Oncology — MCQs

On this page
In a child, which of the following conditions does NOT typically involve CSF examination for diagnosis?
What is the most common abdominal tumor in children?
A 4-year-old child presented with a palpable abdominal mass in the right flank region which was painless and slowly increasing in size along with some episodes of fever and hematuria. On examination, hypertension was noted. CT scan of the abdomen was done. The patient was operated and the mass was resected. The gross specimen and the HPE examination are given below. All of the following genes can be mutated in the above disease except?
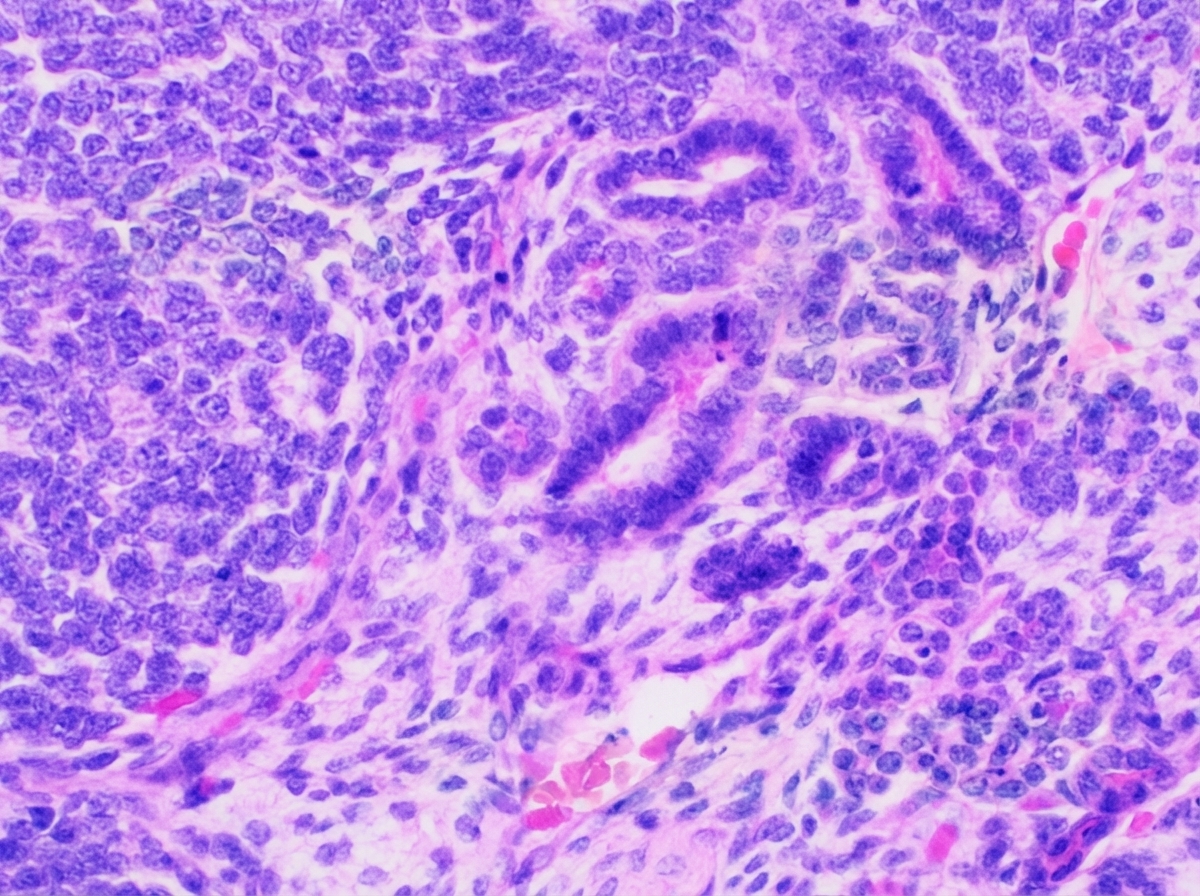
A malignant tumor of childhood that frequently metastasizes to bone marrow most often is:
Neuroblastoma differs from Wilms tumor by all, EXCEPT:
The following physical appearance is seen in which of the following conditions?
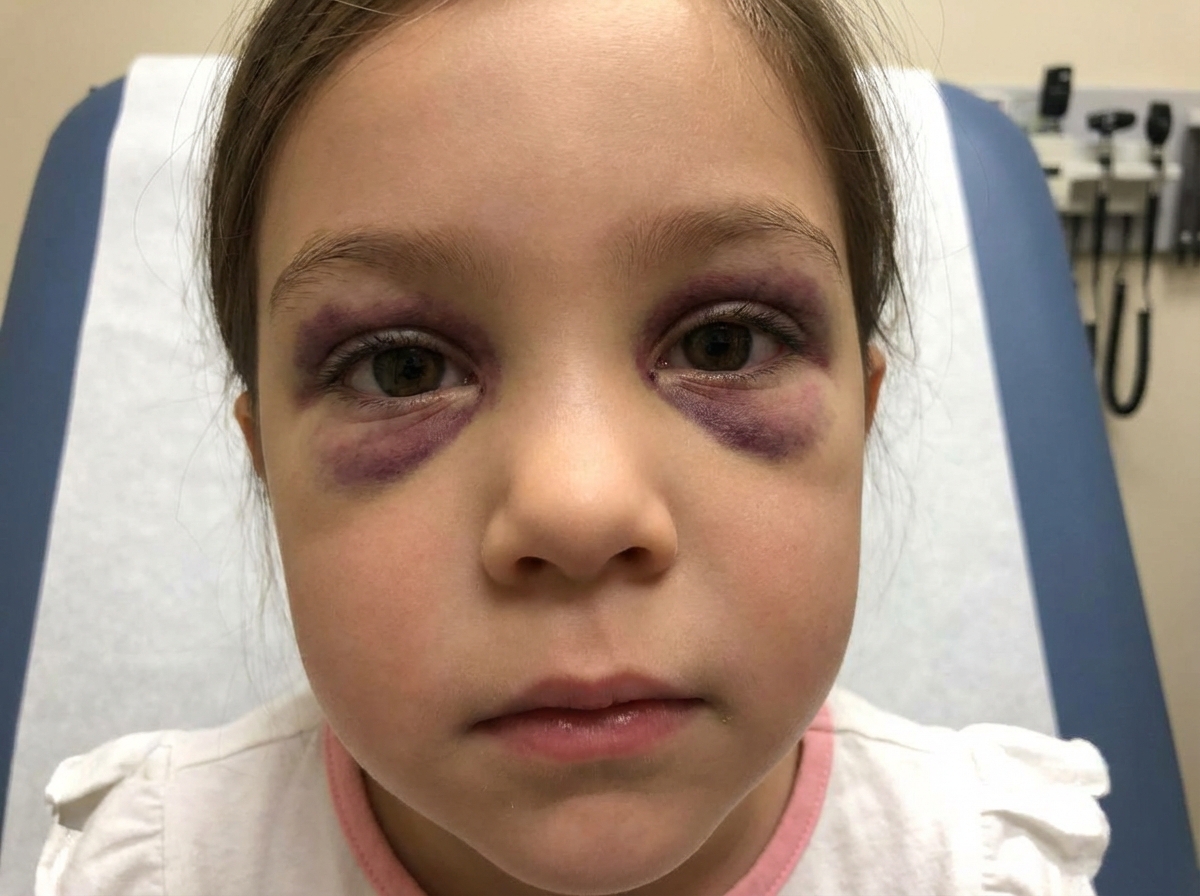
The most common site of neuroblastoma is
A 9-year-old female child presents with a history of headache and visual disturbances. What is the most likely diagnosis?
Which of the following is true about leukemia in Down's syndrome?
Which of the following is NOT a good prognostic factor for Acute Lymphoblastic Leukemia (ALL)?
Practice by Chapter
Leukemias
Practice Questions
Lymphomas
Practice Questions
CNS Tumors
Practice Questions
Neuroblastoma
Practice Questions
Wilms Tumor
Practice Questions
Rhabdomyosarcoma
Practice Questions
Bone Tumors
Practice Questions
Retinoblastoma
Practice Questions
Histiocytosis Syndromes
Practice Questions
Principles of Pediatric Chemotherapy
Practice Questions
Hematopoietic Stem Cell Transplantation
Practice Questions
Late Effects of Cancer Treatment
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
