Pediatric Nutrition — MCQs

On this page
Colostrum contains more of _________?
According to the IAP classification of Grade IV malnutrition, what is the weight-for-age of the standard in percentage?
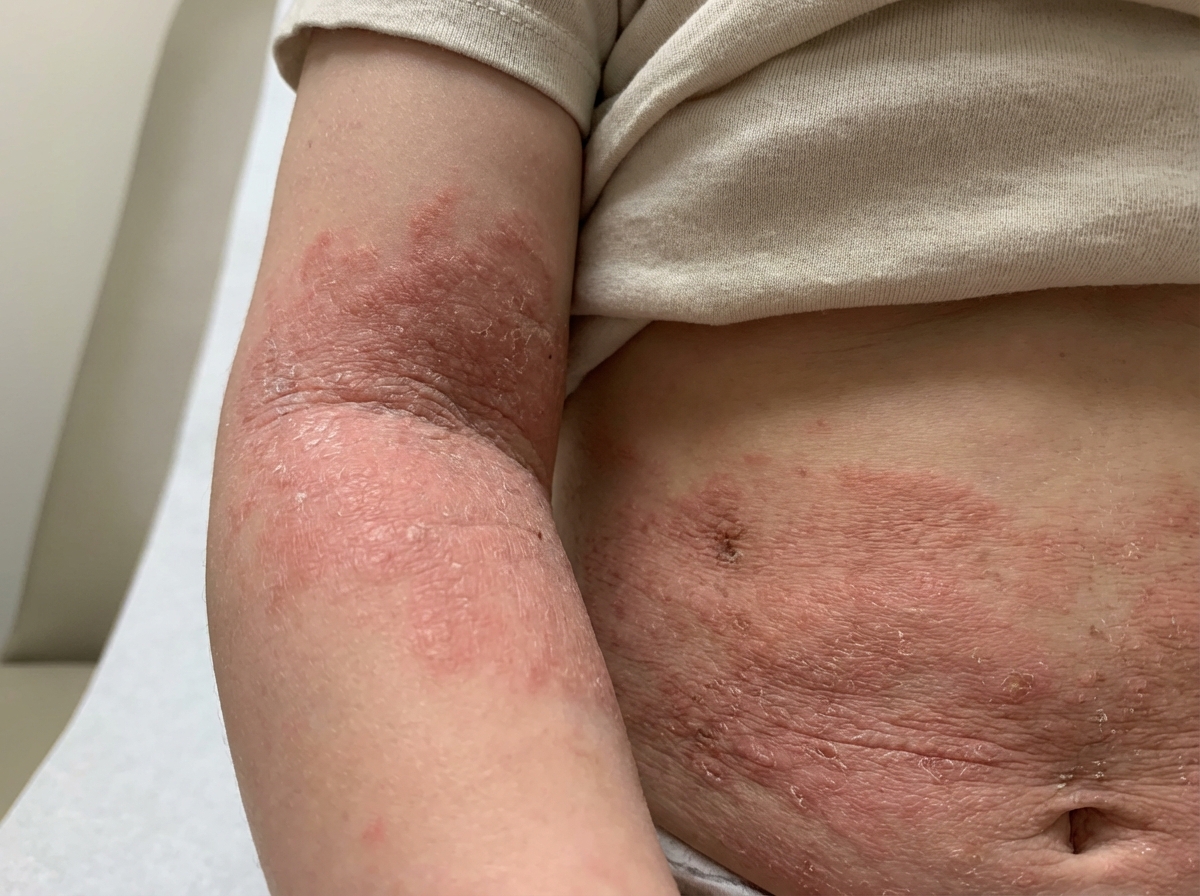
A 5-year-old male child presents with a history of recurrent infections and rashes, as shown in the image. Routine blood investigations reveal thrombocytopenia. Which of the following diagnoses is most likely?
What are the daily caloric requirements for a one-year-old child in kcal/kg/day?
Management of a child with severe protein-energy malnutrition (PEM) and loose stools includes which of the following?
All of the following are signs of inadequate breast milk intake in a neonate, EXCEPT:
Hypervitaminosis of which of the following vitamins will cause bony abnormalities?
Which indicator best reflects both acute and chronic malnutrition?
As compared to cow's milk, human milk has:
The symptoms of dietary deficiency of niacin, which results in pellagra, will be less severe if the diet has a high content of which amino acid?
Practice by Chapter
Breastfeeding
Practice Questions
Infant Formula Feeding
Practice Questions
Complementary Feeding
Practice Questions
Nutritional Requirements by Age
Practice Questions
Malnutrition and Failure to Thrive
Practice Questions
Obesity in Children
Practice Questions
Vitamin Deficiencies
Practice Questions
Mineral Deficiencies
Practice Questions
Food Allergies and Intolerances
Practice Questions
Nutritional Management of Chronic Diseases
Practice Questions
Eating Disorders
Practice Questions
Parenteral and Enteral Nutrition
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
