Cardiology — MCQs

On this page
Which congenital heart disease is associated with the defect shown in the diagram below?
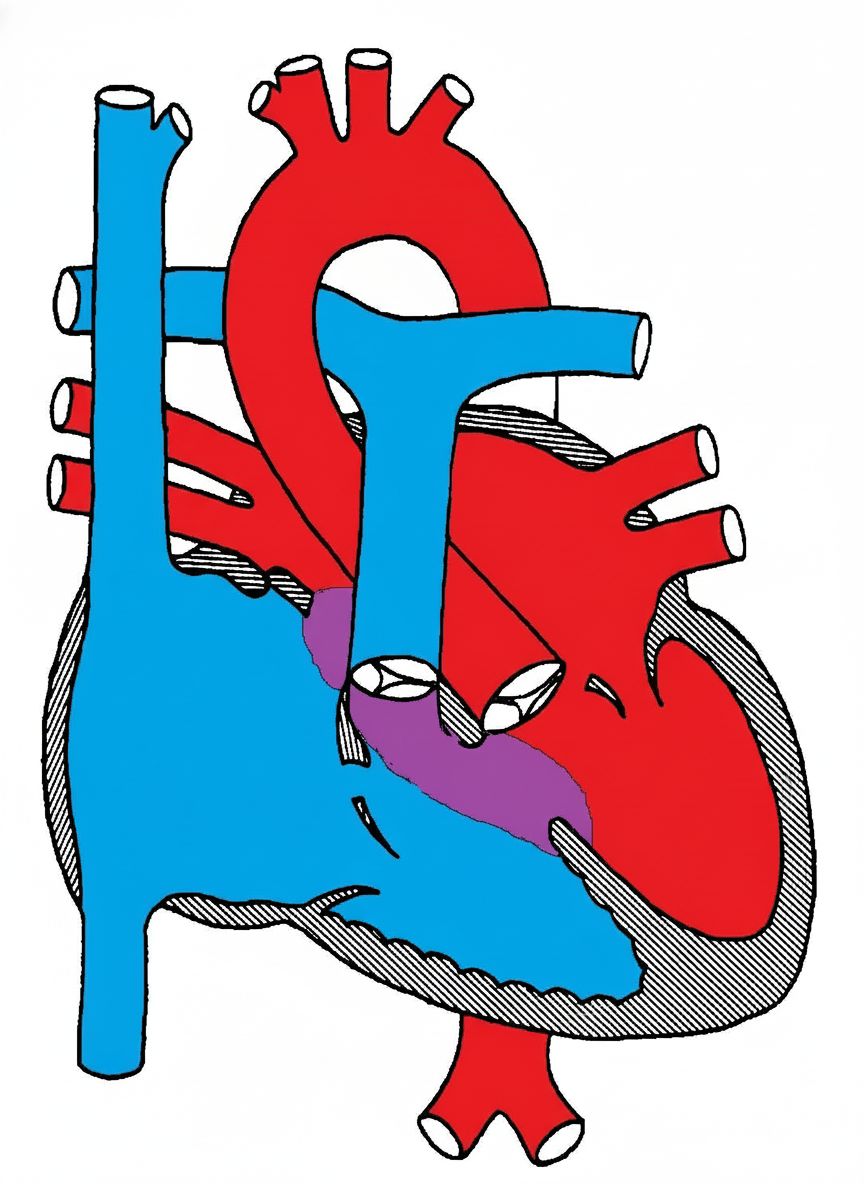
Which of the following is NOT a sign of congestive cardiac failure in infants?
Which of the following is NOT a cause of Long QT syndrome in children?
A 1-year-old child presents with mental retardation, seizures, and facial angiofibromas. The child also experiences repeated episodes of syncope. An echocardiogram reveals a mass in the left ventricle causing intermittent obstruction. Pathologic examination of the resected mass demonstrates a cardiac rhabdomyoma. Which of the following lesions would this patient most likely also have?
What is the most common benign tumor of the heart in children?
All are true in Kawasaki disease except?
What is the most common manifestation of rheumatic fever?
How is congestive cardiac failure diagnosed in an infant?
Which congenital heart defect (CHD) will lead to a left-to-right shunt, generally with cyanosis?
Modified Jones's criteria includes all the following as major criteria except?
Practice by Chapter
Congenital Heart Diseases: Cyanotic
Practice Questions
Congenital Heart Diseases: Acyanotic
Practice Questions
Rheumatic Heart Disease
Practice Questions
Kawasaki Disease
Practice Questions
Infective Endocarditis
Practice Questions
Myocarditis and Cardiomyopathies
Practice Questions
Arrhythmias in Children
Practice Questions
Heart Failure in Children
Practice Questions
Pulmonary Hypertension
Practice Questions
Systemic Hypertension
Practice Questions
Dyslipidemia in Children
Practice Questions
Cardiac Evaluation and Diagnostics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
