Developmental and Behavioral Pediatrics — MCQs

On this page
A 3-year-old child presents with diurnal enuresis and soiling of clothes. What is the required treatment?
A 5-year-old girl is referred for evaluation of bed-wetting. The mother states that her daughter has never fully gained control of her bladder. It took her an extended period of time to grow out of diapers, and the girl has finally stopped having "accidents" during the day. However, she continues to wet her bed at night. The patient has developed normally in all other aspects and will be starting kindergarten in three months. Both her mother and father are extremely frustrated and have been losing sleep, as the girl wakes up at night 4 to 5 times per week. Physical examination is unremarkable. Which of the following will most likely be the result of further investigation?
What is the most common age group affected by infantile colic?
A 3-year-old girl with normal developmental milestones, except for delayed speech onset at four years old, shows a lack of peer interaction and a preference for routine in eating, playing, and sleeping. She experiences temper tantrums when faced with changes. What is the likely diagnosis?
Which of the following findings is NOT true about Fragile X syndrome?
Which of the following is a preventable cause of mental retardation?
An 8-year-old child presents with enuresis (bedwetting). The parents mention the child had a fall from bed once, but has no other significant medical history. There are no signs of urinary tract infection or neurological deficits. What is the best next step in management?
A young boy is brought to the clinic for developmental assessment. On examination, he has a prominent epicanthal fold, a single transverse palmar crease, hypotonia, and intellectual disability. Facial features appear flat with upslanting palpebral fissures. What is the most likely diagnosis?
A 9-month-old child is brought to OPD with developmental concerns. The child cannot sit without support, says "dada" and "mama", and has stranger anxiety. What is the appropriate management?
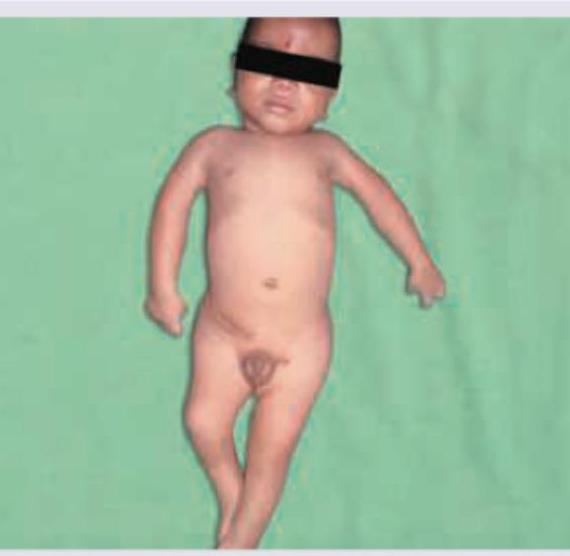
Comment on the diagnosis of this child with hypoactive deep tendon reflexes and reduced range of movement at all joints:
Practice by Chapter
Normal Development and Variations
Practice Questions
Developmental Delay and Intellectual Disability
Practice Questions
Autism Spectrum Disorders
Practice Questions
Attention Deficit Hyperactivity Disorder
Practice Questions
Learning Disabilities
Practice Questions
Language and Speech Disorders
Practice Questions
Motor Disorders
Practice Questions
Behavioral Problems in Young Children
Practice Questions
Sleep Disorders
Practice Questions
Mood and Anxiety Disorders
Practice Questions
Psychosomatic Disorders
Practice Questions
Developmental Surveillance and Screening
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
