Nephrology — MCQs

On this page
A 7-year-old child presents with generalized edema, frothy urine, and fatigue for 2 weeks. Laboratory findings show serum albumin 1.8 g/dL, total cholesterol 350 mg/dL, and 24-hour urine protein 5 g/day. Renal function is normal. Kidney biopsy shows normal glomeruli on light microscopy but effacement of podocyte foot processes on electron microscopy. What is the most appropriate initial treatment?
A 5-year-old child with chronic kidney disease (CKD) presents with bow legs. Laboratory investigations reveal: Serum Calcium: 9.1 mg/dL (normal) Serum Phosphate: 6.9 mg/dL (elevated) Alkaline Phosphatase: Elevated 25(OH) Vitamin D: Low What is the most appropriate next step in management?
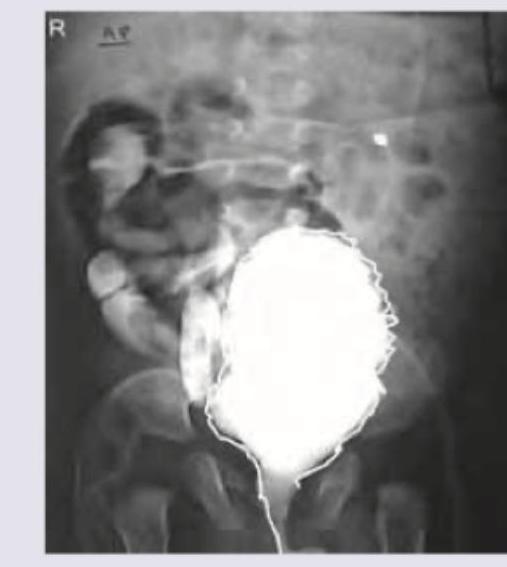
A 1 month old child with recurrent episodes of fever. On examination a suprapubic swelling was noticed and mother reports poor urinary stream. MCUG was performed. All are true about the condition shown except:
A child during evaluation of recurrent hematuria has the following eye finding. He has sensorineural deafness and history of similar illness in family members. What is the diagnosis?

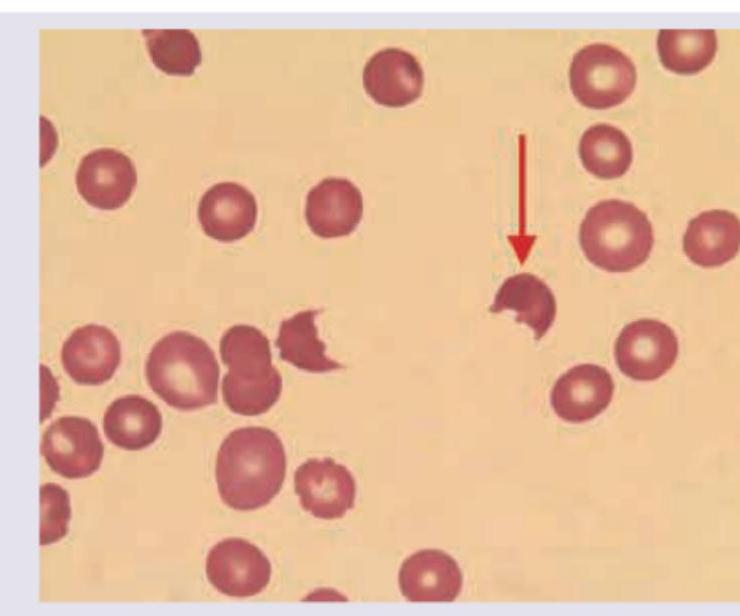
A child with history of diarrhea 1 week back presents with sudden onset pallor and oliguria. Peripheral smear findings are shown below. Which of the following is unlikely finding in this disorder?
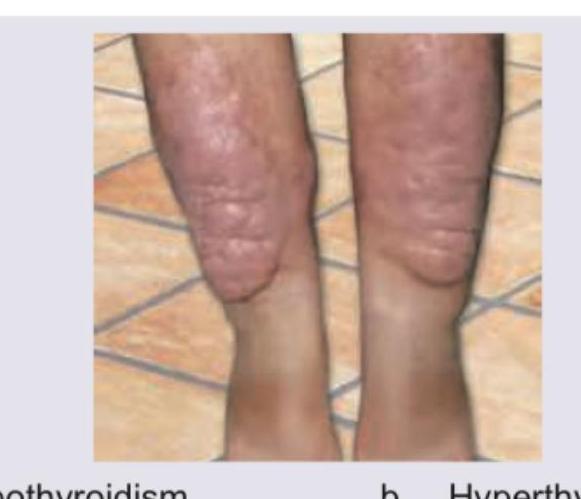
Comment on the diagnosis of the image shown below. (AIIMS Nov 2017)
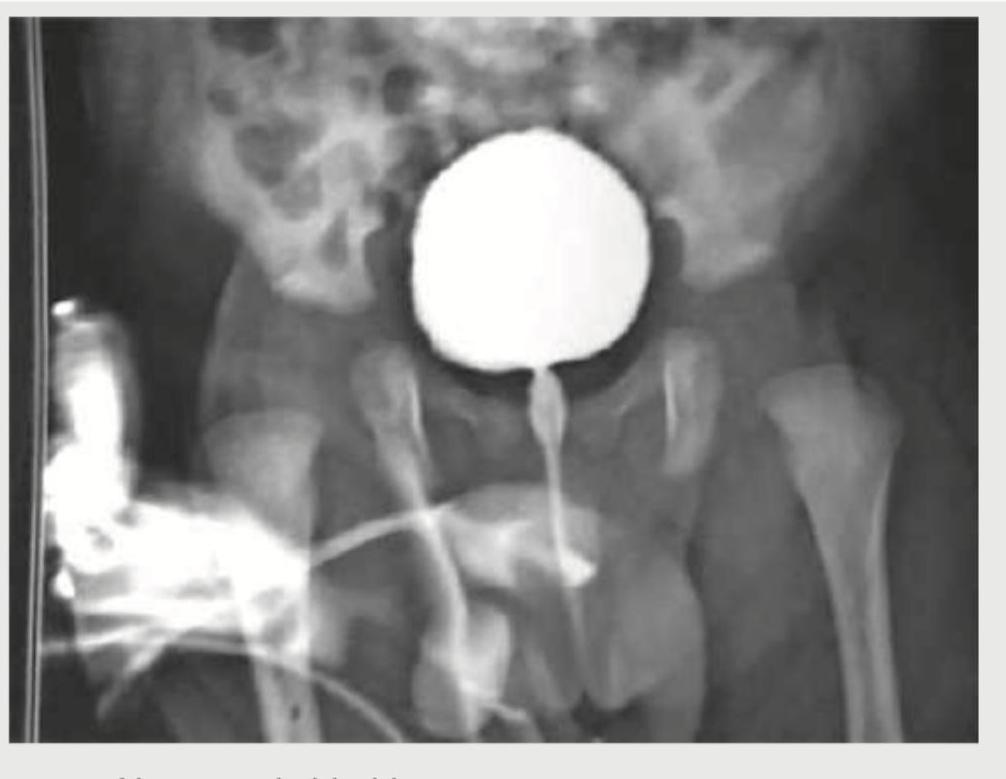
A 3-year-old boy presents with occasional episodes of passing urine after very long durations, going up to as long as 12 hours. Since the child cries due to discomfort and then passes urine with straining, a VCUG is ordered. The VCUG image is shown below. What is the diagnosis?
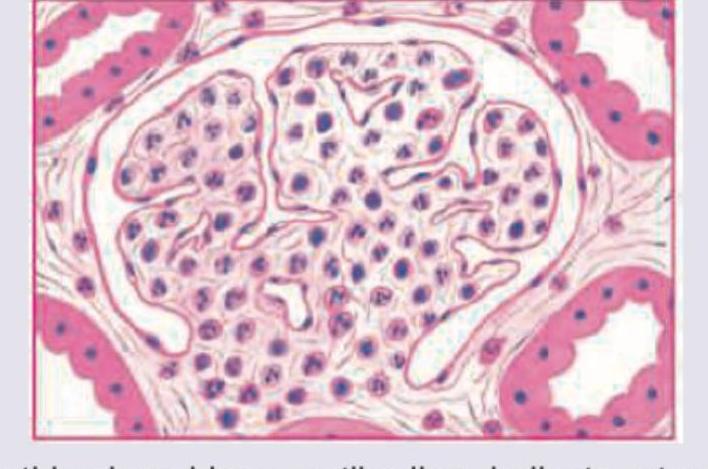
A 6-year-old child presents with puffy eyes, scanty urination. On examination BP=130/80 mmHg and urine examination shows RBC casts. Kidney biopsy specimen is given below. Which of the following is incorrect about the diagnosis of this child?
Autosomal dominant mutations in which one of the following genes may cause focal segmental glomerulosclerosis associated with abnormal genitalia, Wilms tumor and mental retardation?
Which of the following are correct about ectopic ureters? 1. They are more common in males 2. They drain the upper pole of kidney 3. They are associated with duplex ureter 4. They may cause incontinence
Practice by Chapter
Urinary Tract Infections
Practice Questions
Vesicoureteral Reflux
Practice Questions
Glomerulonephritis
Practice Questions
Nephrotic Syndrome
Practice Questions
Acute Kidney Injury
Practice Questions
Chronic Kidney Disease
Practice Questions
Renal Tubular Disorders
Practice Questions
Congenital Anomalies of the Kidney
Practice Questions
Hydronephrosis
Practice Questions
Hypertension in Children
Practice Questions
Hemolytic Uremic Syndrome
Practice Questions
Renal Replacement Therapy in Children
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
