Growth and Development — MCQs

On this page
In the WHO 'Road to Health' card, what does the upper reference line represent?
In WHO growth charts, what does the 'Lower reference curve' represent?
At what age can a child typically kick a ball?
At what age can a child typically identify their gender?
Megalencephaly is commonly seen in which of the following conditions?
Which of the following statements is true regarding the serology of rickets?
What is the name of the device used to measure subscapular skin fold thickness?
At what age can a child play a simple ball game?
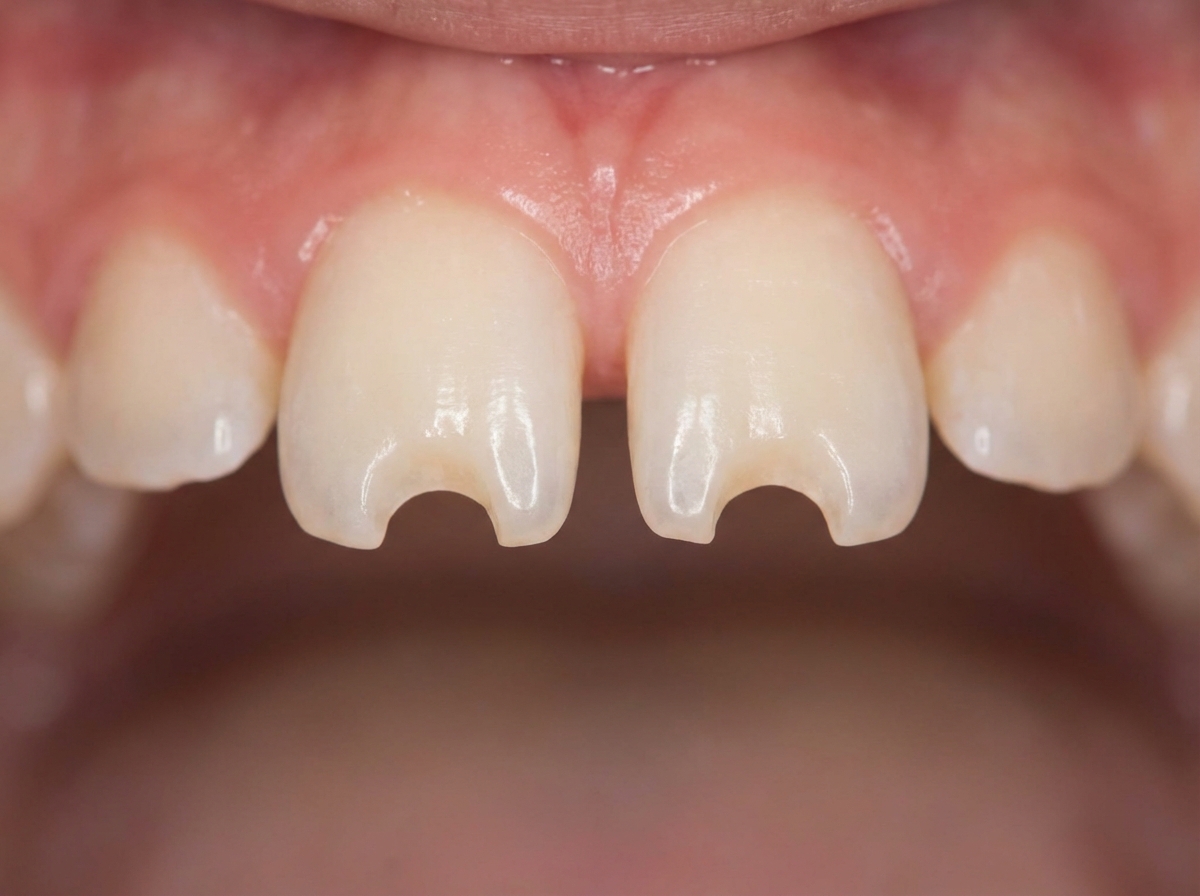
What is this teeth abnormality?
A child can typically withhold and postpone bowel movements voluntarily starting at approximately what age?
Practice by Chapter
Normal Growth Parameters
Practice Questions
Developmental Milestones
Practice Questions
Puberty and Adolescent Development
Practice Questions
Growth Disorders
Practice Questions
Failure to Thrive
Practice Questions
Developmental Screening and Assessment
Practice Questions
Developmental Delays
Practice Questions
Growth Charts and Monitoring
Practice Questions
Short Stature
Practice Questions
Tall Stature
Practice Questions
Precocious and Delayed Puberty
Practice Questions
Psychosocial Development
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
