Developmental and Behavioral Pediatrics — MCQs

On this page
Which conditions are associated with Mitral Regurgitation (MR)?
Some children go through a period of intense appetite when they eat or chew on all sorts of inedible substances. What is this called?
Which of the following statements is NOT true regarding thumb sucking?
Which of the following methods cannot be used to detect subtelomeric fractions in children with idiopathic MR?
A 6-year-old child has an IQ of 50. Which of the following tasks should the child be able to perform?
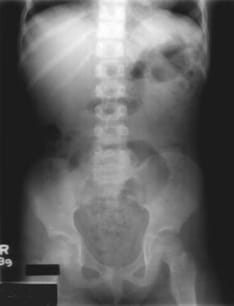
A 6-year-old boy presents with a 3-month history of soiling his underwear almost daily, despite being toilet trained at 2 years of age without difficulty. He has also experienced ongoing constipation for the last 2 years and frequently states, "I didn't know I had to go." He is otherwise healthy, performing well in school, and has a stable home environment. Examination reveals stool in the rectal vault. A plain radiograph of his abdomen is provided. What is the most appropriate initial management for this condition?
Regression of milestones occurs after normal development up to which age in Rett's disease?
Which is the most common genetic cause of mental retardation?
Which of the following is FALSE regarding thumb sucking?
What is true about autism?
Practice by Chapter
Normal Development and Variations
Practice Questions
Developmental Delay and Intellectual Disability
Practice Questions
Autism Spectrum Disorders
Practice Questions
Attention Deficit Hyperactivity Disorder
Practice Questions
Learning Disabilities
Practice Questions
Language and Speech Disorders
Practice Questions
Motor Disorders
Practice Questions
Behavioral Problems in Young Children
Practice Questions
Sleep Disorders
Practice Questions
Mood and Anxiety Disorders
Practice Questions
Psychosomatic Disorders
Practice Questions
Developmental Surveillance and Screening
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
