Food Allergies — MCQs

A man had Egg omelet 1-4 hours back and developed diarrhea, vomiting and abdominal cramps. Most likely cause of poisoning is
Which type of dermatitis is evaluated through patch testing?
A man takes peanut and develops tongue swelling, neck swelling, stridor, hoarseness of voice. What is the probable diagnosis?
In chronic allergy, which Ig is more persistent in the body?
A 45-year-old patient with a known allergy to penicillin presents with an enterococcal endocarditis. The physician needs to prescribe an antibiotic but wants to ensure it is safe for a penicillin allergy. The patient has had previous allergic reactions to penicillin including rash & swelling. Which of the following drugs can be used safely in a patient allergic to penicillin?
Drug of choice for Enterococcus infection in a patient allergic to penicillin?
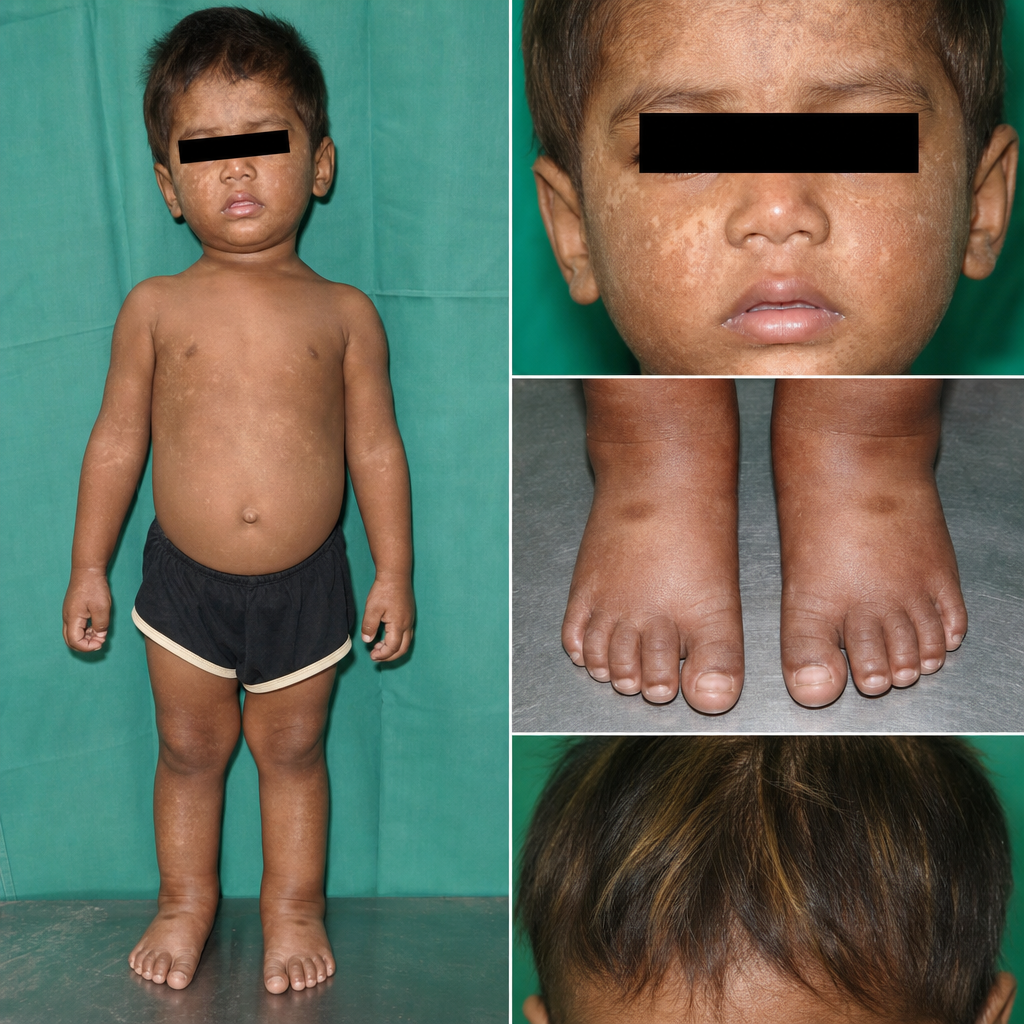
A 2.5-year-old boy is brought to the nutrition clinic. He was born at term with a birth weight of 3.0 kg. His mother reports that since weaning he has been fed almost exclusively on a maize-based porridge with minimal animal protein or legumes. On examination, he weighs 9.8 kg and has a height of 82 cm. He has bilateral pitting oedema up to the ankles, generalised skin changes with areas of hyperpigmentation and hypopigmentation, and hair that shows alternating light and dark bands. Serum albumin is 1.8 g/dL. Haemoglobin is 8.2 g/dL. Stool microscopy shows no parasites. Which of the following biochemical profiles is most consistent with this child's nutritional disorder?
What is a characteristic feature of Systemic Juvenile Idiopathic Arthritis?
An 8-year-old child has had abdominal pain and dark urine for 10 days. Physical examination shows blotchy purple skin lesions on the trunk and extremities. Urinalysis shows hematuria and proteinuria. Serologic test results are negative for myeloperoxidase-antineutrophil cytoplasmic antibody (MPO-ANCA) and proteinase 3-antineutrophil cytoplasmic antibody (PR3-ANCA). A skin biopsy specimen shows necrotizing vasculitis of small dermal vessels. A renal biopsy specimen shows immune complex deposition in glomeruli, with some IgA-rich immune complexes. Which of the following is the most likely diagnosis?
A child presents with delayed separation of the umbilical cord, leukocytosis, Down syndrome, and recurrent infections. What is the most likely diagnosis?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
