Infectious Diseases — MCQs

On this page
A child presents with fever and unconsciousness for 1 day and pallor with no focal neurological deficit. What is the most probable diagnosis?
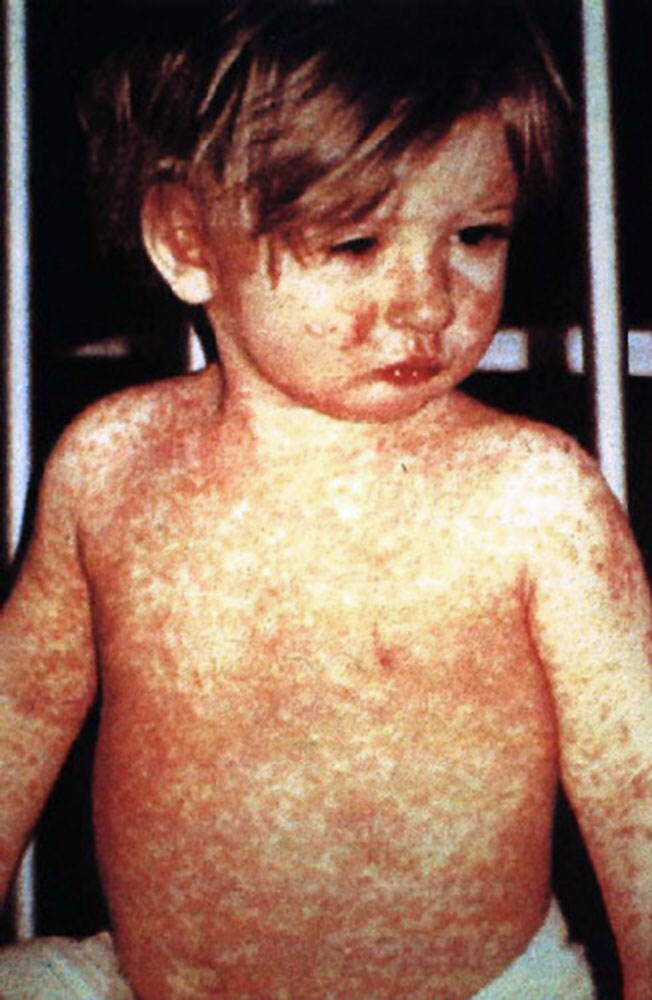
What is the most common complication of measles?
A 6-month-old child presents with recurrent seizures and poor development. The evaluation reveals hydrocephalus, impaired movement of the extremities, hypotonia, and retinal abnormalities. A computerized tomography (CT) scan demonstrates large ventricles and calcified lesions. Which of the following is the most likely diagnosis?
A mother has been infected with rubella during pregnancy. Which of the following fetal congenital malformations can occur?
Primary pneumococcal peritonitis in children is most commonly associated with which of the following conditions?
Which of the following statements about HIV in neonates is incorrect?
Erythema infectiosum is seen in which of the following conditions?
A 60-year-old unvaccinated patient presents to the OPD with fever and red eyes. On examination, a specific type of rash is observed on the body. What is the most likely complication expected with this condition?
A child presents with seborrheic dermatitis, sinusitis, and chronically draining ears. On examination, the child has failure to thrive with hepatosplenomegaly and exophthalmos. What is the probable diagnosis?
A 2-year-old female child was brought to a PHC with a history of cough and fever for 4 days and inability to drink for the last 12 hours. On examination, the child weighed 5 kg and had a respiratory rate of 45/minute with fever. How would this child be classified?
Practice by Chapter
Vaccine-Preventable Diseases
Practice Questions
Immunization Schedule
Practice Questions
Common Childhood Infections
Practice Questions
Pediatric HIV
Practice Questions
Congenital Infections
Practice Questions
Fever in Infants and Children
Practice Questions
Meningitis and Encephalitis
Practice Questions
Respiratory Tract Infections
Practice Questions
Gastrointestinal Infections
Practice Questions
Parasitic Infections
Practice Questions
Tuberculosis in Children
Practice Questions
Opportunistic Infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
