Gastroenterology — MCQs

On this page
All of the following statements regarding this image are true except:
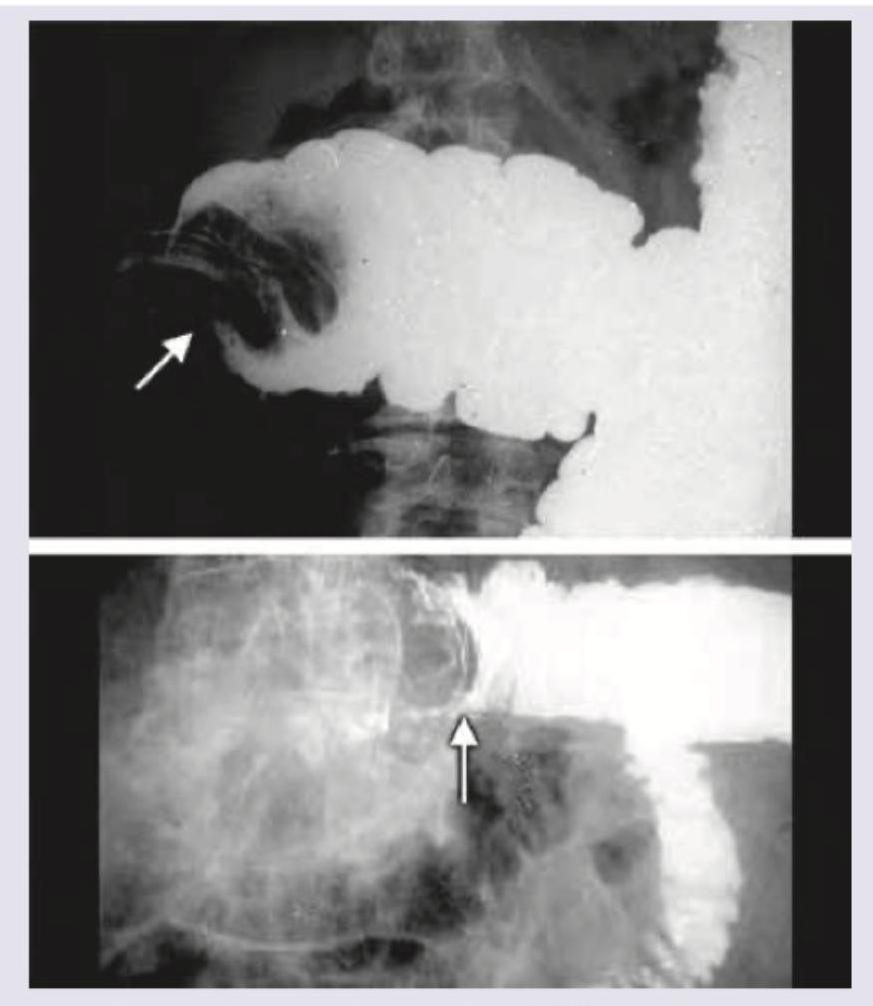
A baby presents with colicky abdominal pain. Mother gives a history of bloody stools. All the statements regarding this condition are true except:
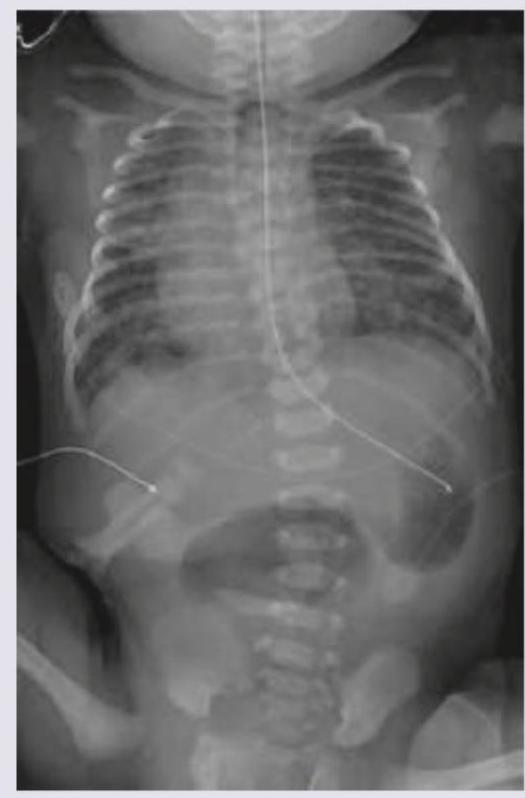
A baby on day 4 of its birth presents with repeated vomiting. The vomiting is bilious in nature. What is the most possible diagnosis as per the infantogram?
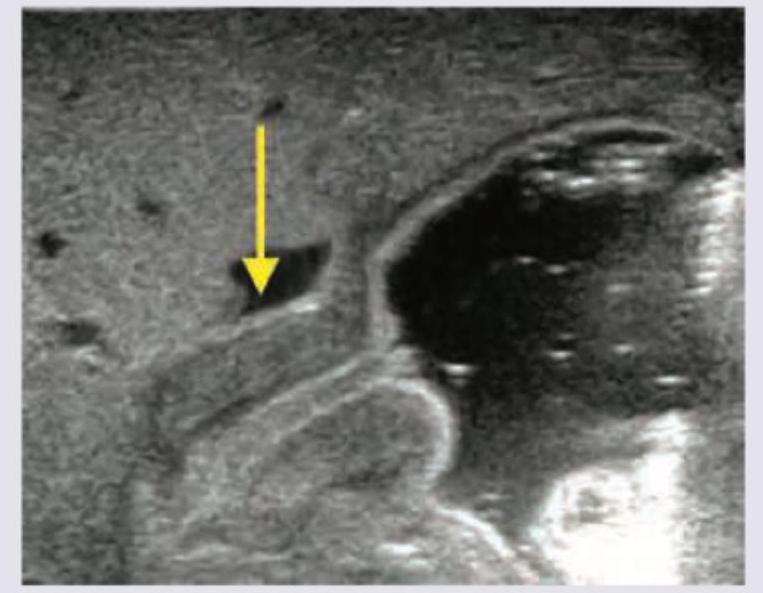
Neonate is brought at 3 weeks of age, with projectile vomiting. USG was performed and is shown below. When can the abdominal mass in this condition be best palpated?
USG abdomen of a 9-month-old child as shown below denotes:
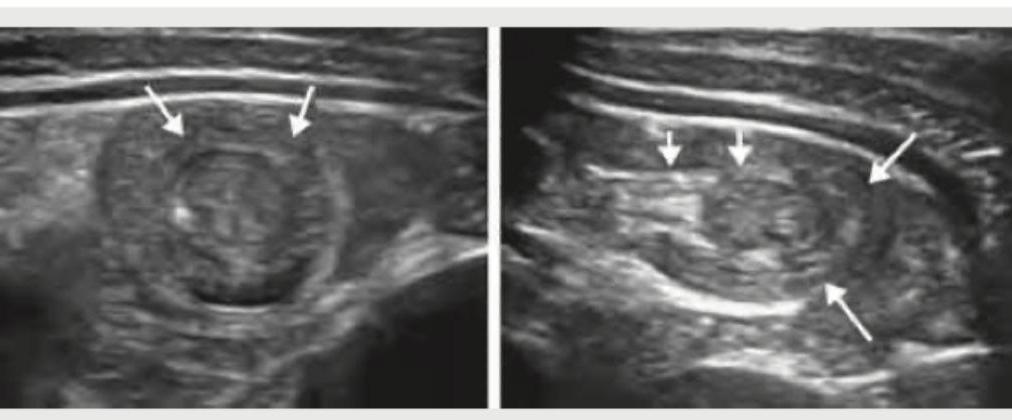
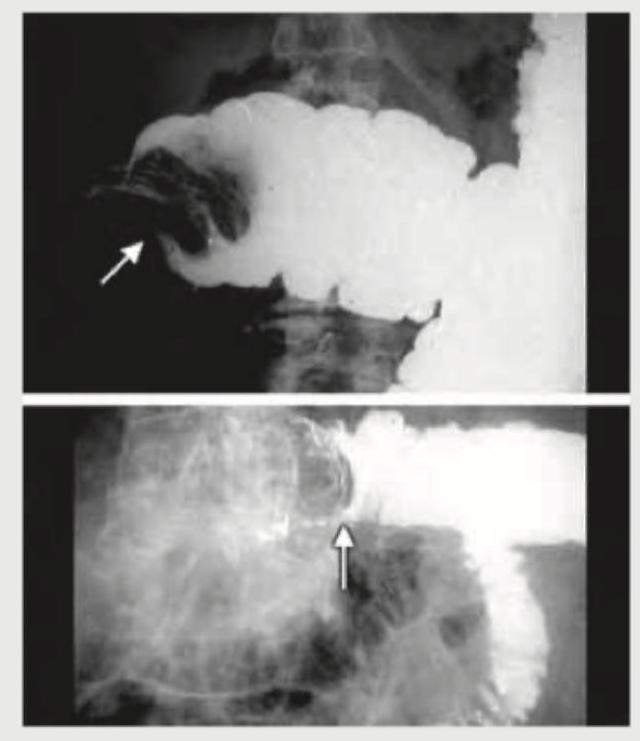
All of the following statements regarding this image are true except: (Recent NEET Pattern 2016-17)
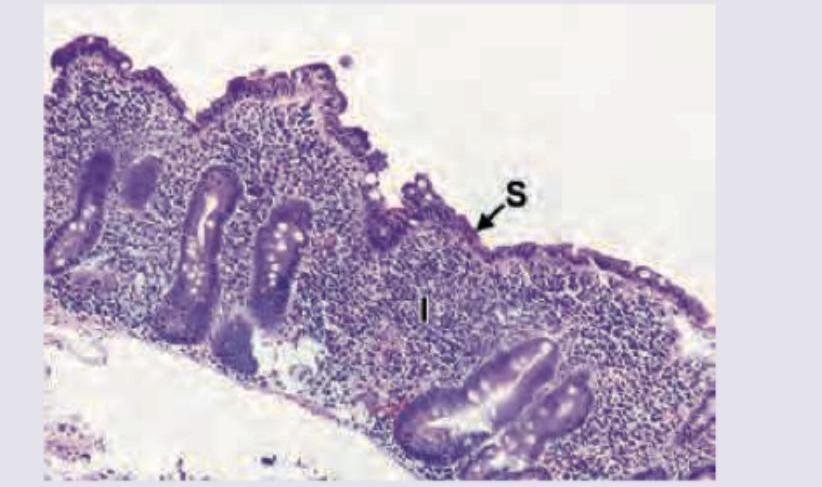
One-year-old child with failure to thrive and diarrhea. On examination anemia and puffy eyes are noted. Intestinal biopsy was performed. All are true about the condition shown except:
Which of the following statements are correct regarding the management of gastrointestinal bleeding in children? I. Somatostatin or octreotide infusion should be given for at least 7 days after stoppage of initial bleeding to prevent rebleeding II. Endoscopic Sclerotherapy (EST) involves endoscopic injection of N -butyl-2-cyanoacrylate or iso-butyl-2-cyanoacrylate III. EST has upto 90 % efficacy in controlling acute bleeding IV. Following an episode of acute variceal bleeding, all patients should receive secondary prophylaxis to prevent rebleeding Select the answer using the code given below :
Consider the following features: 1. Visible gastric peristalsis 2. Bilious vomiting 3. Palpable tumour 4. Melena Which of these is/are feature/features of infantile hypertrophic pyloric stenosis?
An eight month old male child is brought to the emergency with recurrent episodes of screaming and drawing up of legs. The child appears to be listless in between the attacks. Local examination of abdomen reveals feeling of emptiness in the right iliac fossa and blood stained mucus is found on the finger on rectal examination. The most probable clinical diagnosis in this child is
Practice by Chapter
Gastroesophageal Reflux
Practice Questions
Peptic Ulcer Disease
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Celiac Disease
Practice Questions
Malabsorption Syndromes
Practice Questions
Acute and Chronic Diarrhea
Practice Questions
Constipation and Encopresis
Practice Questions
Gastrointestinal Bleeding
Practice Questions
Intestinal Obstruction
Practice Questions
Liver Diseases in Children
Practice Questions
Pancreatic Disorders
Practice Questions
Pediatric Nutritional Support
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
