Nephrology — MCQs

On this page
A 4-year-old girl with Henoch-Schönlein purpura presents with abdominal pain, palpable purpura, hematuria, and nephrotic-range proteinuria. Renal biopsy shows mesangial proliferative glomerulonephritis with IgA deposits. What is the most appropriate treatment plan for this patient?
A child presents with bedwetting at night, and urinalysis is normal. What is the next management step?
A 7-year-old child presents with hematuria, hypertension, and periorbital edema. Laboratory tests show elevated antistreptolysin O (ASO) titers. What is the most likely diagnosis?
A 3-year-old child presents with a history of recurrent urinary tract infections, poor growth, and hypertension. What is the most likely diagnosis?
A 5-year-old boy presents with a history of nocturnal enuresis and recurrent urinary tract infections. What is the most appropriate initial investigation?
An 8-year-old child presents with hematuria 5 days after a throat infection. What is the most likely diagnosis?
In HSP gross hematuria is seen in what % of children?
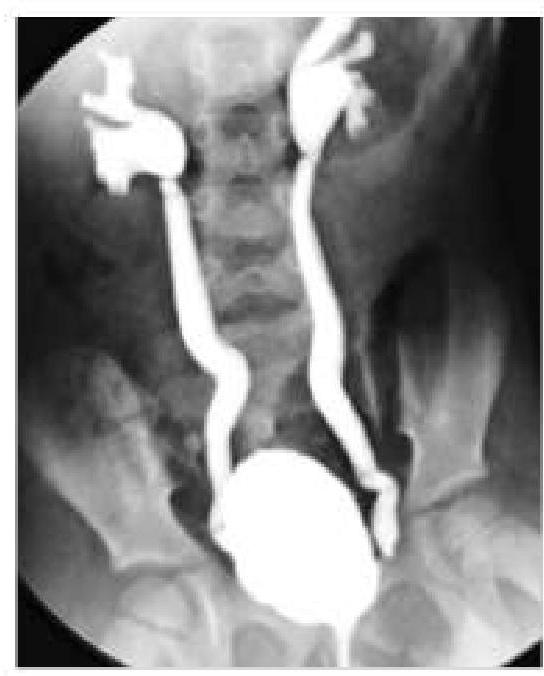
A 6-year-old boy came with a history of recurrent urinary tract infections. Imaging was done and showed retrograde flow of urine from the bladder into the ureters. What is the most likely diagnosis based on the imaging findings?
Which of the following is NOT typically associated with posterior urethral valves?
Which of the following statements about chronic pyelonephritis in children is true?
Practice by Chapter
Urinary Tract Infections
Practice Questions
Vesicoureteral Reflux
Practice Questions
Glomerulonephritis
Practice Questions
Nephrotic Syndrome
Practice Questions
Acute Kidney Injury
Practice Questions
Chronic Kidney Disease
Practice Questions
Renal Tubular Disorders
Practice Questions
Congenital Anomalies of the Kidney
Practice Questions
Hydronephrosis
Practice Questions
Hypertension in Children
Practice Questions
Hemolytic Uremic Syndrome
Practice Questions
Renal Replacement Therapy in Children
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
