Neonatology — MCQs

On this page
In neonatal herpes, what is true?
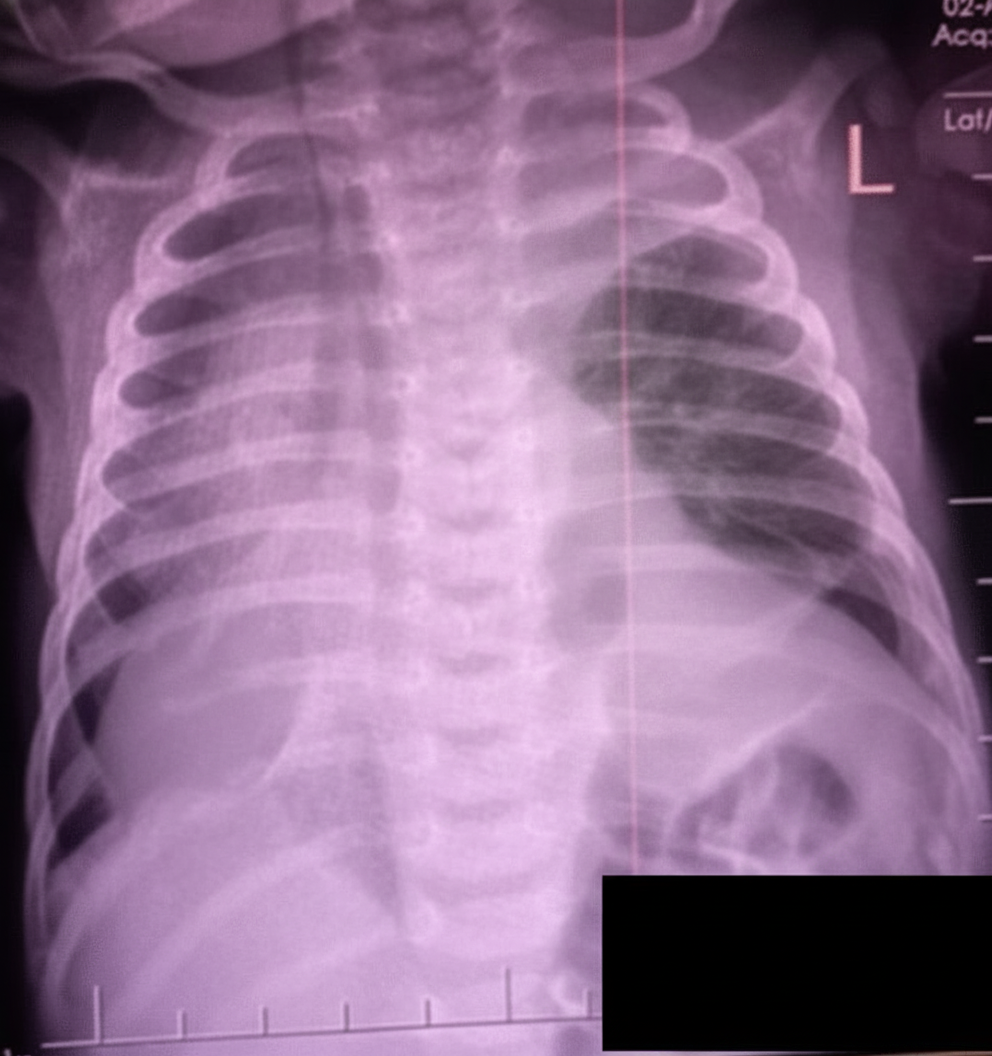
A 3-day-old child presents with the below CXR. What is the diagnosis?
Anatomical closure of the ductus arteriosus occurs at which time interval?
What is the definition of hypertension in a full-term newborn?
A 5-day-old neonate presents with shallow breathing, generalized hypotonia, rigidity, occasional spasms, and foul-smelling brown material around the umbilicus. The child was born at 39 weeks gestation via spontaneous vaginal delivery, with no antenatal care received. The parents reported a normal suck and cry after birth. What is the case load for this condition to be considered eliminated?
An infant of a diabetic mother can have all of the following conditions except:
Which vitamin is administered to newborns to prevent hemorrhage?
A premature baby born to a diabetic mother presented with respiratory distress and was admitted to the neonatal intensive care unit. Which of the following findings indicates Respiratory Distress Syndrome (RDS) in a newborn?
What are keratin-filled cysts commonly found along the midpalatine raphe of a newborn called?
Intrauterine seizure in a fetus is typically seen due to a deficiency of which of the following?
Practice by Chapter
Neonatal Resuscitation
Practice Questions
Care of the Normal Newborn
Practice Questions
Prematurity and Low Birth Weight
Practice Questions
Respiratory Distress Syndrome
Practice Questions
Neonatal Jaundice
Practice Questions
Neonatal Sepsis
Practice Questions
Necrotizing Enterocolitis
Practice Questions
Intraventricular Hemorrhage
Practice Questions
Persistent Pulmonary Hypertension
Practice Questions
Perinatal Asphyxia
Practice Questions
Neonatal Seizures
Practice Questions
Congenital Anomalies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
