Infectious Diseases — MCQs

On this page
A 5 year old child with unprovoked dog bite, appropriate management is
A 3-year-old child is brought to the outpatient department with an upper respiratory tract infection. On asking about their previous immunization history, it is found that they have had no primary immunizations from birth. What is the most appropriate step in the management of this patient?
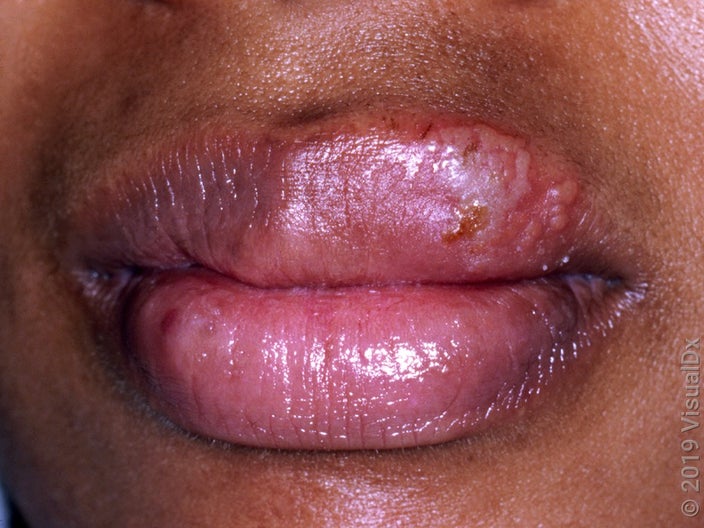
A 10-year-old child had fever for 5 days, along with which he developed multiple fluid filled lesions on the lips as shown below. What is the probable underlying etiology for the skin lesions?
A 3-year-old boy was admitted to the hospital for high fever and difficulty in breathing. He had been well until 4 days before admission, when he developed sneezing and a runny and stuffy nose followed by a non-productive cough the next day. This was followed by appearance of characteristic rash on face, trunk, extremities and back along with fever. On examination: Shotty anterior cervical and supraclavicular lymph nodes, hyperemic conjunctiva, and Koplik spots on buccal mucosa. The white blood cell count was 3,100/ml, with a differential of 70% polymorphonuclear leukocytes. All of the following are complications of the above disease EXCEPT?
A child suffering from Rubella presented with small red spots (petechiae) on the soft palate. These are known as __________.
Prior to discharge of a patient with H. influenzae meningitis, the essential investigation to be done is?
Fever stops and rash begins is diagnostic of –
Which of the following is the most appropriate treatment for a child with severe falciparum malaria with high parasitemia?
Which of the following is NOT true regarding rheumatic chorea in children?
A young child of 7 years of age is seen with indurated ulcers, lymphadenopathy and fever. The likely treatment is:
Practice by Chapter
Vaccine-Preventable Diseases
Practice Questions
Immunization Schedule
Practice Questions
Common Childhood Infections
Practice Questions
Pediatric HIV
Practice Questions
Congenital Infections
Practice Questions
Fever in Infants and Children
Practice Questions
Meningitis and Encephalitis
Practice Questions
Respiratory Tract Infections
Practice Questions
Gastrointestinal Infections
Practice Questions
Parasitic Infections
Practice Questions
Tuberculosis in Children
Practice Questions
Opportunistic Infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
