Growth and Development — MCQs

On this page
The following clinical features are seen in which disease?
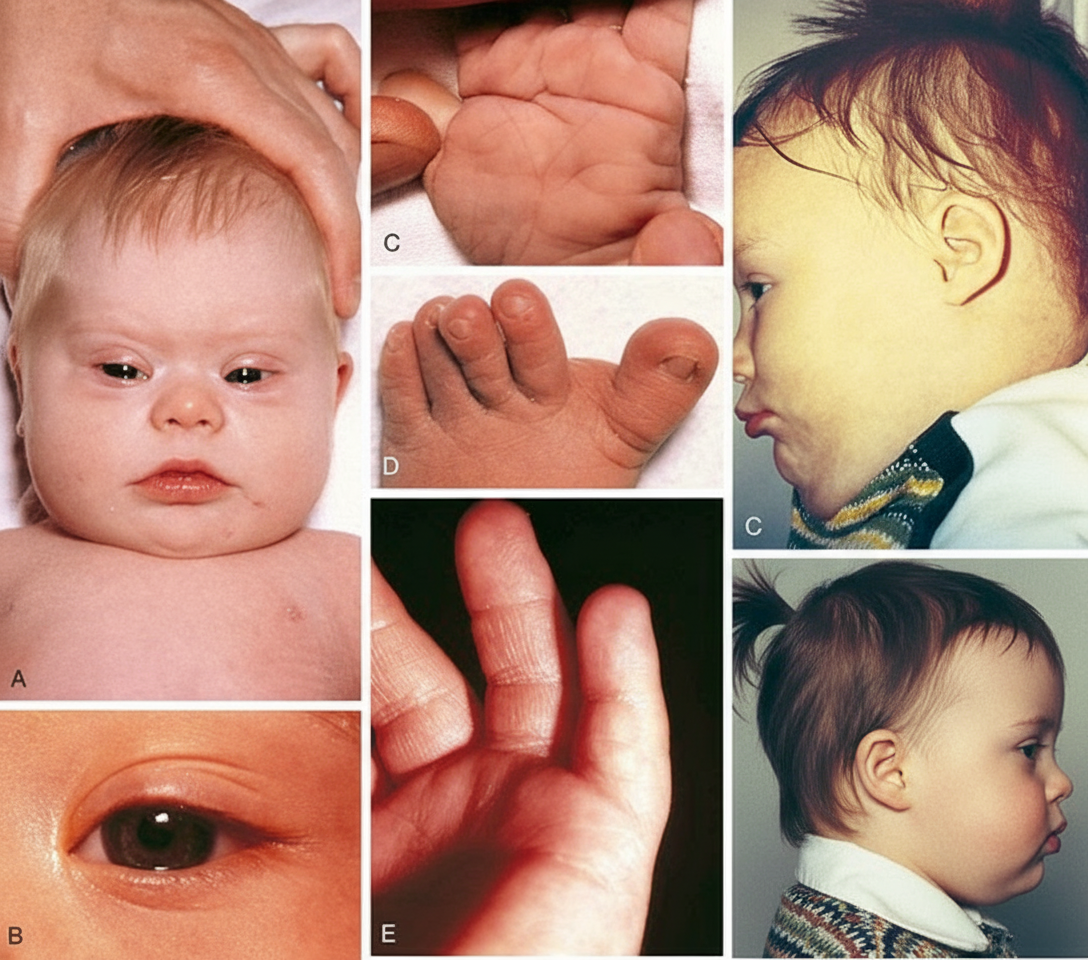
What is the normal respiratory rate in a child less than 2 months old?
All of the following are true statements about Down syndrome, except:
Which of the following reflexes is not present at birth?
At what age does a child's intracellular fluid (ICF) and extracellular fluid (ECF) composition become similar to that of an adult?
Delayed dentition is usually considered when there are no teeth by what age?
By what age do teeth typically begin to erupt in primary dentition?
The behaviour therapeutic falls in the management of enuresis. What is the pharmacological drug of choice for this case?
Which of the following is NOT a guideline for immunization against infectious diseases?
A baby placed in the prone position is able to lift the head and upper chest on extended arms by what age?
Practice by Chapter
Normal Growth Parameters
Practice Questions
Developmental Milestones
Practice Questions
Puberty and Adolescent Development
Practice Questions
Growth Disorders
Practice Questions
Failure to Thrive
Practice Questions
Developmental Screening and Assessment
Practice Questions
Developmental Delays
Practice Questions
Growth Charts and Monitoring
Practice Questions
Short Stature
Practice Questions
Tall Stature
Practice Questions
Precocious and Delayed Puberty
Practice Questions
Psychosocial Development
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
