Gastroenterology — MCQs

On this page
An 8-year-old child is referred with a history of mononeuritis multiplex and hepatosplenomegaly. Examination of the oral cavity and pharynx revealed enlarged orange-colored tonsils. Which of the following statements regarding this condition is false?
A 23-year-old woman, G2, P1, gave birth at term to a boy of normal weight and length following an uncomplicated pregnancy. The infant initially did well, but at 6 weeks, he began feeding poorly for 1 week, and his mother noticed that much of the milk he ingested was forcefully vomited within 1 hour. Now, on physical examination, the infant is afebrile, and there are no external anomalies. A midabdominal mass is palpable. Bowel sounds are active. The medical history indicates that both the mother and her first child had the same illness during infancy. Which of the following conditions is most likely to explain these findings?
A 6-year-old girl presents with constipation, abdominal distention, and vomiting. She is diagnosed with Hirschsprung disease (aganglionic megacolon), a congenital condition leading to colon dilation. This condition is caused by the absence of which of the following kinds of neural cell bodies?
A 6-month-old baby presents with a history of bloody diarrhea for 2 days and abdominal distension. On examination, the baby screams. What is the most likely diagnosis?
A 12-year-old boy presented with abdominal pain. What is the most likely diagnosis?
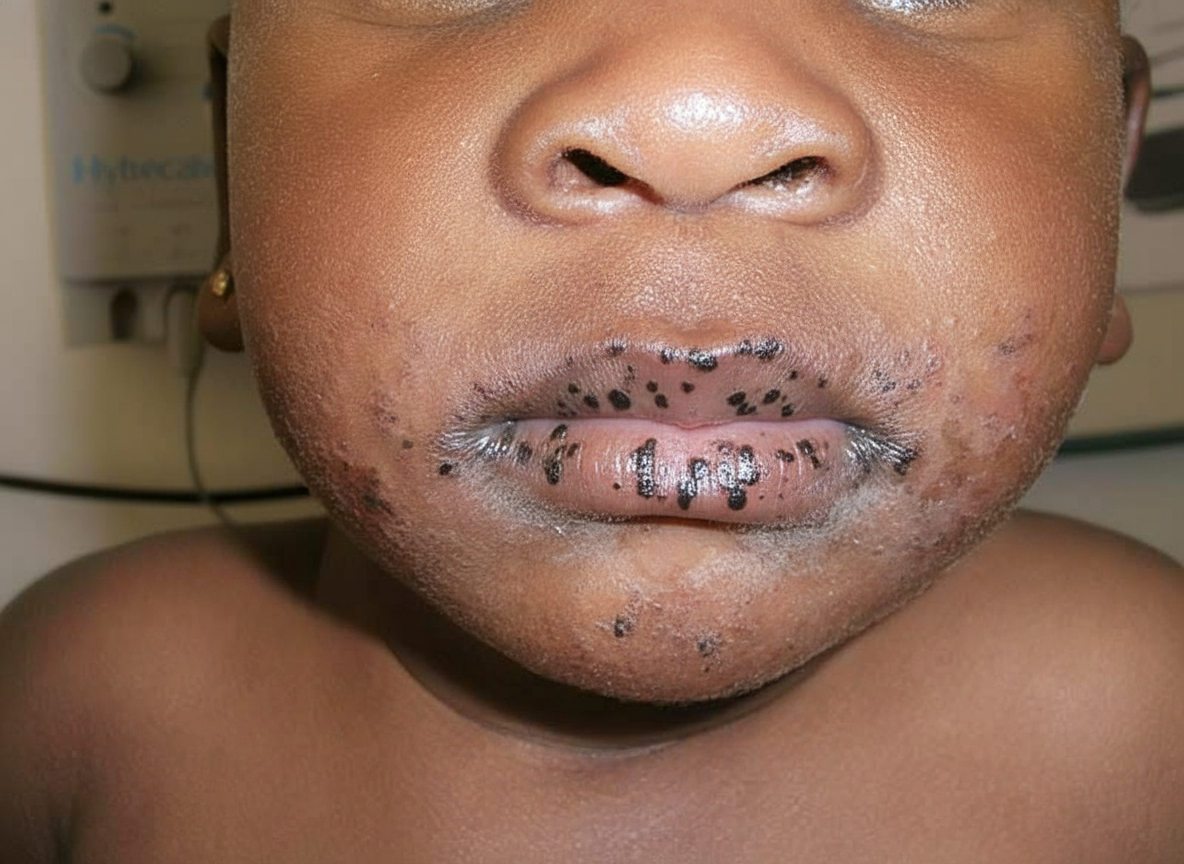
What are the differential diagnoses for a left-sided abdominal mass in a baby?
Which of the following is NOT true about Intussusception?
Which of the following is the most sensitive indicator of intravascular volume depletion in an infant presented with acute rotavirus gastroenteritis?
Reye's syndrome is characterized by which of the following findings?
In necrotizing enterocolitis, what is the earliest change seen on X-ray abdomen?
Practice by Chapter
Gastroesophageal Reflux
Practice Questions
Peptic Ulcer Disease
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Celiac Disease
Practice Questions
Malabsorption Syndromes
Practice Questions
Acute and Chronic Diarrhea
Practice Questions
Constipation and Encopresis
Practice Questions
Gastrointestinal Bleeding
Practice Questions
Intestinal Obstruction
Practice Questions
Liver Diseases in Children
Practice Questions
Pancreatic Disorders
Practice Questions
Pediatric Nutritional Support
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
