Infectious Diseases — MCQs

On this page
An 11-day-old neonate presents with a sharp cough, mild conjunctivitis with pus, and pneumonia confirmed on chest film. Gram stain of the pus shows no organisms. What is the most likely causative agent?
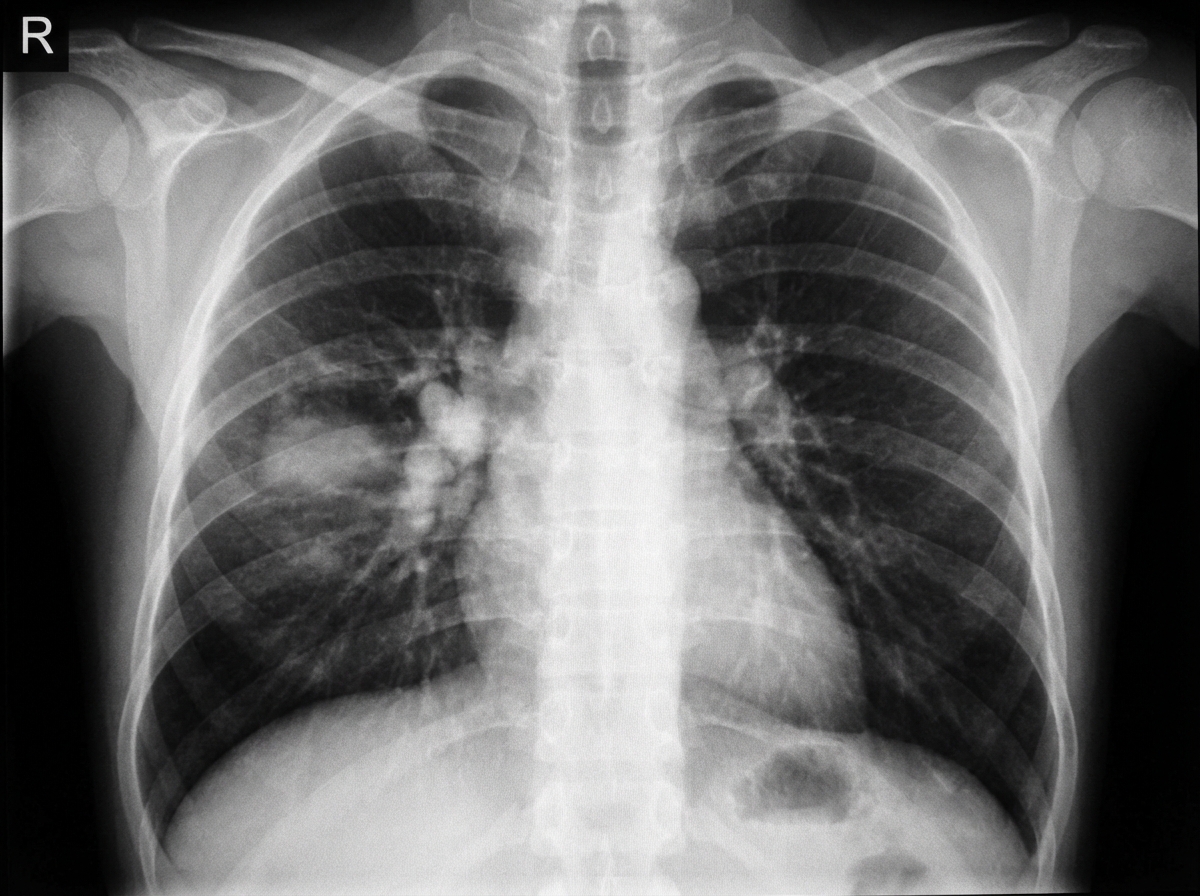
A 4-year-old child presented with cough persisting for 1 month and low-grade fever. There was a history of contact with TB. What is the chest X-ray suggestive of?
What is the diagnostic method for congenital syphilis?
CSF findings show protein 60%, sugar 40%, and neutrophils are predominant. What is the most likely diagnosis?
What is the recommended duration for isolation of a patient with bacterial meningitis?
A 2-year-old child is admitted to the ICU due to complications thought to be secondary to measles infection. Which of the following is the least common complication of measles?
In neonatal sepsis, which of the following is an acute phase reactant?
Primary complex in which of the following sites suggests congenital tuberculosis?
In cases of Streptococcal pharyngitis, how early should treatment be initiated to effectively prevent Rheumatic fever?
Which of the following investigations is the best method for diagnosing HIV in childhood?
Practice by Chapter
Vaccine-Preventable Diseases
Practice Questions
Immunization Schedule
Practice Questions
Common Childhood Infections
Practice Questions
Pediatric HIV
Practice Questions
Congenital Infections
Practice Questions
Fever in Infants and Children
Practice Questions
Meningitis and Encephalitis
Practice Questions
Respiratory Tract Infections
Practice Questions
Gastrointestinal Infections
Practice Questions
Parasitic Infections
Practice Questions
Tuberculosis in Children
Practice Questions
Opportunistic Infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
