Neonatology — MCQs

On this page
The item shown below is used to feed newborns born at what gestational age?
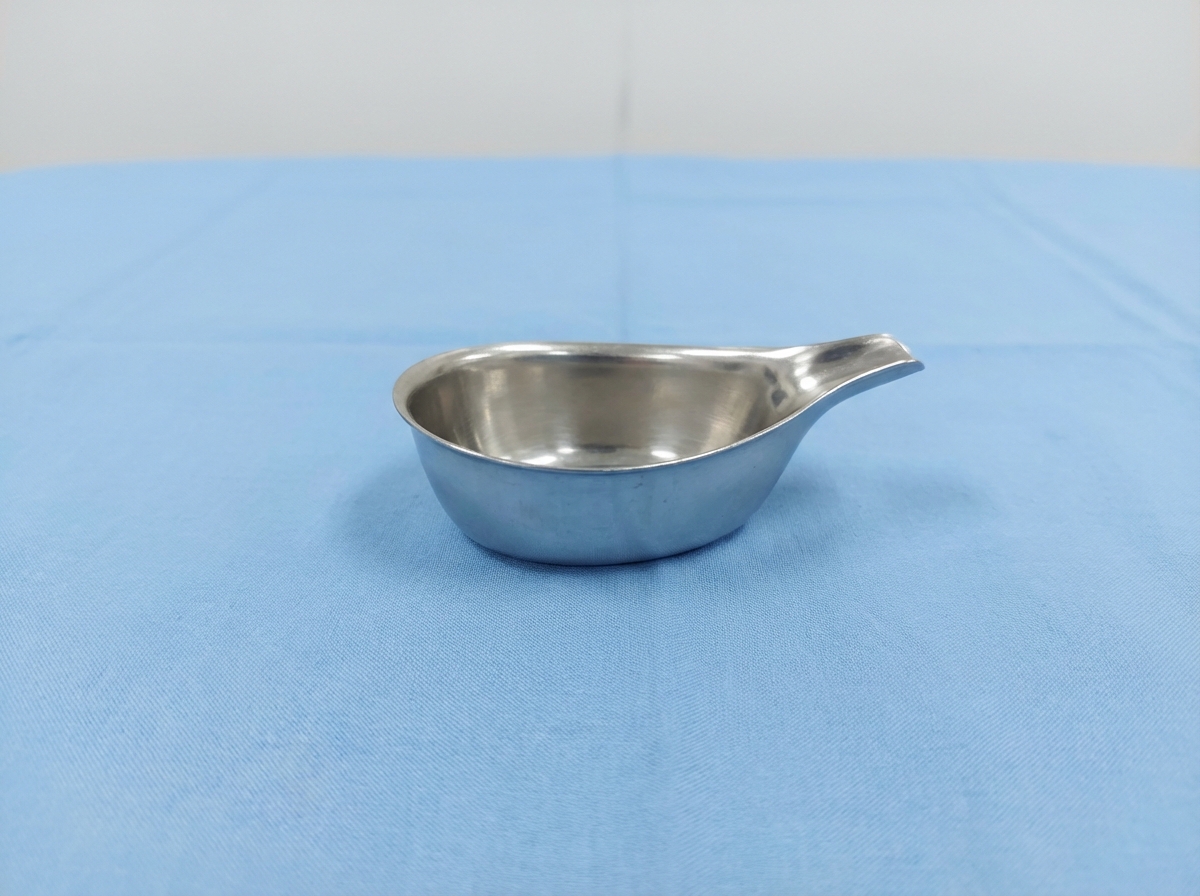
A 4-day-old infant, delivered at home, is brought to the emergency with complaints of bleeding from the umbilical stump. His PT is 24 seconds, APTT is 37 seconds, and platelet count is 200,000/mm3. Apart from maintaining intravascular volume, what would be the definitive line of management?
A three-day-old term infant, born at home and exclusively breast-fed, presented with lethargy, bulging fontanel, and bright red blood from the rectum. What is the most likely etiology of this condition?
What is true about cephalhematoma?
All of the following regarding meconium aspiration syndrome is true EXCEPT?
The neonatal period extends up to which day of life?
Harlequin skin change in the newborn is seen in which of the following conditions?
What is the approximate length of the small bowel in a full-term newborn?
Total body water in a neonate is approximately:
What is the recommended ratio of chest compressions to breathing during cardiopulmonary resuscitation in a newborn patient admitted to the ICU?
Practice by Chapter
Neonatal Resuscitation
Practice Questions
Care of the Normal Newborn
Practice Questions
Prematurity and Low Birth Weight
Practice Questions
Respiratory Distress Syndrome
Practice Questions
Neonatal Jaundice
Practice Questions
Neonatal Sepsis
Practice Questions
Necrotizing Enterocolitis
Practice Questions
Intraventricular Hemorrhage
Practice Questions
Persistent Pulmonary Hypertension
Practice Questions
Perinatal Asphyxia
Practice Questions
Neonatal Seizures
Practice Questions
Congenital Anomalies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
