Secondary Immunodeficiency Disorders — MCQs

AIDS, secondary infection will be all except
CD40 deficiency in a person signifies?
Which of the following methods is NOT recommended for the diagnosis of HIV infection in a 2-month-old child?
With the lack of CD40 in B cells, which immunological abnormality is seen?
Which of the following is not a complication of Congenital Rubella Syndrome (CRS)?
According to WHO, the major clinical sign of HIV infection in children in stage 1 is the following.
Given the immunologic abnormalities of normal serum IgG, normal serum IgA, normal serum IgM, decreased T-cell function, and decreased parathyroid function, which clinical presentation is most likely?
Best method to diagnose HIV in an infant?
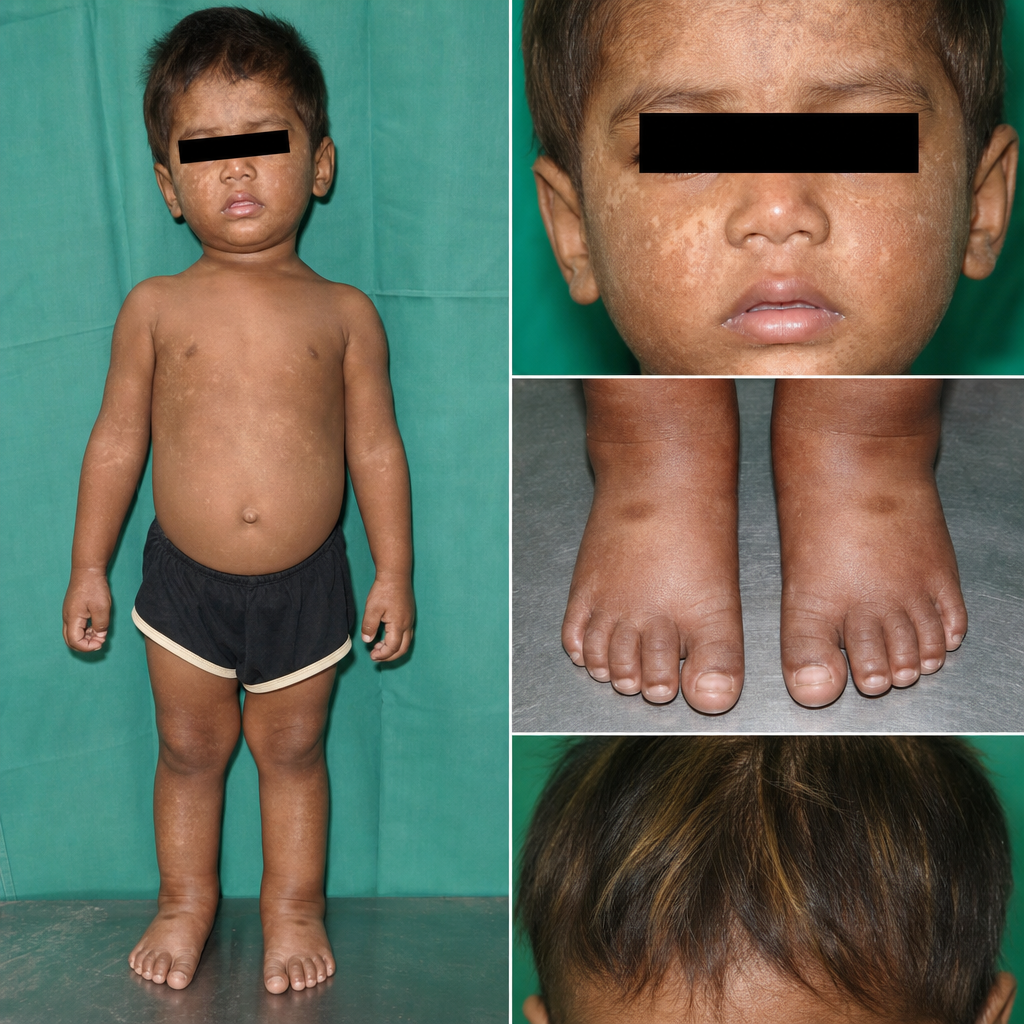
A 2.5-year-old boy is brought to the nutrition clinic. He was born at term with a birth weight of 3.0 kg. His mother reports that since weaning he has been fed almost exclusively on a maize-based porridge with minimal animal protein or legumes. On examination, he weighs 9.8 kg and has a height of 82 cm. He has bilateral pitting oedema up to the ankles, generalised skin changes with areas of hyperpigmentation and hypopigmentation, and hair that shows alternating light and dark bands. Serum albumin is 1.8 g/dL. Haemoglobin is 8.2 g/dL. Stool microscopy shows no parasites. Which of the following biochemical profiles is most consistent with this child's nutritional disorder?
What is a characteristic feature of Systemic Juvenile Idiopathic Arthritis?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
