Immunology and Allergies — MCQs

On this page
A child presents with blotchy rash on legs, back and buttocks. All are true about the condition except:
Which of the following are causes of secondary immunodeficiency in children? I. Diphenylhydantoin II. Severe malnutrition III. Post-varicella state IV. Nephrotic syndrome Select the correct answer using the code given below :
Eight months old child had history of unusual crying and convulsions following previous vaccination after BCG, DPT & OPV ( first dose), and Hepatitis B. Now parents have brought child for next doses of vaccination. Which vaccine is contraindicated in this situation?
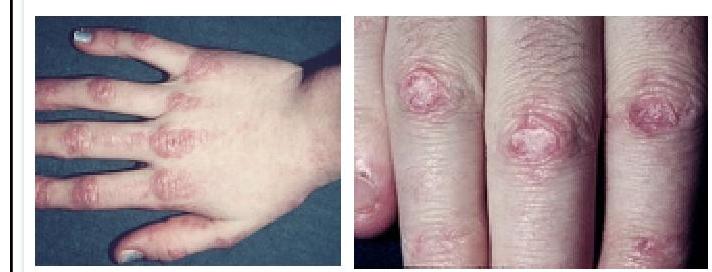
A 10-year-old boy presents with fever, joint pain, and a lesion over his hand, as seen in the image below. Which of the following is the clinical finding, and what is the likely diagnosis?
In which of the following disorders, vaccines are not contraindicated in the person suffering from that disease?
A 10 year old male child presents with purpuric rashes on the lower extremities, hematuria, abdominal pain, and arthritis but has no history of fever. What is the likely diagnosis ?
All are common features of juvenile idiopathic arthritis EXCEPT
Pauciarticular JRA is characterized by all except:
Which of the following is not true about Juvenile rheumatoid arthritis?
A 3-month-old with recurrent infections and no thymus shadow has lymphopenia. What is the most likely enzyme deficiency?
Practice by Chapter
Development of Immune System
Practice Questions
Primary Immunodeficiency Disorders
Practice Questions
Secondary Immunodeficiency Disorders
Practice Questions
Allergic Rhinitis
Practice Questions
Asthma in Children
Practice Questions
Atopic Dermatitis
Practice Questions
Food Allergies
Practice Questions
Drug Allergies
Practice Questions
Anaphylaxis
Practice Questions
Urticaria and Angioedema
Practice Questions
Autoimmune Disorders
Practice Questions
Immunotherapy
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
