Neonatology — MCQs

On this page
Positive pressure ventilation (PPV) in neonatal resuscitation is indicated in all of the following except:
A neonate is being resuscitated as shown in the image. What is the ratio of chest compressions:rescue breaths for this patient?
A child presents in the first week of life with recurrent vomiting, failure to thrive. On examination enlarged liver and spleen are palpated. Blood work shows hyperlipidemia and deranged LFT. CT abdomen was performed. What is the clinical diagnosis?
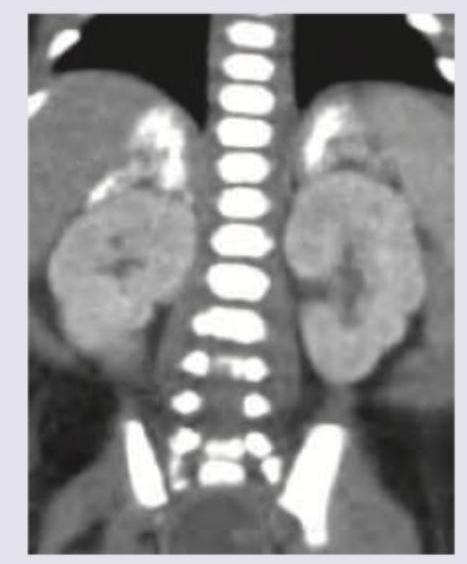
A 2-week-old neonate is brought with complaints of recurrent vomiting, prolongation of physiological jaundice. Urine tests negative for sugar by dipstick but Benedict's test is positive. Which of the following enzymatic defect is most likely responsible for this presentation?
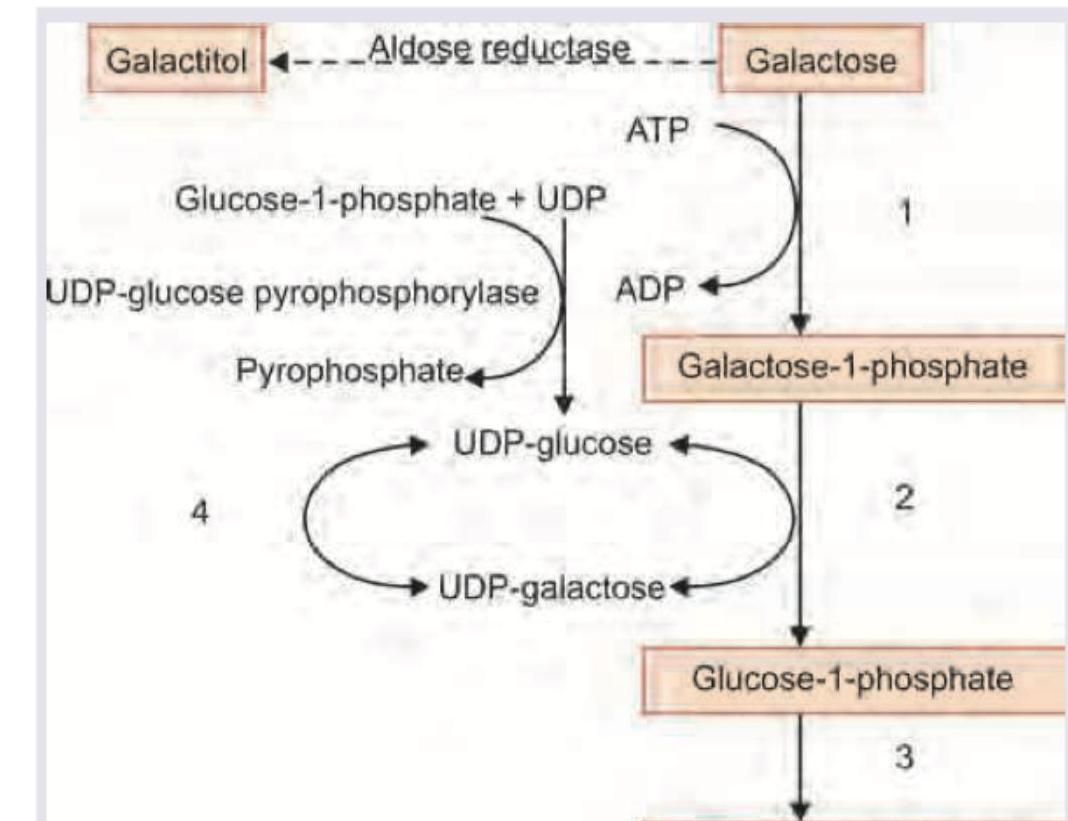
What is incorrect about the neonate shown:
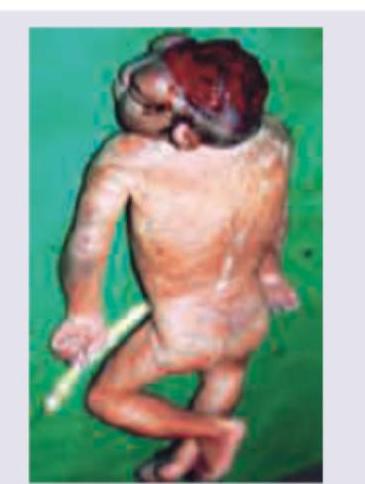
A 2-hour-old neonate born by normal vaginal delivery has a scalp swelling, with normal cry and activity. What is the probable cause?
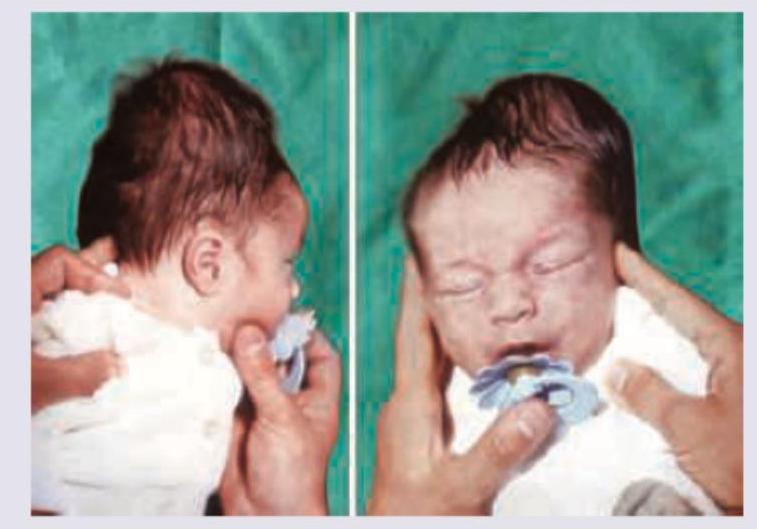
In a neonate with the following findings, what is the likely etiology of hypothyroidism? (NEET Pattern 2018)
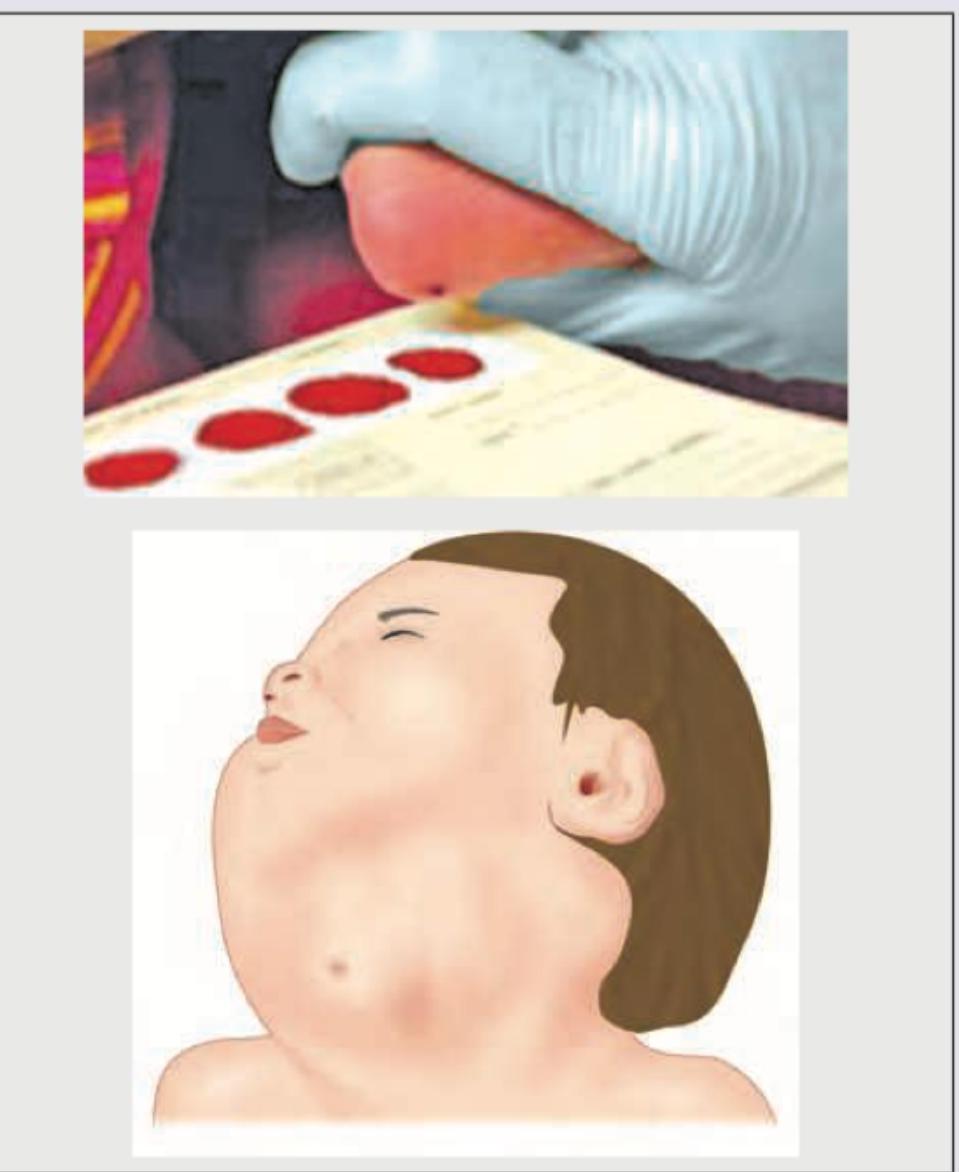
The following kit is used for management of?

The following image shows:
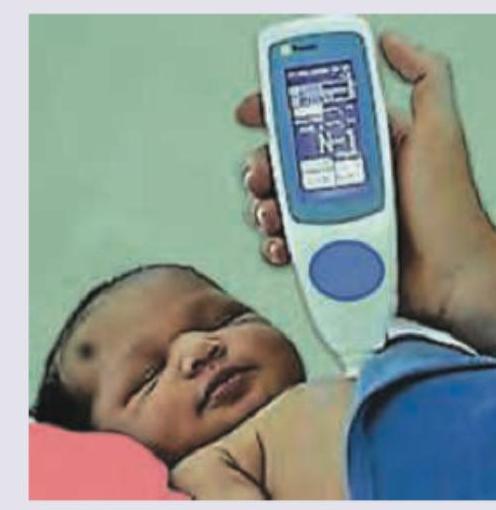
The picture shows a newborn with excessive salivation. Which of the following statements is NOT true regarding the condition shown?
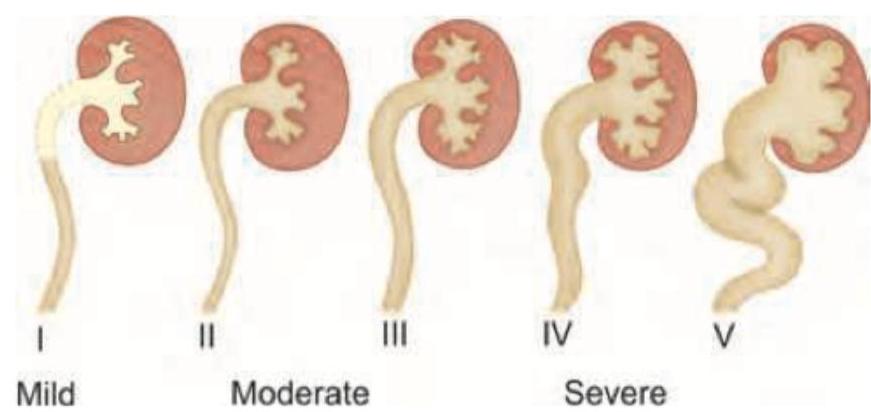
Practice by Chapter
Neonatal Resuscitation
Practice Questions
Care of the Normal Newborn
Practice Questions
Prematurity and Low Birth Weight
Practice Questions
Respiratory Distress Syndrome
Practice Questions
Neonatal Jaundice
Practice Questions
Neonatal Sepsis
Practice Questions
Necrotizing Enterocolitis
Practice Questions
Intraventricular Hemorrhage
Practice Questions
Persistent Pulmonary Hypertension
Practice Questions
Perinatal Asphyxia
Practice Questions
Neonatal Seizures
Practice Questions
Congenital Anomalies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
