Neonatology — MCQs

On this page
Which of the following is considered the most important risk factor for necrotizing enterocolitis?
Which of the following are common physiological problems in neonates?
What does the Apgar score stand for?
A neonate born to a mother with hepatitis B infection should be treated with what intervention?
A 2-day-old newborn baby presented with microcephaly, macroglossia, visceromegaly, and a blood glucose level of 20 mg/dl. What is the most likely diagnosis?
Dental lamina cysts of newborns are seen where?
A newborn has Apgar scores of 3 at 1 minute and 6 at 5 minutes. At 10 minutes, the child shows features of breathlessness. Chest X-ray reveals mediastinal shift. What are the possible causes?
What is the most important indicator of successful neonatal resuscitation?
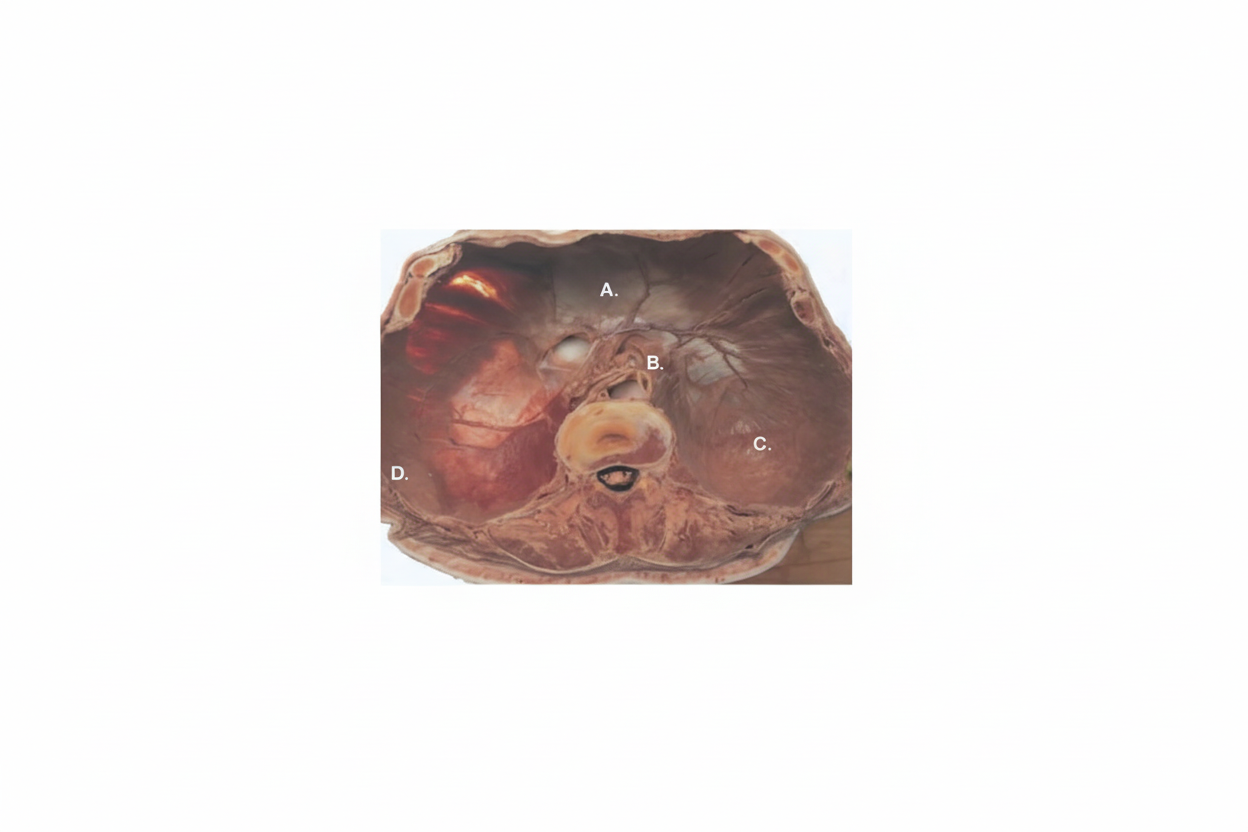
A neonate, within 4 hours of birth, presented with severe respiratory distress. He appears to be dyspneic, tachypneic, and cyanotic with severe retractions of the chest. On examination, grunting is present along with the use of accessory muscles. The neonate also appears to have a scaphoid abdomen and increased chest wall diameter. There is evidence of a shift of the point of maximal cardiac impulse from its original location to the right side. Chest x-ray of the neonate shows a defect in the development of which part of the responsible structure, causing this condition?
The late features of kernicterus include all of the following except:
Practice by Chapter
Neonatal Resuscitation
Practice Questions
Care of the Normal Newborn
Practice Questions
Prematurity and Low Birth Weight
Practice Questions
Respiratory Distress Syndrome
Practice Questions
Neonatal Jaundice
Practice Questions
Neonatal Sepsis
Practice Questions
Necrotizing Enterocolitis
Practice Questions
Intraventricular Hemorrhage
Practice Questions
Persistent Pulmonary Hypertension
Practice Questions
Perinatal Asphyxia
Practice Questions
Neonatal Seizures
Practice Questions
Congenital Anomalies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
