Gastroenterology — MCQs

On this page
A child with diarrhea was eager to drink, and the skin pinch went back slowly. Which of the following categories is the child classified into as per IMNCI?
A 2-week-old infant presents with high conjugated (direct) bilirubin, dark-colored urine, and clay-colored stools. On examination, the infant appears jaundiced, but is feeding normally. What is the most likely diagnosis?
A child presents with abdominal distension and an enlarged liver by 8cm below the costal margin. The liver is smooth on palpation. Which of the following is the most likely diagnosis?
A 5 year old boy presented with hematemesis and was found to have splenomegaly, on examination. There was a past history of exchange transfusion in this child for neonatal jaundice. What is the probable diagnosis?
A child was brought to the casualty with complaints of vomiting and loose stools with a history of laxative use. On examination, arrhythmia is present. What will be the abnormality present?
A child has elevated liver enzyme levels. A ring-like structure is noted on ocular examination. Which of the following is the cause for this?
Which of the following is not true about CHPS? CHPS - Congenital hypertrophic pyloric stenosis
A 2-month-old infant presents with projectile non-bilious vomiting after each feeding for the past week, weight loss, and constant hunger. On examination, a firm, olive-shaped mass is palpable in the right upper quadrant. Serum electrolytes show hypochloremic hypokalemic metabolic alkalosis. What is the definitive treatment?
A 6-week-old infant presents with a history of non-bilious, non-projectile vomiting starting at 3 weeks of age. The infant's abdominal examination is normal. Which of the following is the most likely diagnosis?
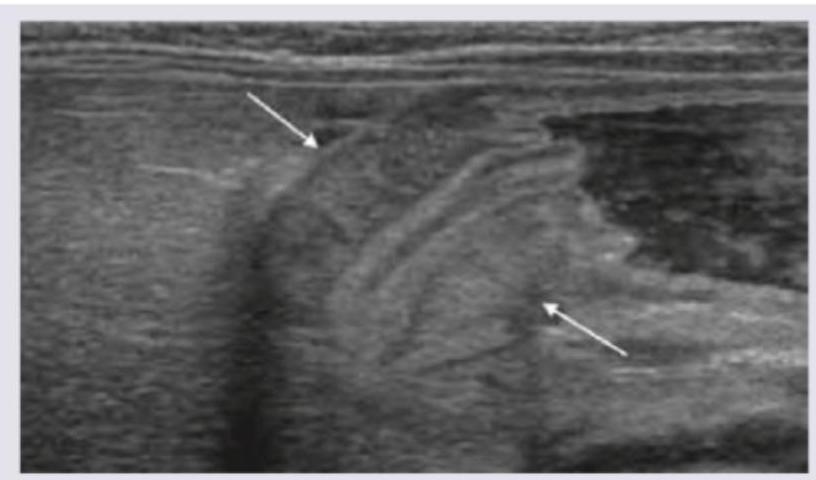
A 4-week-old baby presents with non-bilious vomiting and abdominal distension. The radiological image is shown. Among the clinical features, which is the most essential finding in reaching the diagnosis of this condition?
Practice by Chapter
Gastroesophageal Reflux
Practice Questions
Peptic Ulcer Disease
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Celiac Disease
Practice Questions
Malabsorption Syndromes
Practice Questions
Acute and Chronic Diarrhea
Practice Questions
Constipation and Encopresis
Practice Questions
Gastrointestinal Bleeding
Practice Questions
Intestinal Obstruction
Practice Questions
Liver Diseases in Children
Practice Questions
Pancreatic Disorders
Practice Questions
Pediatric Nutritional Support
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
