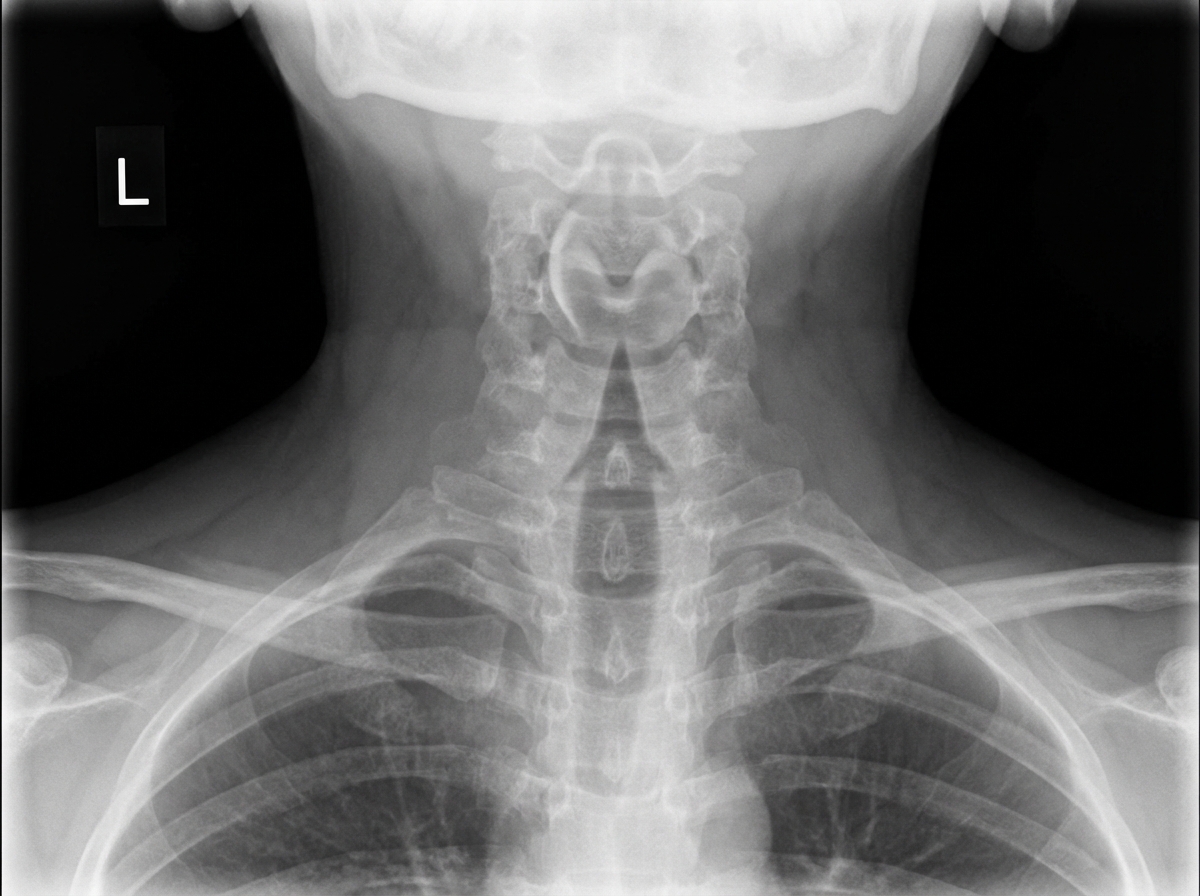
Which of the following is FALSE regarding cystic fibrosis?
Which of the following are features of cystic fibrosis?
Which one of the following values is not a feature of acute severe asthma?
Which of the following findings are true about bronchiolitis in children?
In a child with a suspected foreign body in the lung, what is the next best step in management?
A young boy developed respiratory distress. On examination, the chest X-ray showed hyperinflation of one lung. Which of the following is the most possible diagnosis?
A 3-week-old male infant, born to a primiparous mother, presents with noisy breathing. The child is afebrile, sleeping and feeding well, and has a normal clinical examination. What is the recommended management protocol?
Which of the following childhood disorders is associated with an omega-shaped epiglottis?
What is the most common contributory factor to respiratory failure in patients with cystic fibrosis?
Practice by Chapter
Upper Respiratory Tract Infections
Practice Questions
Lower Respiratory Tract Infections
Practice Questions
Asthma Management
Practice Questions
Cystic Fibrosis
Practice Questions
Bronchiolitis
Practice Questions
Foreign Body Aspiration
Practice Questions
Sleep-Disordered Breathing
Practice Questions
Congenital Lung Malformations
Practice Questions
Pleural Diseases
Practice Questions
Tuberculosis in Children
Practice Questions
Chronic Lung Disease in Premature Infants
Practice Questions
Pulmonary Function Testing
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
