Neonatology — MCQs

On this page
In a neonate, jaundice appears for the first time in the 2nd week. Which of the following is NOT a cause of this presentation?
What is the most common situation associated with transient tachypnea of the newborn?
What is the recommended room temperature for maintaining warmth for neonates?
Which of the following are contraindications to breast milk feeding?
A newborn has a heart rate of 110, has been crying vigorously, with good muscle tone and active movements. The baby has good respiratory effort and rate. The body of the baby is pink in color but the extremities are blue. What is the APGAR score of the child?
All are true about necrotizing enterocolitis except?
With respect to Facility Based Newborn Care (FBNC), which of the following facilities exists at MCH Level I (SC & PHC) for newborn care?
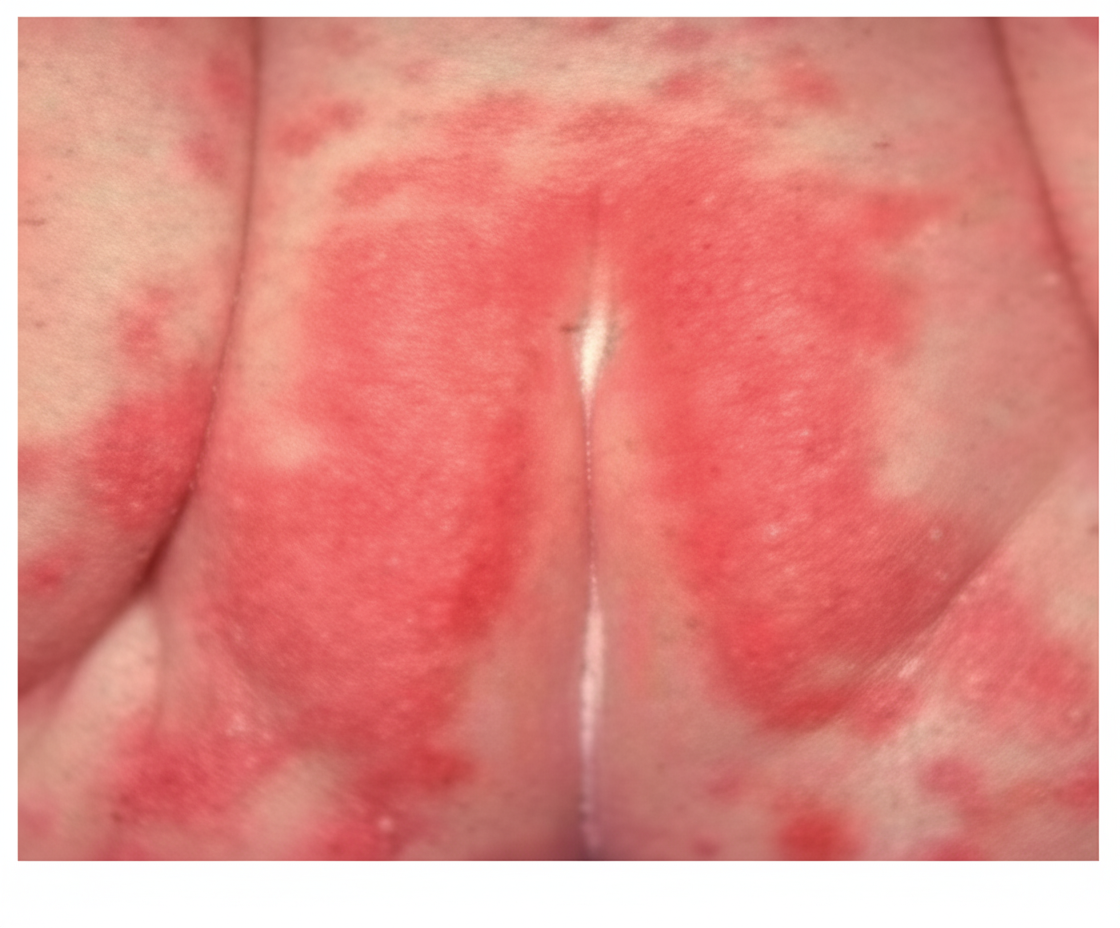
A rash is observed in a neonate admitted to the NICU for 6 days. What is the most likely cause?
Early onset sepsis in a neonate occurs within which timeframe?
What is the best method to monitor the breathing of a non-ventilated preterm baby in an incubator and detect apnea?
Practice by Chapter
Neonatal Resuscitation
Practice Questions
Care of the Normal Newborn
Practice Questions
Prematurity and Low Birth Weight
Practice Questions
Respiratory Distress Syndrome
Practice Questions
Neonatal Jaundice
Practice Questions
Neonatal Sepsis
Practice Questions
Necrotizing Enterocolitis
Practice Questions
Intraventricular Hemorrhage
Practice Questions
Persistent Pulmonary Hypertension
Practice Questions
Perinatal Asphyxia
Practice Questions
Neonatal Seizures
Practice Questions
Congenital Anomalies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
