Immunology and Allergies — MCQs

On this page
A 3-year-old male presents with a skin rash and epistaxis. He has experienced several severe sinopulmonary infections. A careful history reveals that his maternal uncle died of bleeding complications following an emergency cholecystectomy. What additional findings are likely in this case?
Which of the following is a characteristic of Henoch-Schonlein Purpura?
Abdominal pain in Henoch-Schonlein purpura is most commonly due to which of the following mechanisms?
A child presents with recurrent Staphylococcus infections. Laboratory examination shows very low levels of immunoglobulins (G, A, M, E), and a low quantity of B cells. There is a normal reaction to environmental antigens on the skin. What is the most likely diagnosis?
A 9-month-old child was admitted to ICU with a history of recurrent sinusitis and otitis media by Staphylococcus aureus. Blood test shows decreased serum IgA, IgG, IgM, IgE, and plasma B cells. What is the diagnosis?
Which of the following vaccines is contraindicated in a patient of Severe Combined Immunodeficiency (SCID)?
A 6-month-old infant presents with recurrent infections and failure to thrive. Laboratory investigations reveal a deficiency of adenosine deaminase (ADA). Which of the following immunodeficiency disorders is most likely associated?
A 5-year-old short stature boy presented with fever and weight loss for 6 weeks. He has been admitted previously for 4 episodes of pneumonia in last year. On examination neck lymph nodes were enlarged and reddish macules were noticed on the face and forehead. Lymph node biopsy shows Hodgkin's disease. What is the diagnosis?
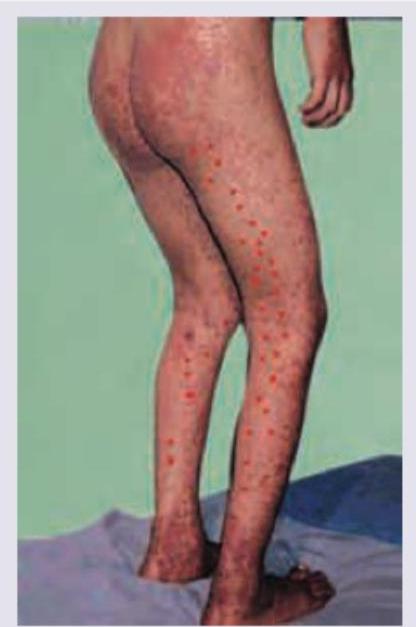
A 7-year-old boy presents with palpable non-blanching rash starting 3 days back from the ankles and involves lower limbs and buttocks. He had viral URTI previously. BP is normal and KFT is normal. What is the diagnosis?
A 6-year-old child with abdominal pain and a rash is shown. Comment on the diagnosis?
Practice by Chapter
Development of Immune System
Practice Questions
Primary Immunodeficiency Disorders
Practice Questions
Secondary Immunodeficiency Disorders
Practice Questions
Allergic Rhinitis
Practice Questions
Asthma in Children
Practice Questions
Atopic Dermatitis
Practice Questions
Food Allergies
Practice Questions
Drug Allergies
Practice Questions
Anaphylaxis
Practice Questions
Urticaria and Angioedema
Practice Questions
Autoimmune Disorders
Practice Questions
Immunotherapy
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
