Infectious Diseases — MCQs

On this page
What is the cause of the 'bull neck' appearance in Diphtheria?
A 2-month-old infant presents with fever, lethargy, and seizures. The infant was born at term with no significant obstetric or early postnatal complications. Physical examination reveals nuchal rigidity and bulging fontanelles. Lumbar puncture shows a high CSF neutrophil count and gram-positive cocci in chains. What is the most likely causative pathogen?
A 28-year-old woman gave birth to a small for gestational age newborn at 38 weeks of pregnancy. On examination, the newborn was found to have rhinitis, a distended abdomen, wrinkled skin, and palmoplantar blisters. The woman had an earlier history of abortion and stillbirth. What is the most likely diagnosis?
A child is suffering from varicella. When is it earliest and safe for the child to meet her pregnant aunt?
A premature baby of 34 weeks gestation was delivered and developed bullous lesions on the skin. Radiographs show periostitis. What should be the next investigation?
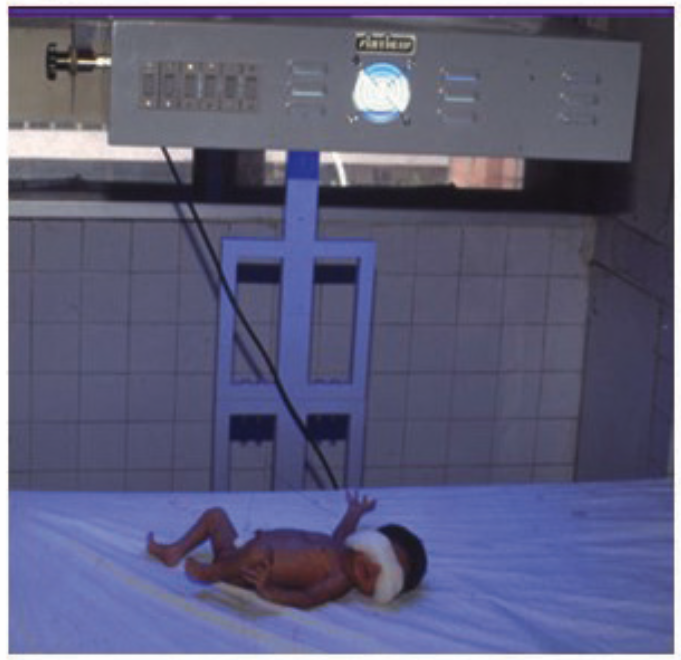
What wavelength is used in the given instrument to treat neonatal pathology?
A 10-year-old boy presents with a two-week history of fever, arthritis, and hepatosplenomegaly. What is the likely diagnosis?
A child presents with fever and maculopapular rash. Which of the following clinical findings is typically NOT associated with measles?
What is the percentage of coincidence between a sore throat and acute rheumatic fever?
What is the standard treatment for Chlamydia pneumoniae infection?
Practice by Chapter
Vaccine-Preventable Diseases
Practice Questions
Immunization Schedule
Practice Questions
Common Childhood Infections
Practice Questions
Pediatric HIV
Practice Questions
Congenital Infections
Practice Questions
Fever in Infants and Children
Practice Questions
Meningitis and Encephalitis
Practice Questions
Respiratory Tract Infections
Practice Questions
Gastrointestinal Infections
Practice Questions
Parasitic Infections
Practice Questions
Tuberculosis in Children
Practice Questions
Opportunistic Infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
