Developmental and Behavioral Pediatrics — MCQs

On this page
At what age does the transfer of one object to another hand happen?
A 9-month-old child is brought to OPD with developmental concerns. The child cannot sit without support, says "dada" and "mama", and has stranger anxiety. What is the appropriate management?
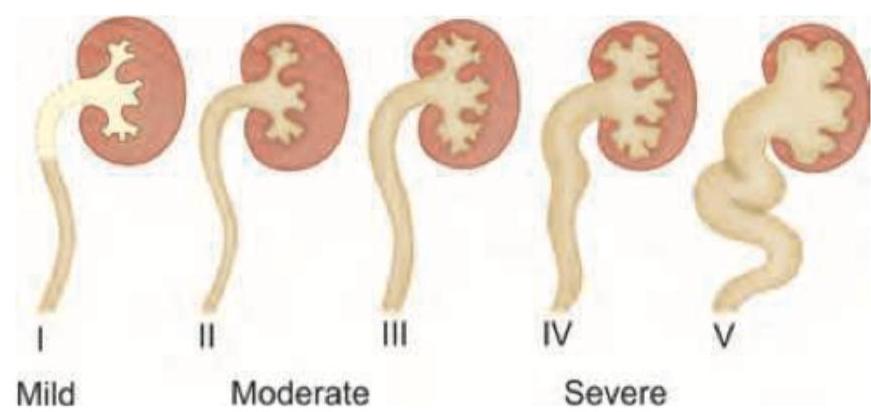
Comment on the diagnosis of this child with hypoactive deep tendon reflexes and reduced range of movement at all joints:
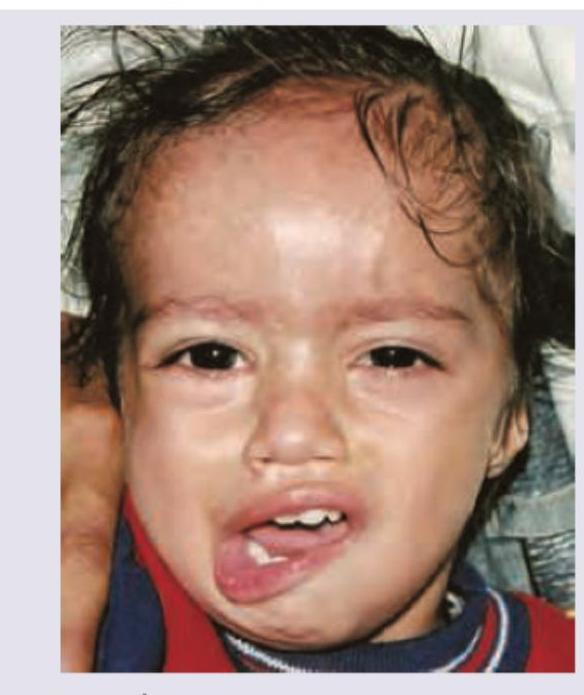
The picture depicts characteristic facial features of a child including a long face, prominent forehead, large ears, and prominent jaw. This disorder is also associated with intellectual disability, autistic behavior, and macroorchidism. Which syndrome is being described?
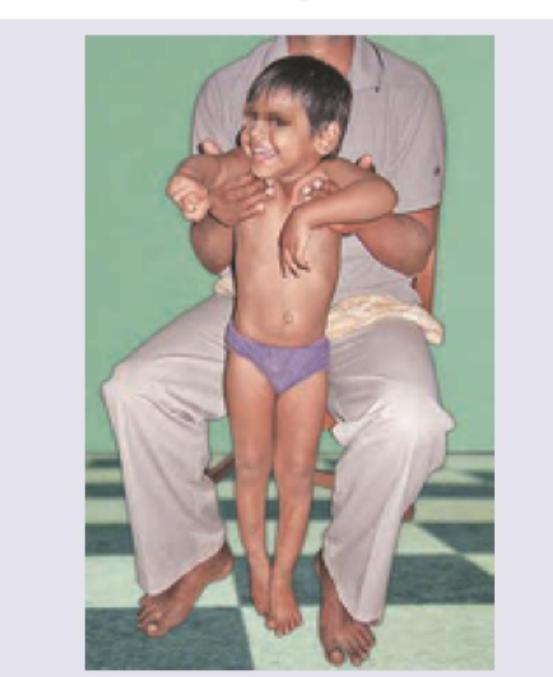
A child is having difficulty standing up from a sitting position and uses a characteristic maneuver shown in the image below. What is the most likely diagnosis?
The child can do this activity at which age?

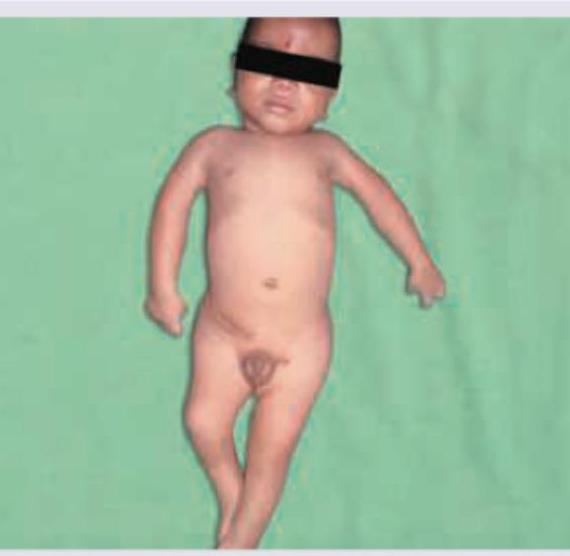
A 2-year-old child presents with developmental delay and hypotonia. The following image shows:
An obese 3-year-old, short stature child with history of hyperphagia, almond eyes and small hands and feet is brought for consultation. On neurological examination hypotonia is noted. IQ is very low. The probable cause is?
A neonate presents with the clinical features shown in the image below. What is the most likely diagnosis?
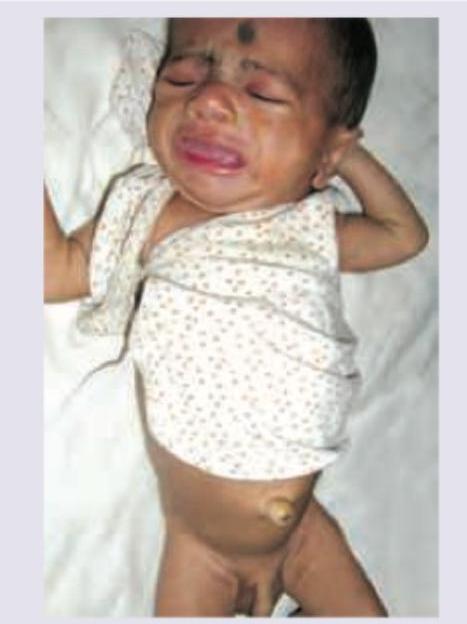
All are seen in this child except:
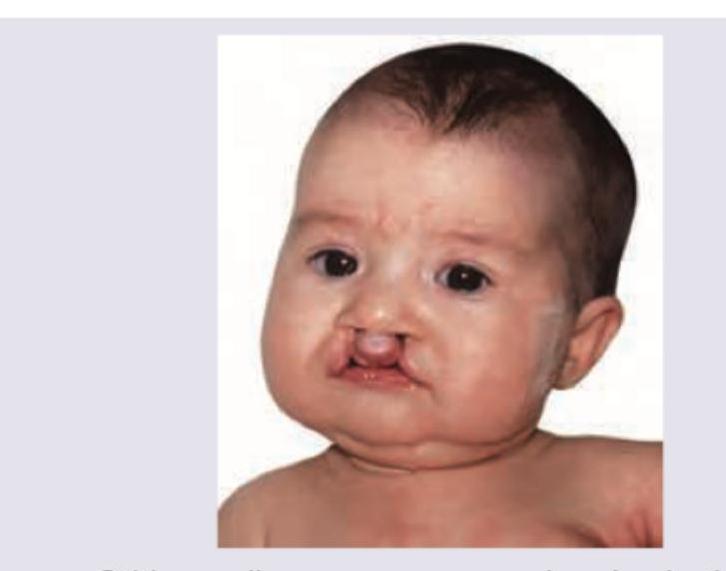
Practice by Chapter
Normal Development and Variations
Practice Questions
Developmental Delay and Intellectual Disability
Practice Questions
Autism Spectrum Disorders
Practice Questions
Attention Deficit Hyperactivity Disorder
Practice Questions
Learning Disabilities
Practice Questions
Language and Speech Disorders
Practice Questions
Motor Disorders
Practice Questions
Behavioral Problems in Young Children
Practice Questions
Sleep Disorders
Practice Questions
Mood and Anxiety Disorders
Practice Questions
Psychosomatic Disorders
Practice Questions
Developmental Surveillance and Screening
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
