Nephrology — MCQs

On this page
What is the formula for calculating GFR?
A child presents with proteinuria, gross hematuria, sensorineural deafness, and anterior lenticonus. What is the inheritance pattern of this condition?
A 4-month-old infant with a urinary tract infection (UTI) was treated for 14 days with IV cefotaxime. What is the next step in management?
A child presented with frothy urine, massive proteinuria, and edema. Urine examination revealed no RBCs, no WBCs, no casts, and no crystals. There is no prior episode of similar presentation. What is your diagnosis?
A 5-year-old child develops the sudden onset of bloody diarrhea, vomiting of blood, hematuria, and renal failure following a flulike gastrointestinal illness. The blood urea nitrogen (BUN) level is markedly increased, but fibrin degradation products and blood clotting times are within normal limits. A peripheral blood smear reveals poikilocytes, schistocytes, and a decrease in the number of platelets. No fever or neurologic symptoms are present. What is the best diagnosis for this patient?
Regarding Hemolytic Uremic Syndrome (HUS), all of the following are true except:
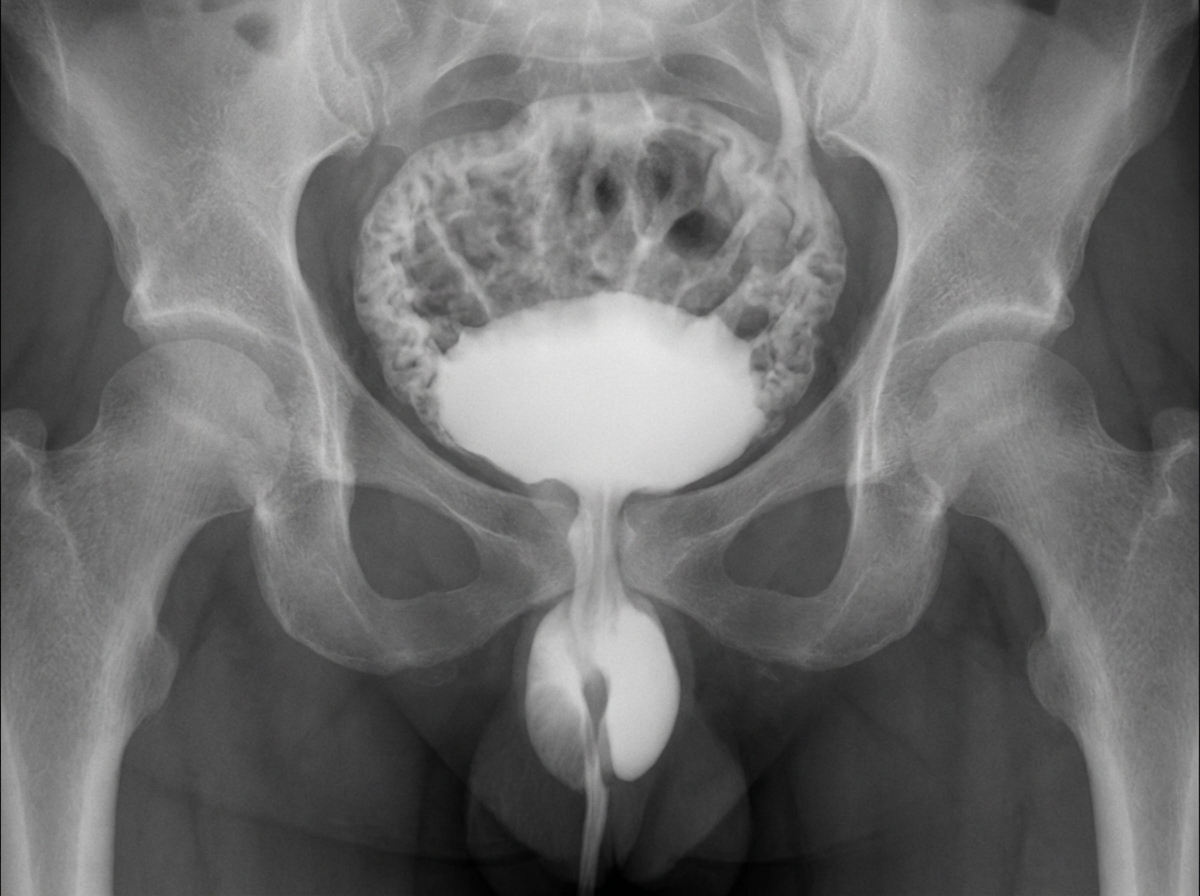
A male child presents with repeated urinary infections and failure to gain weight. A MCU was carried out as shown in the provided image. What is the most probable diagnosis?
Shigella associated hemolytic uremic syndrome is associated with all of the following except?
What is true about minimal change disease?
What is the marker for renal vasculitis in children?
Practice by Chapter
Urinary Tract Infections
Practice Questions
Vesicoureteral Reflux
Practice Questions
Glomerulonephritis
Practice Questions
Nephrotic Syndrome
Practice Questions
Acute Kidney Injury
Practice Questions
Chronic Kidney Disease
Practice Questions
Renal Tubular Disorders
Practice Questions
Congenital Anomalies of the Kidney
Practice Questions
Hydronephrosis
Practice Questions
Hypertension in Children
Practice Questions
Hemolytic Uremic Syndrome
Practice Questions
Renal Replacement Therapy in Children
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
