Growth and Development — MCQs

On this page
What is the best indicator of acute malnutrition?
Which artery is best to palpate for a pulse in infants?
At what age do the first set of milk teeth typically appear?
What is the most common cardiovascular lesion in Down syndrome?
Class III malocclusion is seen in all of the following conditions except?
What is an age-appropriate motor skill for a 1.5-year-old child?
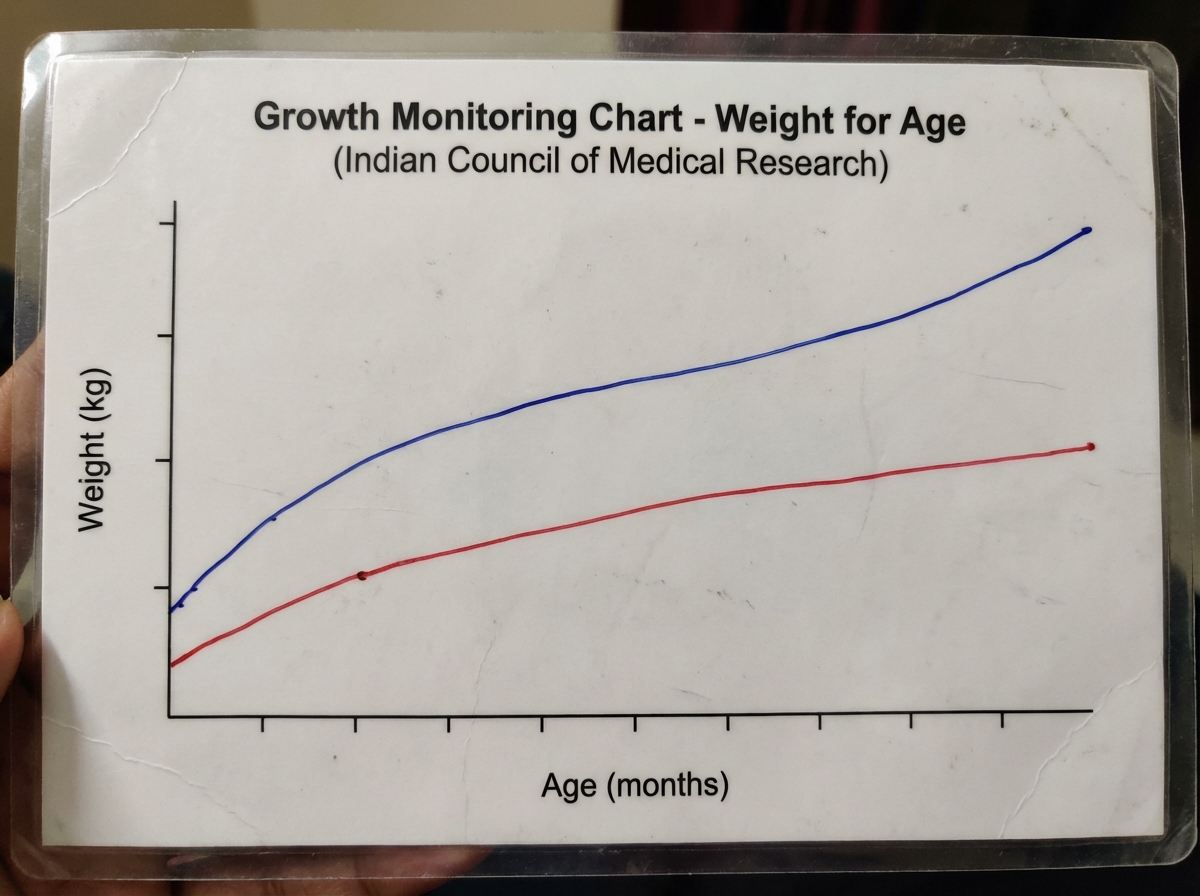
The uppermost line of the card depicted above is equivalent to:
A newborn baby has a head circumference of 35 cm at birth. What will be the optimal head circumference at 6 months of age?
Mr. and Mrs. Annadurai have a 2-month-old baby with Down syndrome. The karyotype of Mrs. Annadurai shows a translocation variety of Down syndrome. Which of the following investigations would you advise to the parents before their next pregnancy?
Which of the following is a sign of puberty in boys?
Practice by Chapter
Normal Growth Parameters
Practice Questions
Developmental Milestones
Practice Questions
Puberty and Adolescent Development
Practice Questions
Growth Disorders
Practice Questions
Failure to Thrive
Practice Questions
Developmental Screening and Assessment
Practice Questions
Developmental Delays
Practice Questions
Growth Charts and Monitoring
Practice Questions
Short Stature
Practice Questions
Tall Stature
Practice Questions
Precocious and Delayed Puberty
Practice Questions
Psychosocial Development
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
