Infectious Diseases — MCQs

On this page
Which of the following symptoms is NOT suggestive of Scarlet fever?
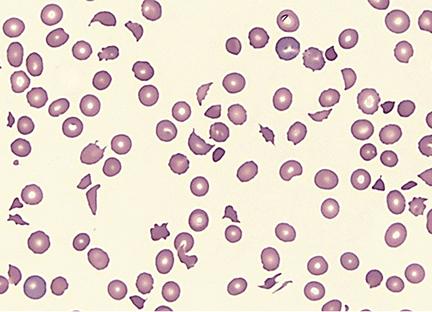
A 2-year-old child in shock presents with multiple non-blanching purple lesions of various sizes scattered on the trunk and extremities. Petechiae are noted, and oozing from the venipuncture site has been observed. The child's peripheral blood smear is shown below. Clotting studies are likely to show which of the following?
At what age is Streptococcus pneumoniae pneumonia most commonly present?
A neonate presents with periventricular calcifications on CT scan of the brain. What is the most appropriate diagnostic method for the suspected etiological agent?
Which of the following statements regarding typhoid in children is false?
A 3-year-old female child presented with low-grade fever, poor feeding, and a rash described as a 'slapped cheek' rash. Which of the following is the predominant site of action of the causative organism?
Which of the following acts as a means of transmission of HIV infection in a newborn?
In rubella syndrome, all are seen except?
A 4-year-old girl with a history of hydrocephalus presents with severe headache and fever. She underwent surgery for a ventricular-peritoneal shunt 2 months ago. The neurologist suspects an infection. Which organism would most likely be isolated from the shunt tubing?
What management is indicated for an infant born to an HIV-positive mother?
Practice by Chapter
Vaccine-Preventable Diseases
Practice Questions
Immunization Schedule
Practice Questions
Common Childhood Infections
Practice Questions
Pediatric HIV
Practice Questions
Congenital Infections
Practice Questions
Fever in Infants and Children
Practice Questions
Meningitis and Encephalitis
Practice Questions
Respiratory Tract Infections
Practice Questions
Gastrointestinal Infections
Practice Questions
Parasitic Infections
Practice Questions
Tuberculosis in Children
Practice Questions
Opportunistic Infections
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
