Cardiology — MCQs

On this page
A 3-year-old child presents with the clinical features shown in the image. What is the most likely diagnosis?
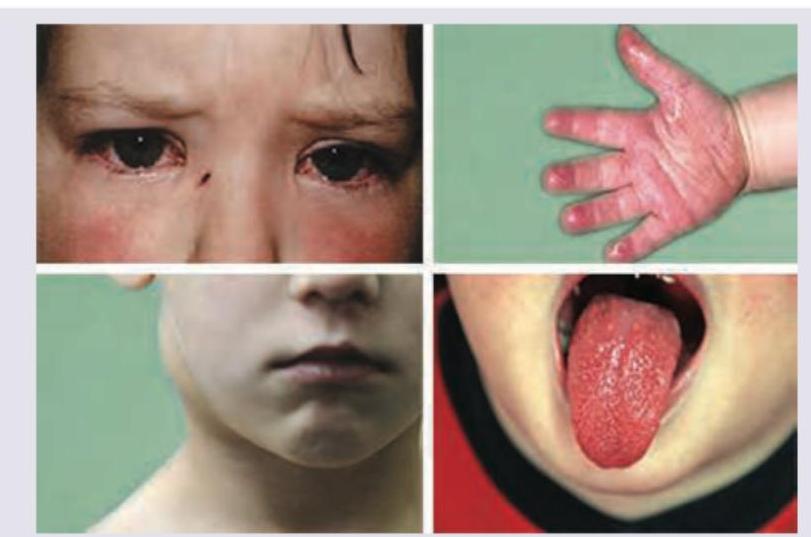
A 10-year-old child with Valvular heart disease on heart failure treatment, has the following ECG tracing. What is the diagnosis?
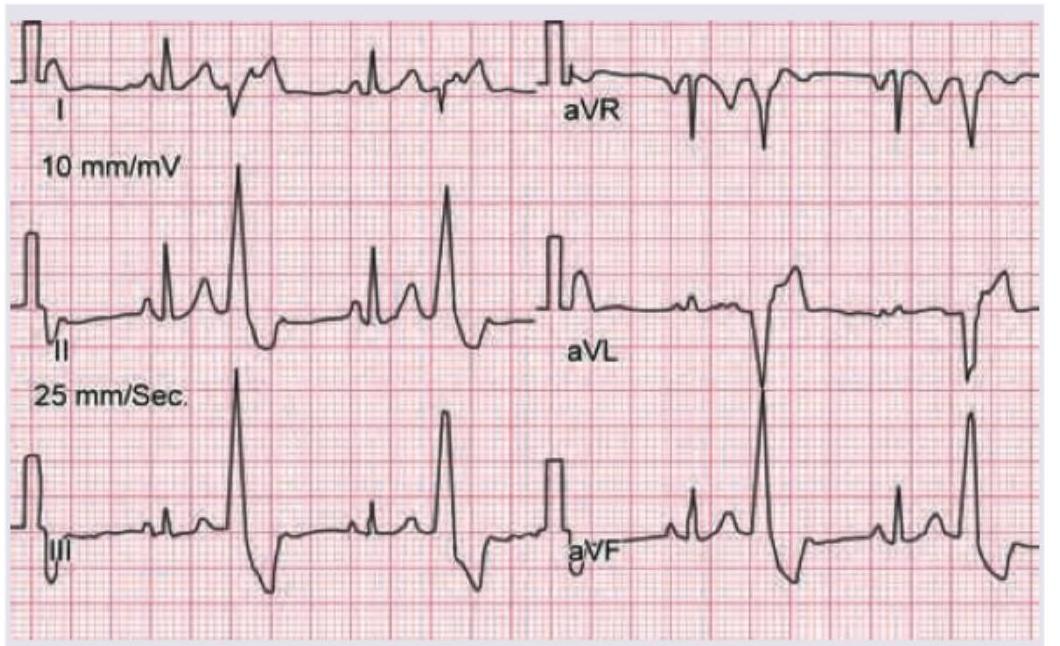
A 1-year-old child with CHD is on heart failure treatment. The ECG shows all except:
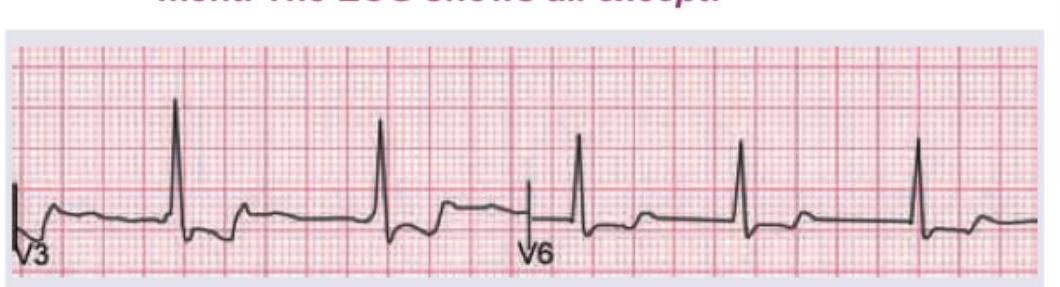
Which one of the following is a cyanotic congenital heart disease?
Which of the following cyanotic heart diseases cause increased pulmonary blood flow? 1. Ebstein anomaly 2. Tetralogy of Fallot 3. Transposition of the great arteries (TGA) 4. Total anomalous pulmonary venous communication (TAPVC) Select the correct combination:
Which of the following is considered a minor clinical finding suggestive of congenital heart disease?
A child with fever for 6 days, strawberry tongue, conjunctival congestion with peeling of skin. What will be the treatment option for this child?
Which of the following congenital heart disease has equal saturation in all heart chambers?
Most common cardiac abnormality in Noonan syndrome is:-
Ebstein anomaly is due to -
Practice by Chapter
Congenital Heart Diseases: Cyanotic
Practice Questions
Congenital Heart Diseases: Acyanotic
Practice Questions
Rheumatic Heart Disease
Practice Questions
Kawasaki Disease
Practice Questions
Infective Endocarditis
Practice Questions
Myocarditis and Cardiomyopathies
Practice Questions
Arrhythmias in Children
Practice Questions
Heart Failure in Children
Practice Questions
Pulmonary Hypertension
Practice Questions
Systemic Hypertension
Practice Questions
Dyslipidemia in Children
Practice Questions
Cardiac Evaluation and Diagnostics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
