Neonatology — MCQs

On this page
Which of the following is correct regarding "witch's milk"?
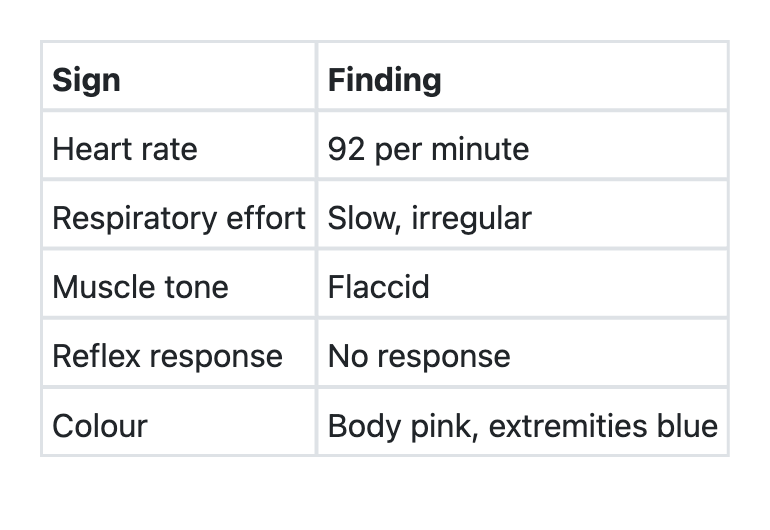
In a newborn, the Apgar score has been recorded at 1 minute of birth. Which one of the following best reflects the Apgar score of this newborn infant on a scale of 0 to 10?
To prevent neonatal tetanus in an infant born to a woman who has not been given Tetanus Toxoid (TT) appropriately during pregnancy, what should ideally be done?
Most common newborn rash which presents at 24-48 hours of life is
Which is the most common laryngeal abnormality that produces laryngeal stridor in a newborn?
A 37-week small-for-date neonate is most likely to develop
When should breastfeeding be initiated to an infant born via a normal delivery?
Neo-natal infection in a Hepatitis 'B' positive pregnant woman can be prevented by administering:
What is the most common cause of intestinal obstruction in neonates?
A woman delivers a healthy baby with weight 2.2 kg at the time of birth. What measures are to be taken? 1. The baby should be exclusively breast fed for first six months 2. The vaccination with OPV and BCG should be delayed till the baby is 2.5 kg of weight 3. Baby should be kept with mother and kangaroo care to be given Select the correct answer using the code given below:
Practice by Chapter
Neonatal Resuscitation
Practice Questions
Care of the Normal Newborn
Practice Questions
Prematurity and Low Birth Weight
Practice Questions
Respiratory Distress Syndrome
Practice Questions
Neonatal Jaundice
Practice Questions
Neonatal Sepsis
Practice Questions
Necrotizing Enterocolitis
Practice Questions
Intraventricular Hemorrhage
Practice Questions
Persistent Pulmonary Hypertension
Practice Questions
Perinatal Asphyxia
Practice Questions
Neonatal Seizures
Practice Questions
Congenital Anomalies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
