Growth and Development — MCQs

On this page
Persistence of the following beyond 6 months of age indicates what?
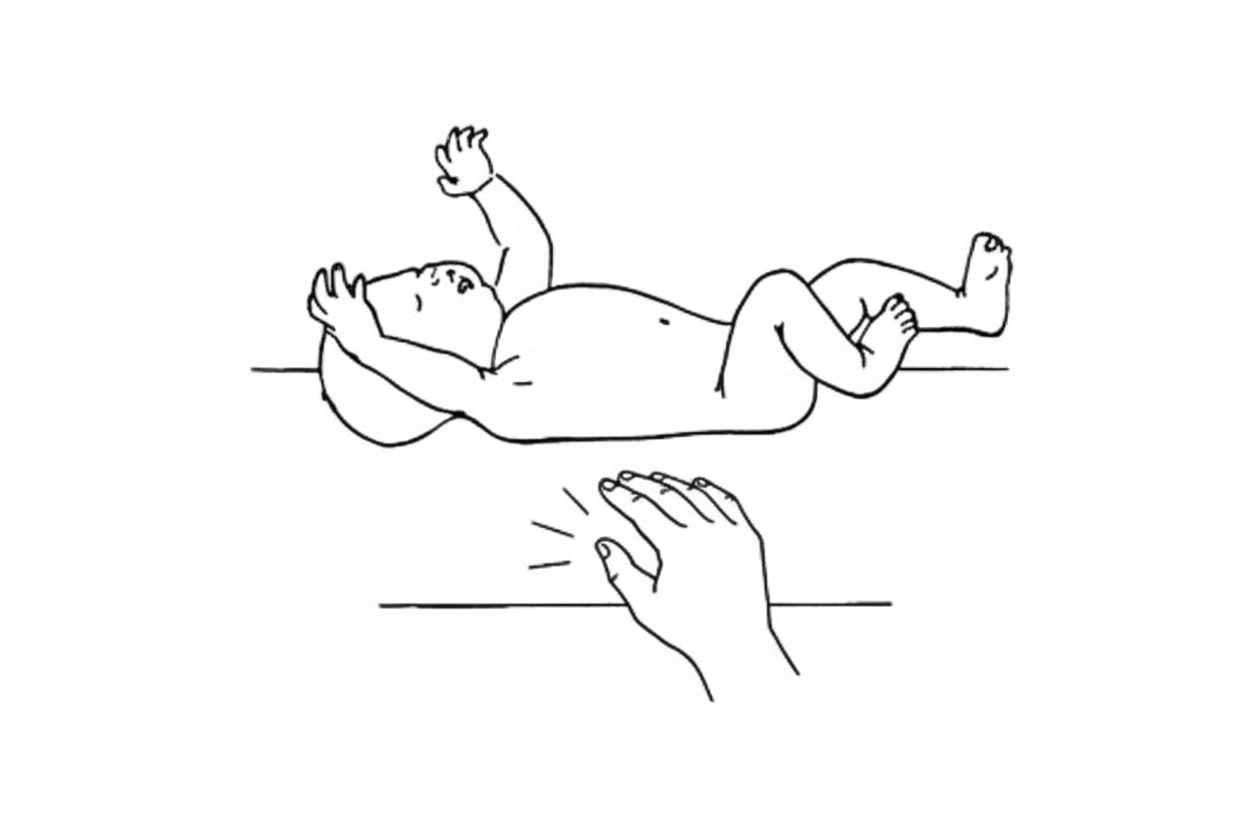
A child presents with short stature. What is a potential underlying cause?
A 4-year-old girl, who was underweight and hypotonic in infancy, is obsessed with food, eats compulsively, and is already grossly overweight. She is argumentative, oppositional, and rigid. She has a narrow face, almond-shaped eyes, and a small mouth. What is her diagnosis?
The period of mixed dentition is typically between which ages?
A normal infant sits briefly leaning forward on her hands, reaches for and grasps a cube, and transfers it from hand to hand. She babbles but cannot wave bye-bye, nor can she grasp objects with the finger and thumb. What is her approximate age?
When does the child first attain the milestone of sitting without support?
A 6-year-old patient presents with a greenish-blue swelling distal to a deciduous second molar. What is the most appropriate management?
What is the most common cause of short stature?
Which of the following statements is true about dentition?
Which of the following is NOT true about Edward syndrome (Trisomy 18)?
Practice by Chapter
Normal Growth Parameters
Practice Questions
Developmental Milestones
Practice Questions
Puberty and Adolescent Development
Practice Questions
Growth Disorders
Practice Questions
Failure to Thrive
Practice Questions
Developmental Screening and Assessment
Practice Questions
Developmental Delays
Practice Questions
Growth Charts and Monitoring
Practice Questions
Short Stature
Practice Questions
Tall Stature
Practice Questions
Precocious and Delayed Puberty
Practice Questions
Psychosocial Development
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
