Gastroenterology — MCQs

On this page
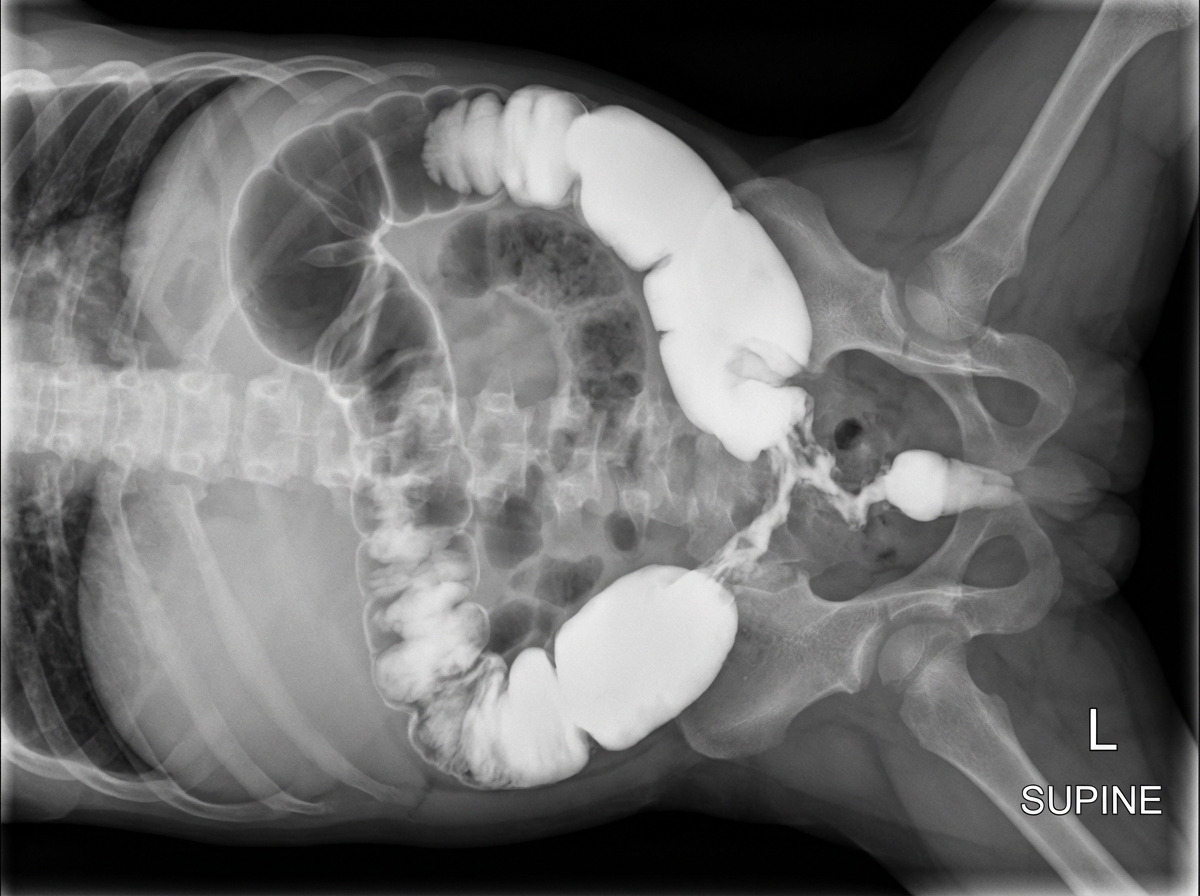
A 5-day-old term male neonate presents with delayed passage of meconium, abdominal distension, and bilious vomiting. Barium enema and intestinal biopsy findings are shown. What is the diagnosis?
What is the composition of Low Osmolar Oral Rehydration Solution (ORS)?
What is the most common genetic cause of liver disease in children?
A neonate presents with a distended abdomen and failure to pass meconium. Which of the following conditions can be ruled out?
Which of these disorders in neonates can best be excluded or diagnosed by anorectal manometry?
A 10-year-old male child presents with a 2-day history of pain in the left hypochondrium. His Hb is 9.69%. His mother reports episodes of passing black-colored stools occurring 7 days prior and on 2-3 occasions over the past 2 years. During these episodes, he experienced fatigability while playing and was unable to keep up with his peers. Which of the following findings will be most helpful in arriving at a clinical diagnosis?
What is the least common site of volvulus in children?
A 2-year-old child presented with hepatomegaly. Which of the following is NOT a potential cause?
A 8-year-old child has a history since early childhood of malabsorption, ataxia, acanthocytes in the peripheral blood, and very low cholesterol and triglyceride levels. In addition, the patient has been developing progressive, bilateral, concentric contraction of the visual fields and loss of central vision. What is the underlying pathogenesis of this patient's disease?
The passage of 'red currant jelly' stools in an infant is characteristic of which condition?
Practice by Chapter
Gastroesophageal Reflux
Practice Questions
Peptic Ulcer Disease
Practice Questions
Inflammatory Bowel Disease
Practice Questions
Celiac Disease
Practice Questions
Malabsorption Syndromes
Practice Questions
Acute and Chronic Diarrhea
Practice Questions
Constipation and Encopresis
Practice Questions
Gastrointestinal Bleeding
Practice Questions
Intestinal Obstruction
Practice Questions
Liver Diseases in Children
Practice Questions
Pancreatic Disorders
Practice Questions
Pediatric Nutritional Support
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
