Growth and Development — MCQs

On this page
Early epiphyseal closure is seen with _________?
Which of the following complications has been associated with the adverse effects of rotavirus vaccine?
Juene syndrome is characterized by which mode of inheritance?
A baby can hold their neck and sit with support, but cannot sit without support. What is the typical age of this baby?
Delayed dentition with multiple supernumerary teeth is seen in which of the following conditions?
What is the approximate water content of breast milk?
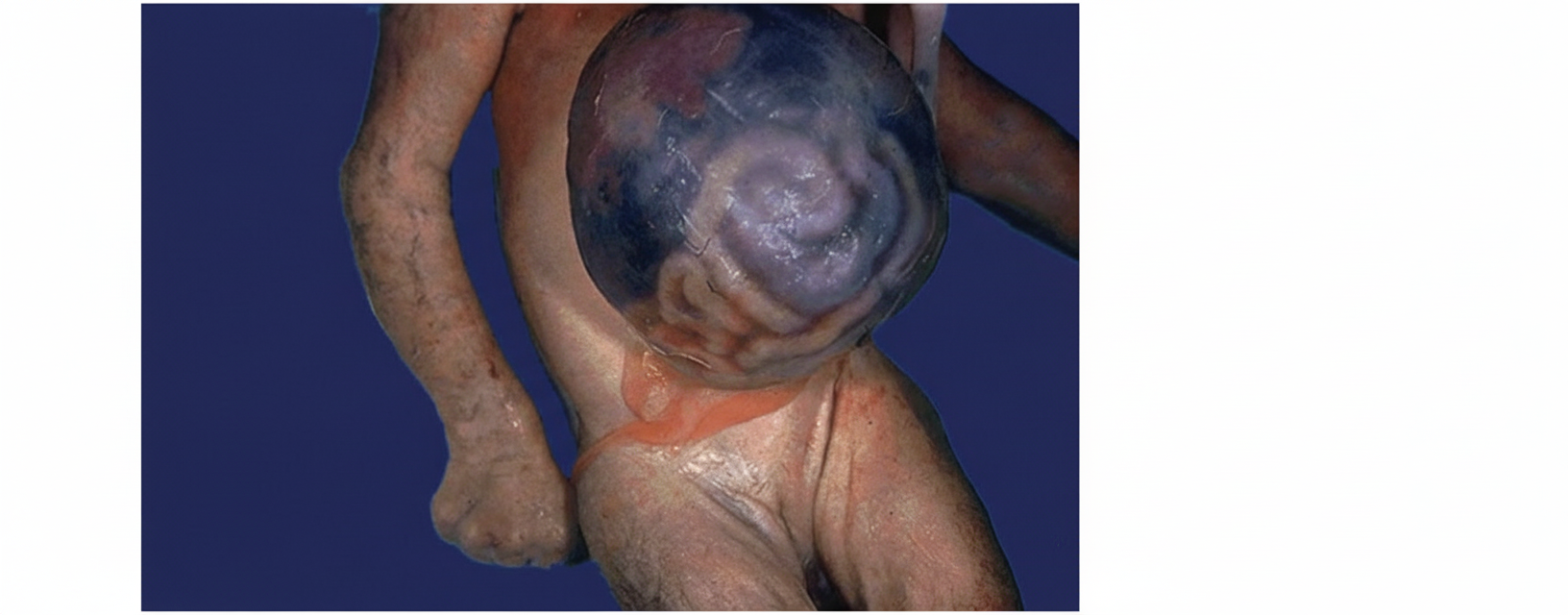
A neonate is found to have a condition as shown in the image. Which of the following is a common associated anomaly?
Down's syndrome is most commonly caused by?
How many teeth are typically present in a 3-year-old child?
At what age does handedness typically develop?
Practice by Chapter
Normal Growth Parameters
Practice Questions
Developmental Milestones
Practice Questions
Puberty and Adolescent Development
Practice Questions
Growth Disorders
Practice Questions
Failure to Thrive
Practice Questions
Developmental Screening and Assessment
Practice Questions
Developmental Delays
Practice Questions
Growth Charts and Monitoring
Practice Questions
Short Stature
Practice Questions
Tall Stature
Practice Questions
Precocious and Delayed Puberty
Practice Questions
Psychosocial Development
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
