Endocrinology — MCQs

On this page
A five-year-old boy presents with coarse facial features, mental retardation, and dysostosis multiplex. Corneal clouding is absent. What is the diagnosis?
Which of the following is NOT true about Turner syndrome?
What is the most common cause of precocious puberty?
A female neonate with DiGeorge syndrome develops severe muscle cramps and convulsions soon after birth. Which of the following is the cause of convulsions in this neonate?
In children with type 1 diabetes mellitus, when is ophthalmologic evaluation indicated?
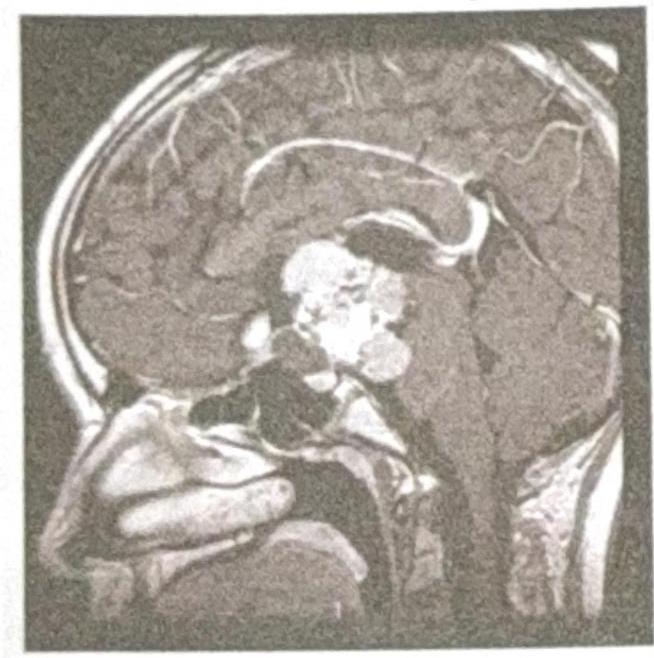
A 9-year-old female child presents with a history of headache and visual disturbances. What is the most likely diagnosis?
Which disease affects only the formation and eruption of teeth but does not cause hypoplasia?
A 2-year-old intellectually disabled child has blue eyes, blonde hair, and fair skin, along with a peculiar body odor. What is the diagnosis?
In children, which is the most commonly recognized form of familial hyperlipidemia?
A 14-year-old boy presents with a 3-month history of increasing weakness, easy fatigability, and weight loss. He also reports recent onset of nausea, vomiting, and abdominal pain. His blood pressure is markedly decreased, and he has increased pigmentation of his skin creases. What is the most likely diagnosis?
Practice by Chapter
Disorders of Growth
Practice Questions
Thyroid Disorders
Practice Questions
Disorders of Puberty
Practice Questions
Adrenal Disorders
Practice Questions
Diabetes Mellitus in Children
Practice Questions
Disorders of Calcium and Phosphate Metabolism
Practice Questions
Disorders of Sexual Development
Practice Questions
Hypoglycemia
Practice Questions
Obesity and Metabolic Syndrome
Practice Questions
Pituitary Disorders
Practice Questions
Multiple Endocrine Neoplasia Syndromes
Practice Questions
Endocrine Emergencies
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
