Gastroenterology — MCQs

On this page
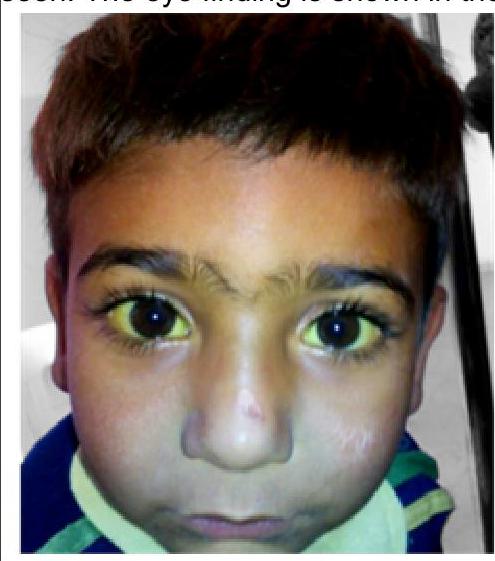
An 11-year-old boy was brought to the outpatient clinic with intention tremor and poor scholastic performance. His sister has similar complaints. On examination, hepatomegaly is seen. The eye finding is shown in the image. What is the probable diagnosis?
Acquired megacolon in children is most commonly due to-
In a child, which of the following diseases is commonly misdiagnosed as appendicitis?
A baby with diarrhea presented with restlessness but is able to drink water. Skin turgor goes back in 2 seconds. The baby is communicating properly. What is the best management?
Most common cause of significant lower GI bleeding (hematochezia) in children is
Exocrine pancreatic insufficiency is seen in:
Organic causes of constipation in infants include all of the following EXCEPT:
Congenital pyloric stenosis causes: 1. Bilious vomiting 2. Non-bilious vomiting 3. Projectile vomiting 4. Non-projectile vomiting 5. Forceful vomiting
6 year old drowsy child came in emergency with history of vomiting, loose motion for 3 days. On examination he had sunken eye, hypothermia, skin on pinching takes time to revert. Diagnosis
The most common congenital esophageal anomaly is which of the following?
Practice by Chapter
Gastroesophageal Reflux
Practice Questions
Peptic Ulcer Disease
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Celiac Disease
Practice Questions
Malabsorption Syndromes
Practice Questions
Acute and Chronic Diarrhea
Practice Questions
Constipation and Encopresis
Practice Questions
Gastrointestinal Bleeding
Practice Questions
Intestinal Obstruction
Practice Questions
Liver Diseases in Children
Practice Questions
Pancreatic Disorders
Practice Questions
Pediatric Nutritional Support
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
