Gastroenterology — MCQs

On this page
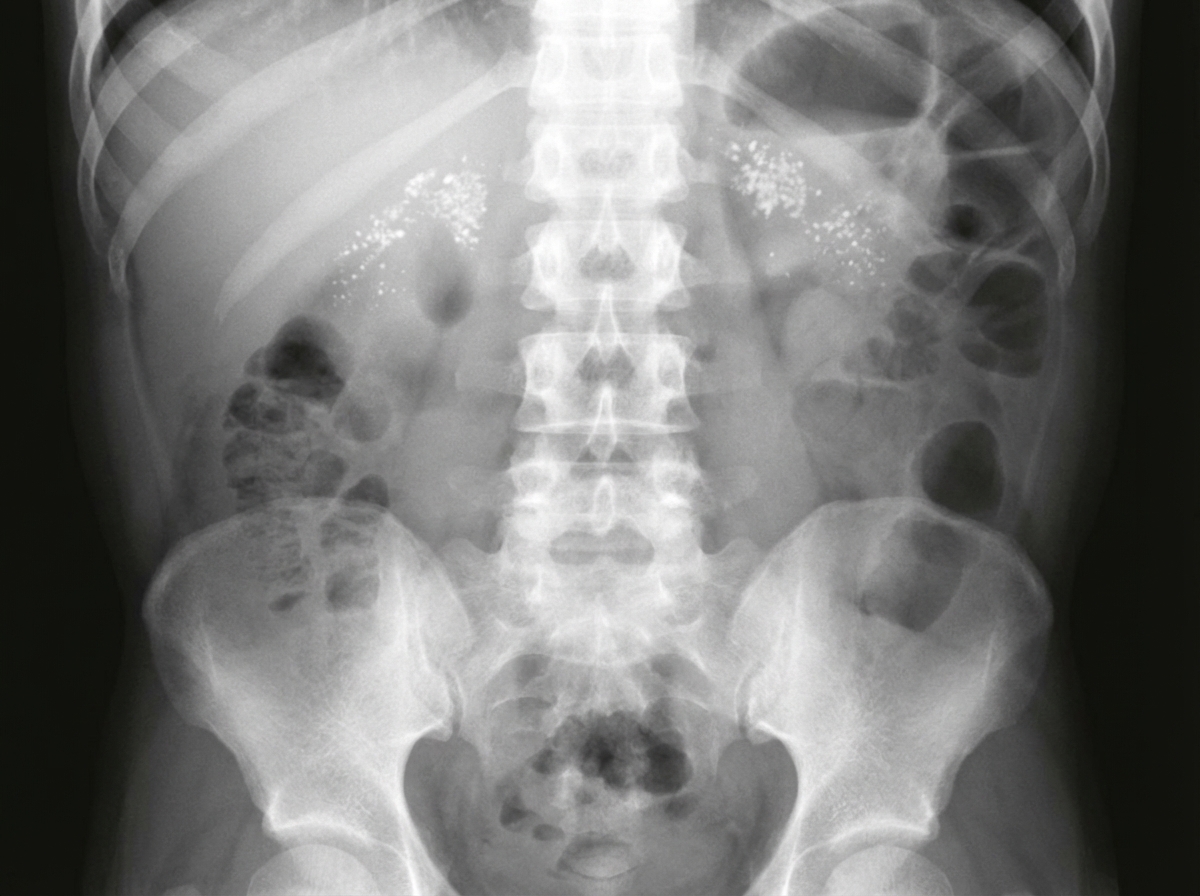
An infant presents with failure to thrive and abdominal distension. His X-ray chest and abdomen showed findings suggestive of a diagnosis. What is the diagnosis?
What is the osmolarity of ORS fluid?
What is an anomaly associated with duodenal atresia?
Which of the following statements regarding Hirschsprung's disease is true?
Which of the following conditions can cause conjugated hyperbilirubinemia in infancy?
A 5-year-old boy presented with massive hematemesis. He is not febrile. Per abdominal examination revealed massive splenomegaly without hepatomegaly. What is the most probable diagnosis?
A 14-year-old male presents with left-sided upper abdominal pain and massive splenomegaly. Two years prior, he experienced massive hematemesis and was diagnosed with Extrahepatic Portal Venous Obstruction (EHPVO), for which he underwent ligation of esophageal varices. What is the likely diagnosis?
Use of antibiotics in a child with diarrhea is indicated in all of the following situations except?
What is the commonest cause of intestinal obstruction in Down's syndrome?
Cystic fibrosis is associated with:
Practice by Chapter
Gastroesophageal Reflux
Practice Questions
Peptic Ulcer Disease
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Celiac Disease
Practice Questions
Malabsorption Syndromes
Practice Questions
Acute and Chronic Diarrhea
Practice Questions
Constipation and Encopresis
Practice Questions
Gastrointestinal Bleeding
Practice Questions
Intestinal Obstruction
Practice Questions
Liver Diseases in Children
Practice Questions
Pancreatic Disorders
Practice Questions
Pediatric Nutritional Support
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
