Growth and Development — MCQs

On this page
In which stage of puberty does growth spurt occur in girls?
What is the primary use of a measuring tape in pediatrics?
At what age does temporary dentition usually begin?
Craniotabes (softening of the skull bones) is NOT seen in which of the following conditions?
What is the most sensitive indicator of depletion of intravascular volume in an infant?
The Simian crease is not seen in which of the following conditions?
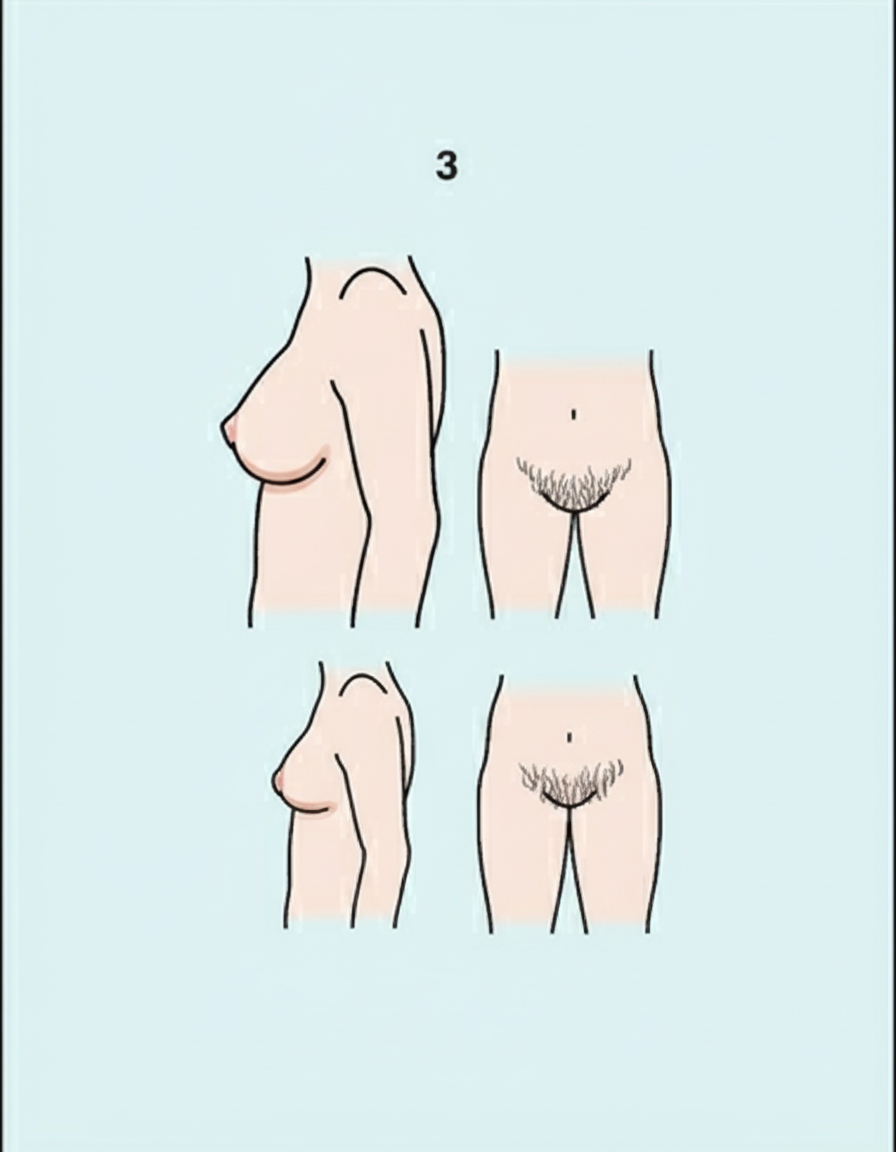
What is the Tanner-Whitehouse (SMR) staging based on the following findings in a female?
What is the following device used to measure?

You are examining an infant and the findings are as follows: Adductor angle - 100°, Popliteal angle - 90°, Dorsiflexion angle of foot - 70°, Scarf sign - Elbow crosses the middle but doesn't reach the anterior axillary line. What is the appropriate age of the infant?
In severe acute malnutrition, what is the defined blood glucose level for hypoglycemia?
Practice by Chapter
Normal Growth Parameters
Practice Questions
Developmental Milestones
Practice Questions
Puberty and Adolescent Development
Practice Questions
Growth Disorders
Practice Questions
Failure to Thrive
Practice Questions
Developmental Screening and Assessment
Practice Questions
Developmental Delays
Practice Questions
Growth Charts and Monitoring
Practice Questions
Short Stature
Practice Questions
Tall Stature
Practice Questions
Precocious and Delayed Puberty
Practice Questions
Psychosocial Development
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
