Growth and Development — MCQs

On this page
Birth weight of a newborn baby doubles by which age?
A child typically climbs stairs at what age?
Which of the following developmental milestones is NOT typically achieved by 13 months of age?
Which of the following is considered a red flag sign in a child's development if not attained?
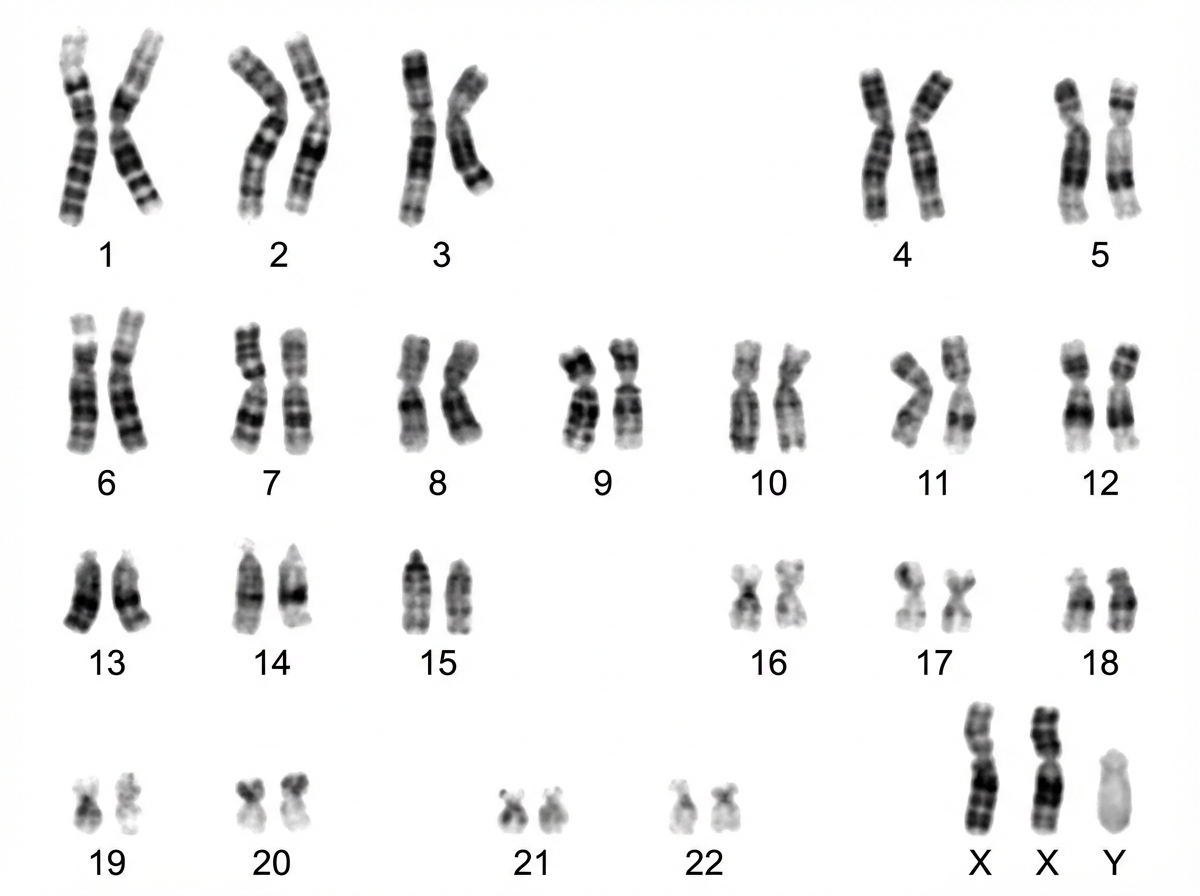
Which of the following chromosomal abnormalities is indicated by the chromosomal mapping?
What is a sternocleidomastoid tumor?
Short stature is defined as a height below which percentile?
Which of the following reflexes are present at birth?
Which X-ray view is used to determine bone age in a 3-year-old child?
A mother brings her 3-year-old female child complaining that the child is not eating. Her weight is 11 kg (50th percentile) and height is 88 cm (75th percentile). What should be done next?
Practice by Chapter
Normal Growth Parameters
Practice Questions
Developmental Milestones
Practice Questions
Puberty and Adolescent Development
Practice Questions
Growth Disorders
Practice Questions
Failure to Thrive
Practice Questions
Developmental Screening and Assessment
Practice Questions
Developmental Delays
Practice Questions
Growth Charts and Monitoring
Practice Questions
Short Stature
Practice Questions
Tall Stature
Practice Questions
Precocious and Delayed Puberty
Practice Questions
Psychosocial Development
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
