Growth and Development — MCQs

On this page
Which of the following conditions is X-linked recessive?
A child who can ride a tricycle and uses alternate steps while climbing stairs has attained a developmental age of:
A 12-month-old baby who is growing well and developing normally is noted to have a single transverse palmar crease (simian crease). Which of the following is a true statement regarding this finding?
Which of the following developmental milestones is typically NOT achieved by 1 year of age?
What is the mean head circumference at birth?
What is the time taken for air to reach the descending colon in a normal infant?
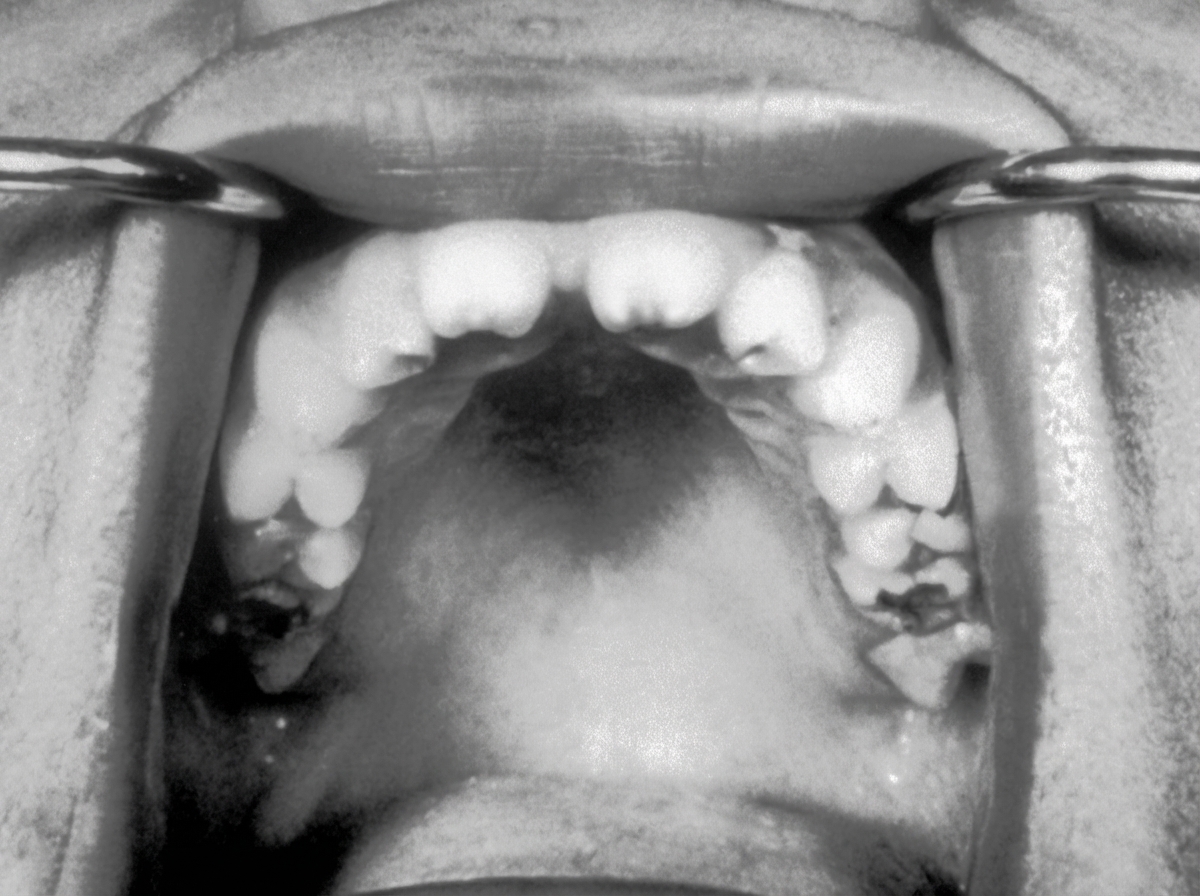
The teeth abnormality shown in the image is seen in which of the following diseases?
Pseudoparalysis in an infant is suggestive of which of the following conditions?
A child climbs with alternate steps, builds a tower of 8-9 cubes, tells 'I' but cannot say their name or age and sex. What is the probable age of this child?
What is the normal uterine-cervix ratio up to 10 years of age?
Practice by Chapter
Normal Growth Parameters
Practice Questions
Developmental Milestones
Practice Questions
Puberty and Adolescent Development
Practice Questions
Growth Disorders
Practice Questions
Failure to Thrive
Practice Questions
Developmental Screening and Assessment
Practice Questions
Developmental Delays
Practice Questions
Growth Charts and Monitoring
Practice Questions
Short Stature
Practice Questions
Tall Stature
Practice Questions
Precocious and Delayed Puberty
Practice Questions
Psychosocial Development
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
