Neonatology — MCQs

On this page
A 4-week-old newborn presents with jaundice and clay-white stools. A liver biopsy shows giant cells with ballooning degeneration of the cytoplasm. What is the most likely diagnosis?
Which of the following are manifestations of hypothermia?
A female newborn presents with vaginal bleeding four days after birth. What is the appropriate management?
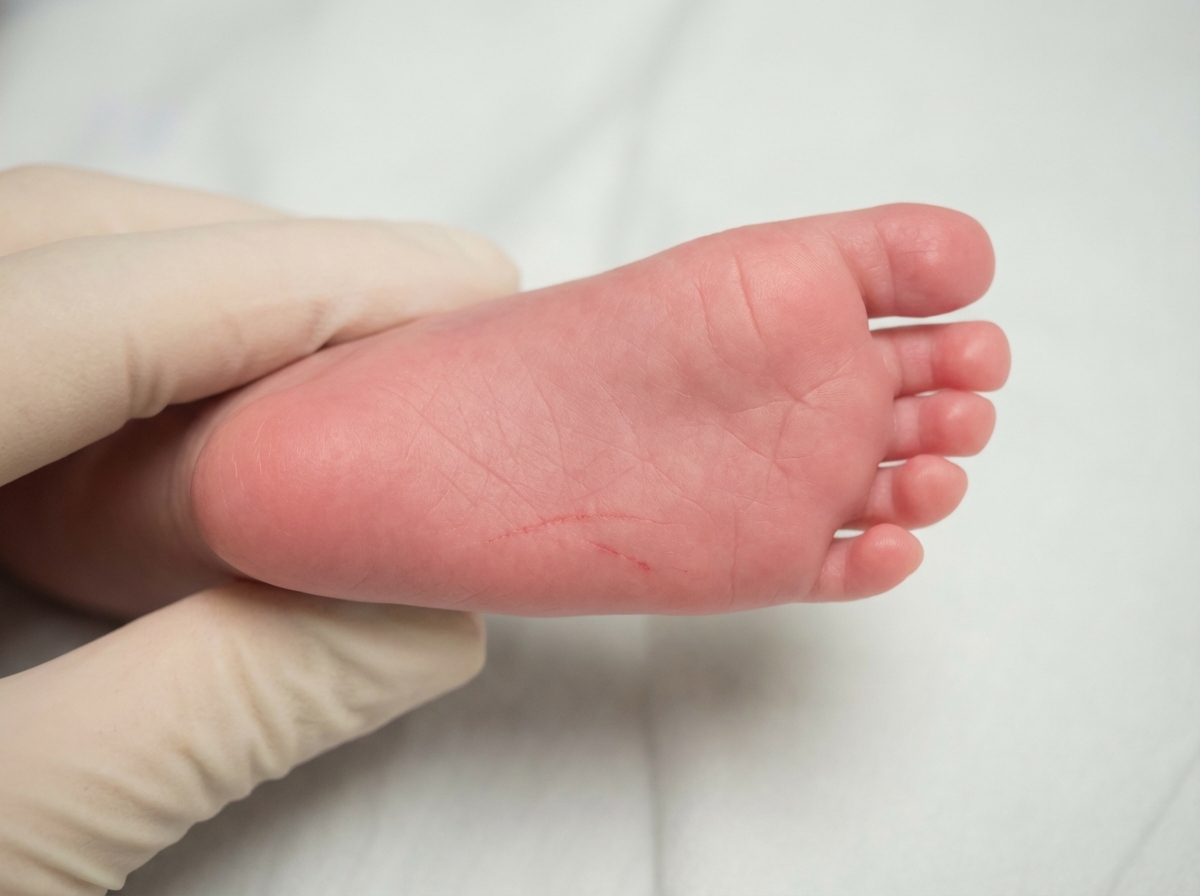
The sole of a newborn baby is suggestive of what condition?
Unconjugated hyperbilirubinemia of the newborn is caused by all of the following EXCEPT:
All of the following are congenital infections EXCEPT:
Breastfeeding should be avoided by a mother on AT (Atorvastatin) for how many weeks?
Vomiting on the first day of a baby's life can be caused by all of the following except?
What is the most characteristic anomaly found in infants of diabetic mothers?
What is the Apgar score in a newborn with the following findings: heart rate of 110, slow and irregular respiratory effort, flaccid muscle tone, no reflex irritability, and blue color?
Practice by Chapter
Neonatal Resuscitation
Practice Questions
Care of the Normal Newborn
Practice Questions
Prematurity and Low Birth Weight
Practice Questions
Respiratory Distress Syndrome
Practice Questions
Neonatal Jaundice
Practice Questions
Neonatal Sepsis
Practice Questions
Necrotizing Enterocolitis
Practice Questions
Intraventricular Hemorrhage
Practice Questions
Persistent Pulmonary Hypertension
Practice Questions
Perinatal Asphyxia
Practice Questions
Neonatal Seizures
Practice Questions
Congenital Anomalies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
