Neonatology — MCQs

On this page
In full term neonates, what causes the closure of the ductus arteriosus?
What is the effect of administration of large doses of vitamin K in a newborn?
A very ill neonate has widespread granulomas. In utero infection with which of the following organisms is suggested by this finding?
An Rh-negative woman is pregnant with an Rh-positive fetus. A few days after birth, the infant develops jaundice, ascites, hepatomegaly, and edema. What is the likely substance deposited in the skin and sclera in jaundice?
What is the drug of choice for neonatal convulsions?
True regarding APGAR score is all except?
Which of the following features of the neonatal airway enables a baby to breathe while suckling breast milk?
Which factor is responsible for maintaining the patency of the ductus arteriosus in a fetus?
Hydrops fetalis may be caused by the following except?
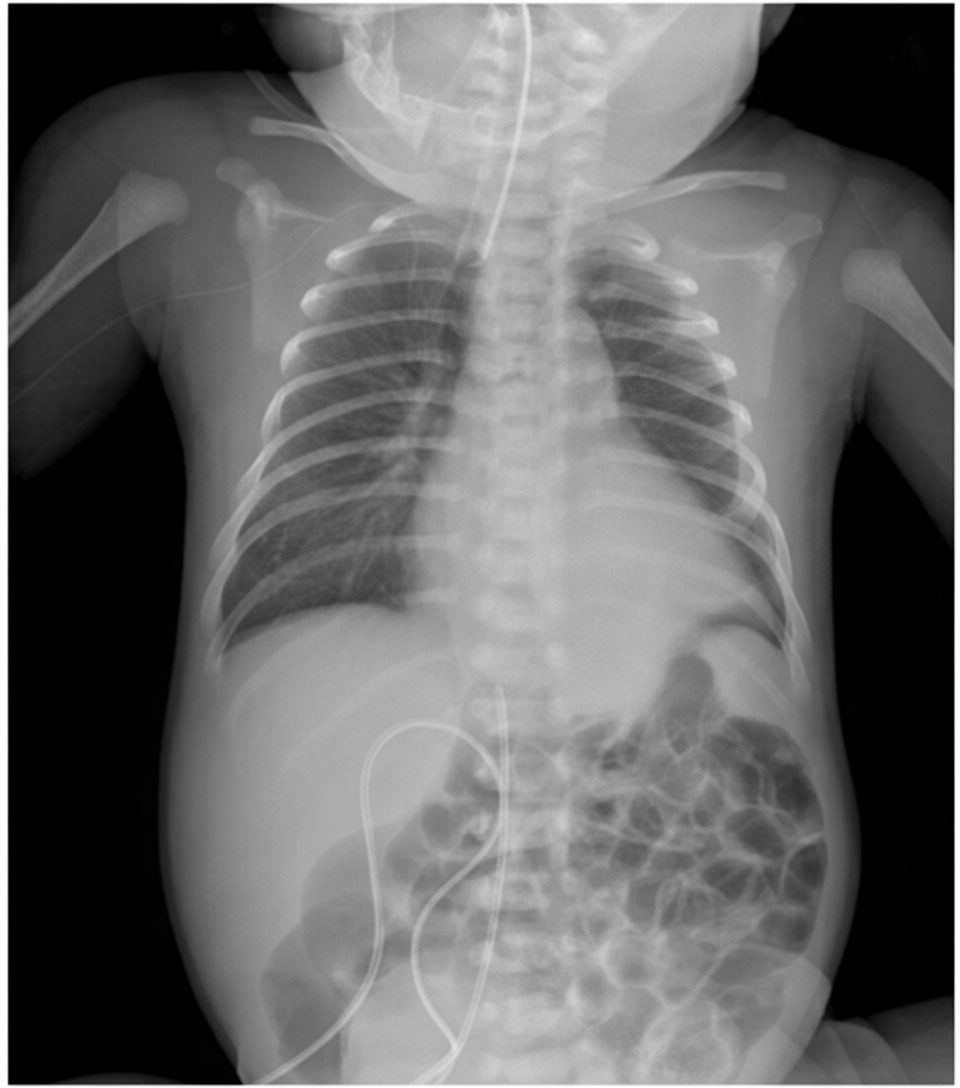
An infant presents with respiratory distress. What is the diagnosis based on the provided X-ray?
Practice by Chapter
Neonatal Resuscitation
Practice Questions
Care of the Normal Newborn
Practice Questions
Prematurity and Low Birth Weight
Practice Questions
Respiratory Distress Syndrome
Practice Questions
Neonatal Jaundice
Practice Questions
Neonatal Sepsis
Practice Questions
Necrotizing Enterocolitis
Practice Questions
Intraventricular Hemorrhage
Practice Questions
Persistent Pulmonary Hypertension
Practice Questions
Perinatal Asphyxia
Practice Questions
Neonatal Seizures
Practice Questions
Congenital Anomalies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
