Oncology — MCQs

On this page
Which of the following is the most common cause of a posterior mediastinum mass in children?
A 5-year-old child presented with abdominal distension, pallor, easy bruising, and bone pain. Physical examination revealed hepatosplenomegaly and lymphadenopathy. The child was suspected to have a metabolic disorder, and a bone marrow biopsy was planned for histopathologic examination. Microscopic examination of the stained biopsy showed a distended phagocytic cell with fibrillary cytoplasm and an eccentrically placed nucleus. Periodic acid-Schiff (PAS) staining was intensely positive. Given this presentation, what is the primary management strategy for this condition?
What is the most likely diagnosis?
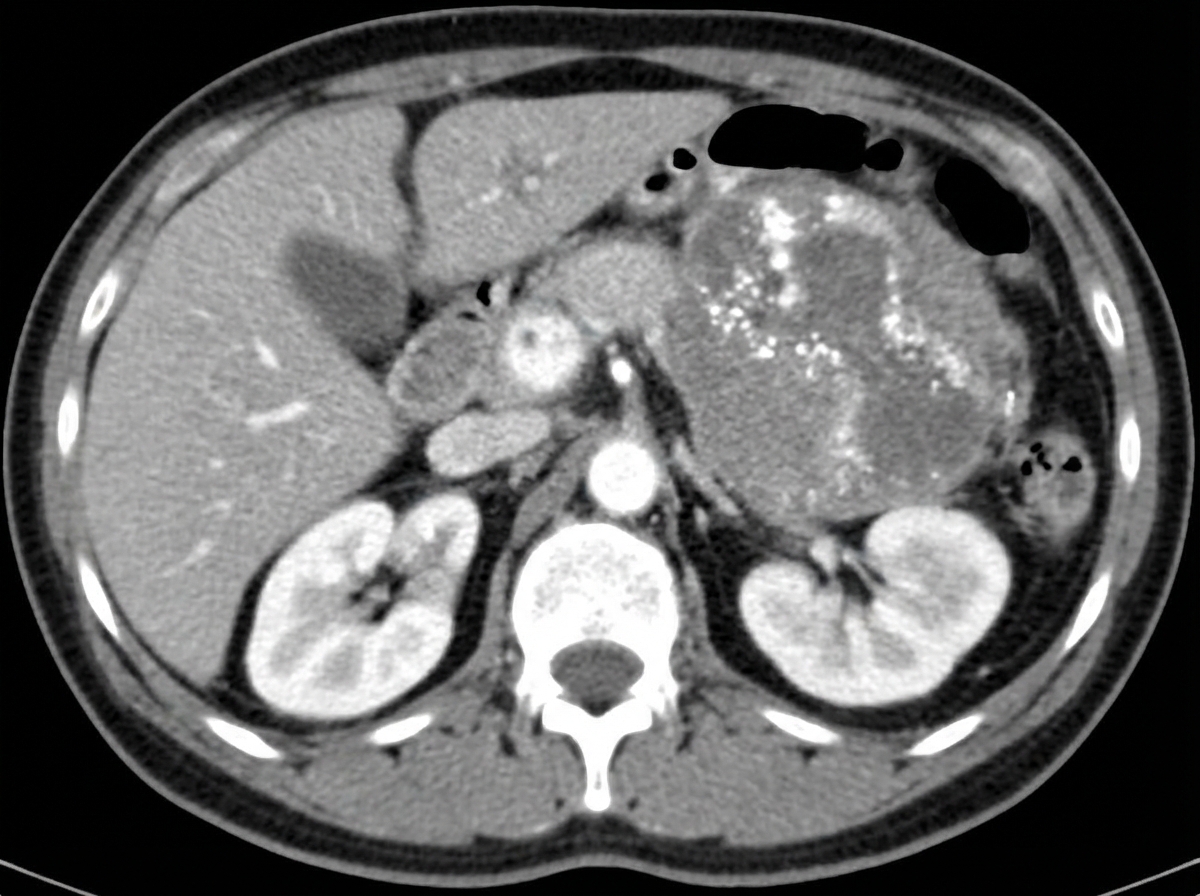
A pediatrician discovers a large mass in the abdomen of a 3-year-old child. Ultrasound examination demonstrates that the mass appears to arise from the right kidney. Which of the following tumors is most likely present?
Which among the following is the most common thyroid malignancy in children?
Spontaneous regression can occur with which of the following conditions?
A child presents with proptosis, multiple skeletal limb secondaries, and sutural separation. What is the most likely diagnosis?
Which of the following malignancies is classified by the Chang staging system?
Which of the following is a poor prognostic indicator in ALL in children?
Blast cells of acute lymphocytic leukemia in childhood characteristically contain which of the following?
Practice by Chapter
Leukemias
Practice Questions
Lymphomas
Practice Questions
CNS Tumors
Practice Questions
Neuroblastoma
Practice Questions
Wilms Tumor
Practice Questions
Rhabdomyosarcoma
Practice Questions
Bone Tumors
Practice Questions
Retinoblastoma
Practice Questions
Histiocytosis Syndromes
Practice Questions
Principles of Pediatric Chemotherapy
Practice Questions
Hematopoietic Stem Cell Transplantation
Practice Questions
Late Effects of Cancer Treatment
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
