Neonatology — MCQs

On this page
Anatomical closure of ductus arteriosus is completed by which time period?
Jaundice appearing at or within 24 hours of birth is commonly due to?
A term neonate with a birth weight of 3980g showed the following feature. All of the following can be expected in this baby EXCEPT?
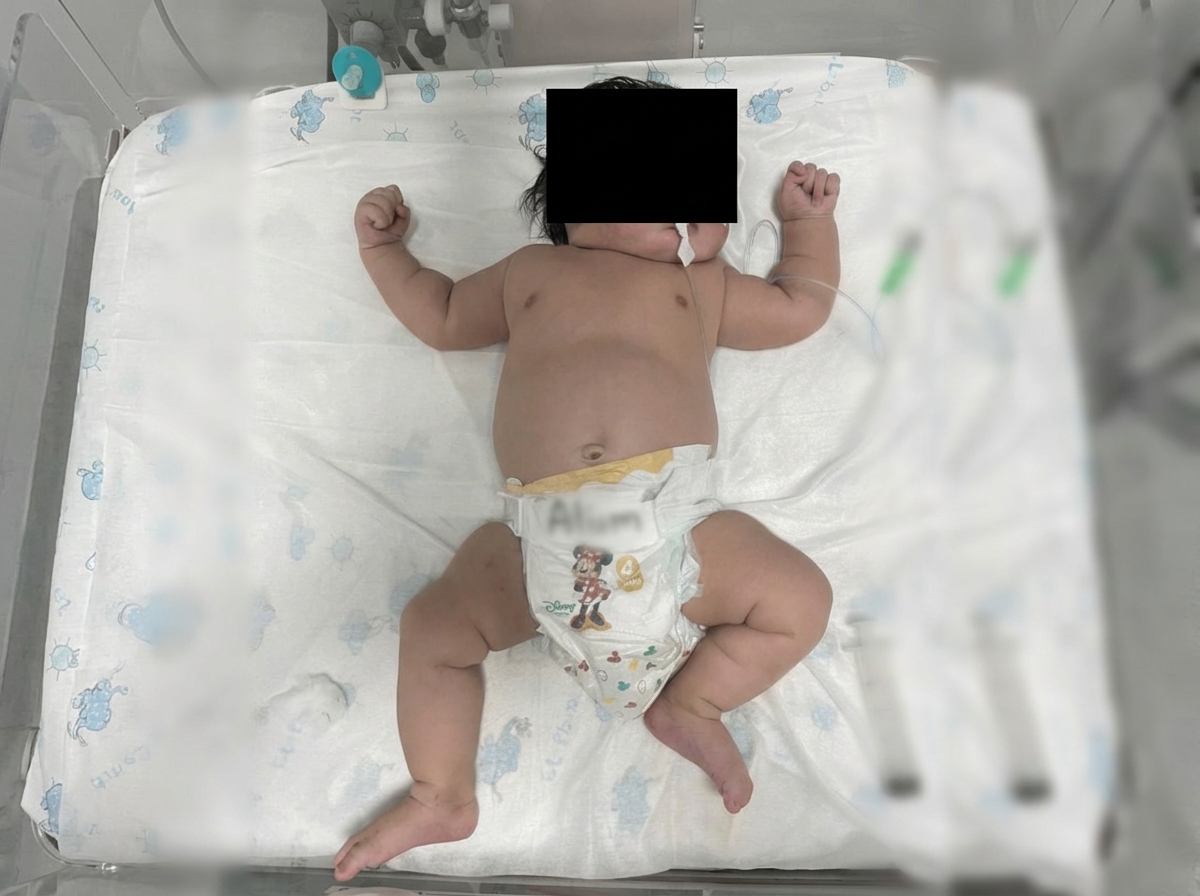
All of the following are risk factors for neonatal hypocalcemia except?
A child develops respiratory distress and a scaphoid abdomen 2 days after birth. Breath sounds are decreased on the left side. After bag and mask ventilation, an endotracheal tube is inserted, and the maximal cardiac impulse shifts to the right side. What is the next step in management?
What is the APGAR score for a newborn with the following findings: respiratory rate of 40/min, heart rate of 80/min, slow and irregular respirations, grimace on suctioning, completely pink color, and flexed posture with active limb movements?
A preterm infant weighing 1600 grams should not receive which of the following vaccines at birth?
Which one of the following statements is TRUE regarding neonatal sepsis?
Kangaroo mother care can be initiated immediately in babies weighing:
For a non-ventilated preterm baby in an incubator, what is the best method to monitor breathing and detect apnea?
Practice by Chapter
Neonatal Resuscitation
Practice Questions
Care of the Normal Newborn
Practice Questions
Prematurity and Low Birth Weight
Practice Questions
Respiratory Distress Syndrome
Practice Questions
Neonatal Jaundice
Practice Questions
Neonatal Sepsis
Practice Questions
Necrotizing Enterocolitis
Practice Questions
Intraventricular Hemorrhage
Practice Questions
Persistent Pulmonary Hypertension
Practice Questions
Perinatal Asphyxia
Practice Questions
Neonatal Seizures
Practice Questions
Congenital Anomalies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
