Traumatic Brain Injury — MCQs

First step in management of raised intracranial pressure-
In patient of head injuries with rapidly increasing intracranial tension without hematoma, the drug of choice for initial management would be :
Signs of increased intracranial tension are all except:
Which of the following is false regarding cranial trauma?
Which of the following is not true about non-contrast CT scan in head injury?
Which one of the following is a secondary brain injury?
Neurological status is assessed under which step of ABCDE of trauma care?
A man presents to the emergency department with a head injury following a vehicular accident. What is the investigation of choice?
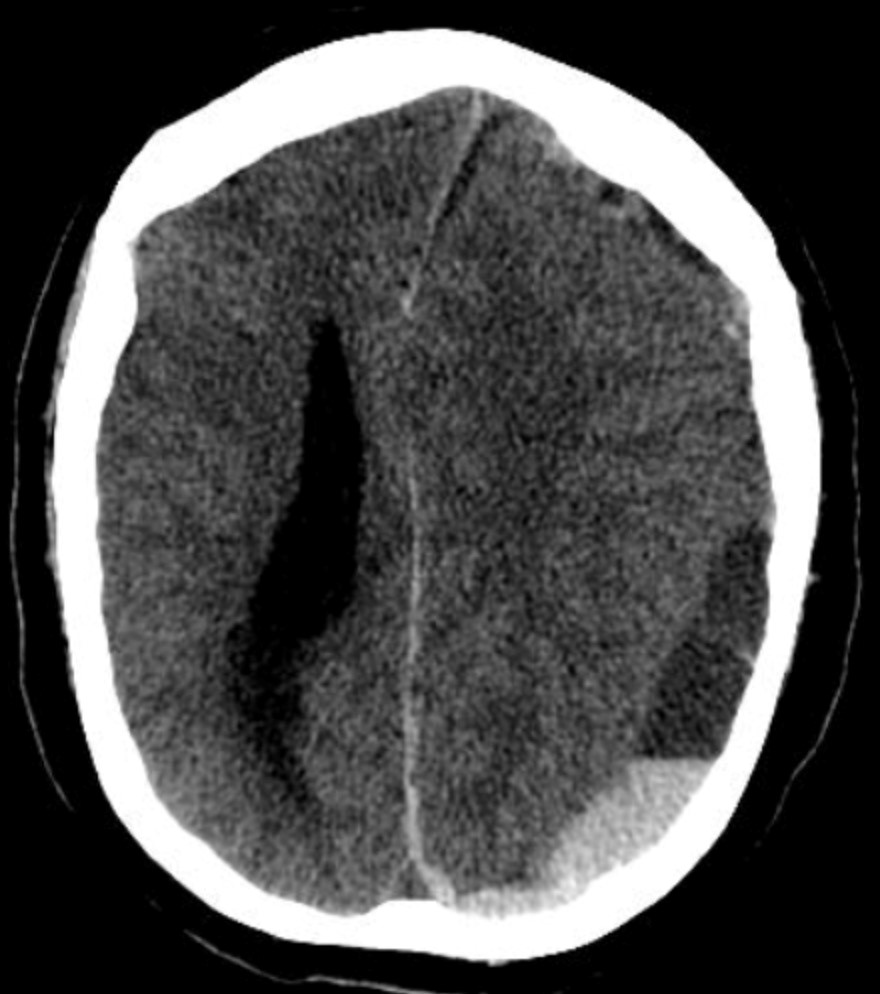
A polytrauma patient's CT brain shows a crescent-shaped extra-axial collection with a concave inner margin. What is the most likely diagnosis?
A child with moderate to severe head injury is admitted in PICU. First line treatments are all except:
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
