Growth and Development — MCQs

On this page
All of the following statements are true regarding principles of development except?
Head control/neck holding is possible in an infant by which age?
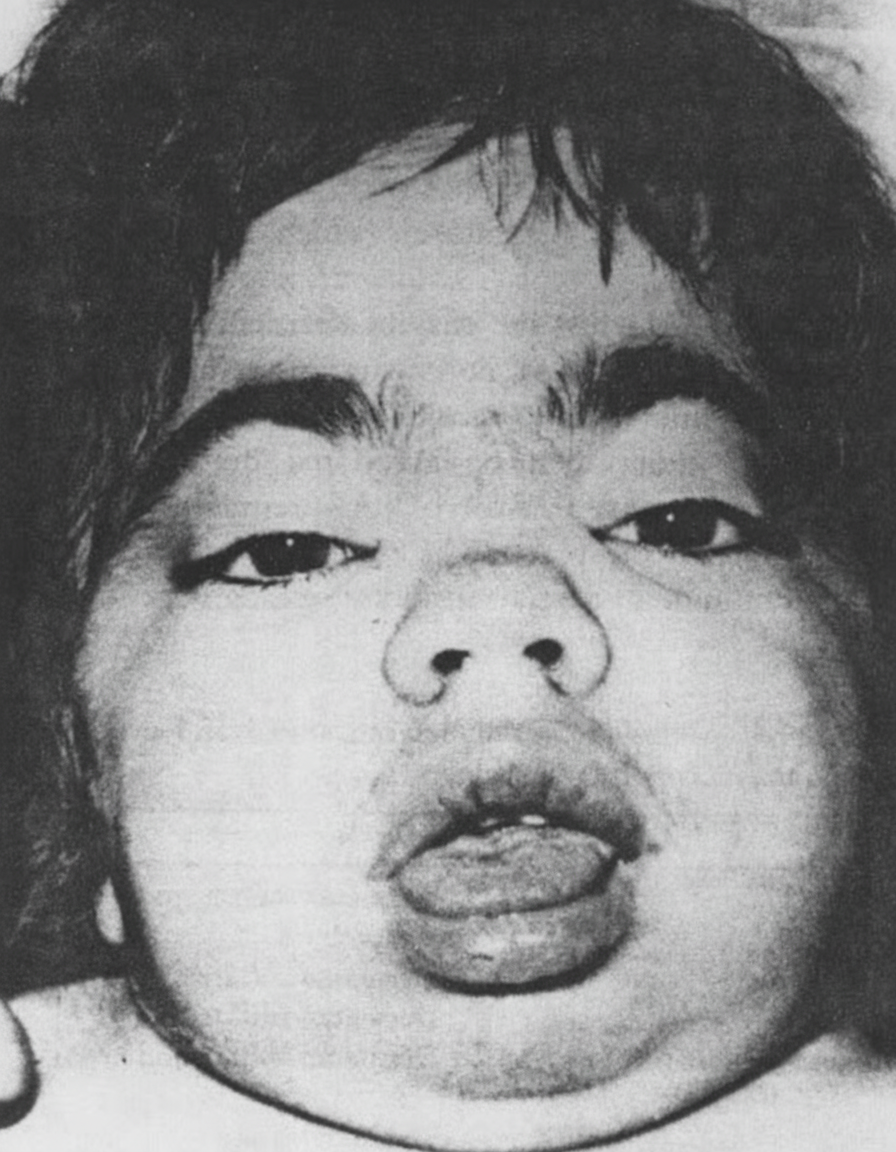
What is the disease this child, who also has hepatosplenomegaly and intellectual disability, is suffering from?
Waterlow classification of malnutrition in children takes into account which of the following parameters?
A child draws a person with 2-4 body parts besides the head at the age of _________
Wide open anterior fontanelle is found in which of the following conditions?
What is the inheritance pattern of dentinogenesis imperfecta?
Which of the following classifications or indices does not include height?
A 14-year-old presents with primary amenorrhea. On examination, she has breast development and normal pubic hair growth. Which of the following best describes the normal sequence of pubertal changes in a female?
Which of the following childhood disorders typically improves with age?
Practice by Chapter
Normal Growth Parameters
Practice Questions
Developmental Milestones
Practice Questions
Puberty and Adolescent Development
Practice Questions
Growth Disorders
Practice Questions
Failure to Thrive
Practice Questions
Developmental Screening and Assessment
Practice Questions
Developmental Delays
Practice Questions
Growth Charts and Monitoring
Practice Questions
Short Stature
Practice Questions
Tall Stature
Practice Questions
Precocious and Delayed Puberty
Practice Questions
Psychosocial Development
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
