Failure to Thrive — MCQs

A 5-year-old has the following anthropometry findings: Weight/age < -3.2 SD, Height/age < -2.5 SD, Weight/height < -1.7 SD. What is the most likely diagnosis?
What is the maintenance fluid requirement in a 6 kg child ?
Organic causes of constipation in infants include all of the following EXCEPT:
Which is true about an infant with failure to thrive and the following findings?
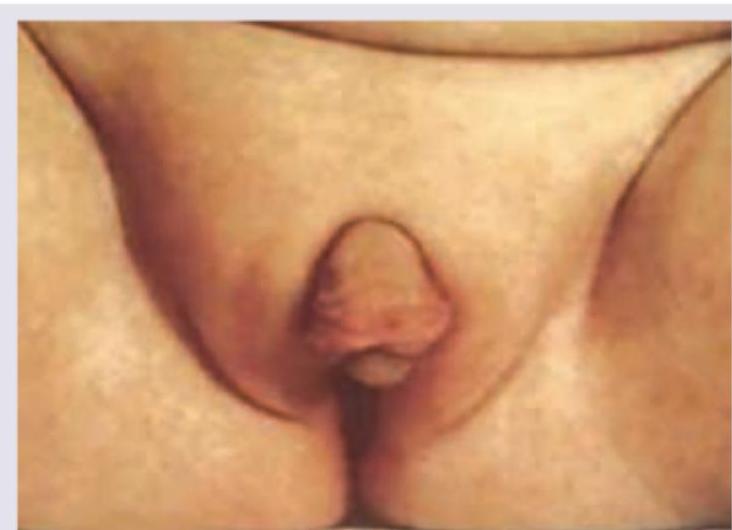
Which of the following is NOT a feature of HIV infection in childhood -
Most common symptom of HIV infection in infants is:
A child presented at 10 weeks with recurrent episode of pneumonia and failure to thrive. X-ray shows cardiomegaly & pulmonary plethora. What is the diagnosis?
A 1-month old baby present with frequent vomiting and failure to thrive. There are features of moderate dehydration. Blood sodium in 122 mEq/l and potassium is 6.1 mEq/l. The most likely diagnosis is?
At what age can a child typically laugh aloud?
At what age can a child typically count 4 pennies accurately?
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
