Cardiology — MCQs

On this page
What could be the possible diagnosis for a newborn exhibiting weak lower limb pulses and strong upper limb pulses?
A 9-month-old infant presents with severe respiratory distress, central cyanosis not improving with oxygen, and a harsh systolic murmur. Chest X-ray shows boot-shaped heart with decreased pulmonary vascular markings. Echocardiography confirms the diagnosis. What is the most likely underlying cardiac defect?
A 4-year-old child presents with high-grade fever for 5 days, bilateral non-purulent conjunctival injection, strawberry tongue, cervical lymphadenopathy (>1.5 cm), and polymorphous rash. On day 6, desquamation of fingertips begins. Echocardiography shows coronary artery dilation. What is the most appropriate immediate treatment?
A 3-year-old child is brought to the clinic with a history of cyanosis since infancy. Which of the following is a component of Tetralogy of Fallot (TOF)?
A 6-week-old term baby presents with poor feeding. All are true about the condition shown except:
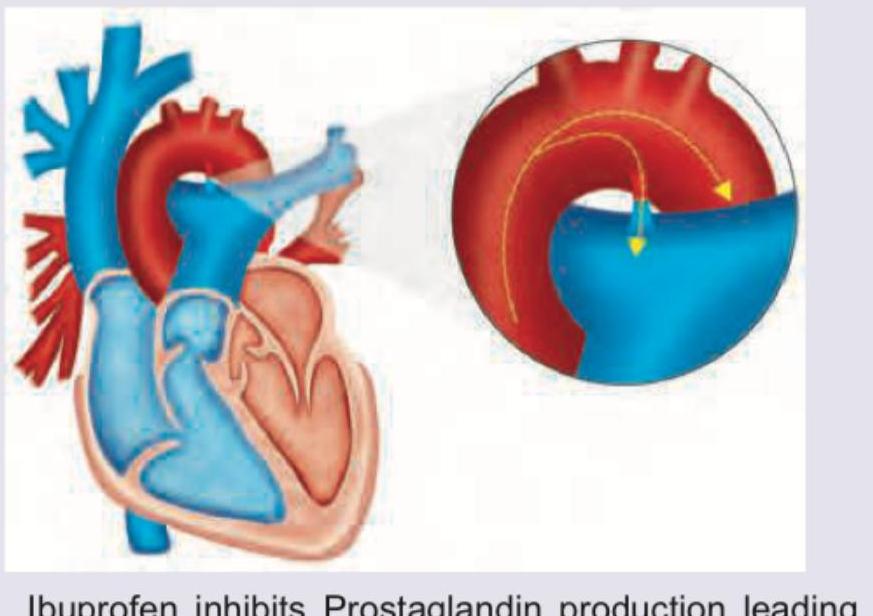
Which congenital heart disease is associated with the defect shown?
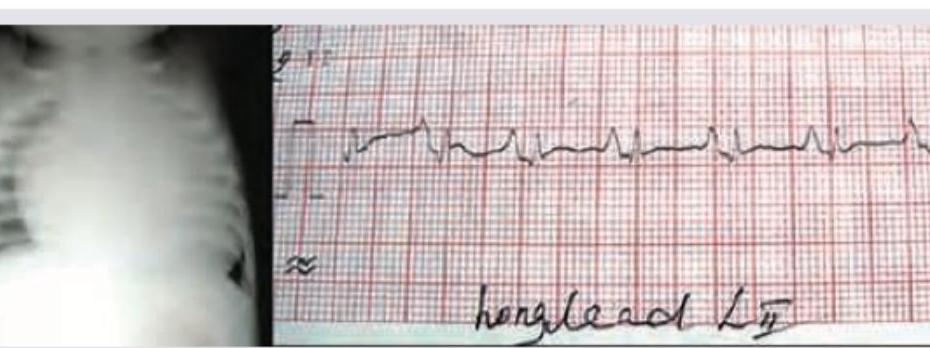
A 1 day old neonate presents with central cyanosis. CXR and ECG are performed (shown in the image). Which diagnosis is most consistent with these findings?
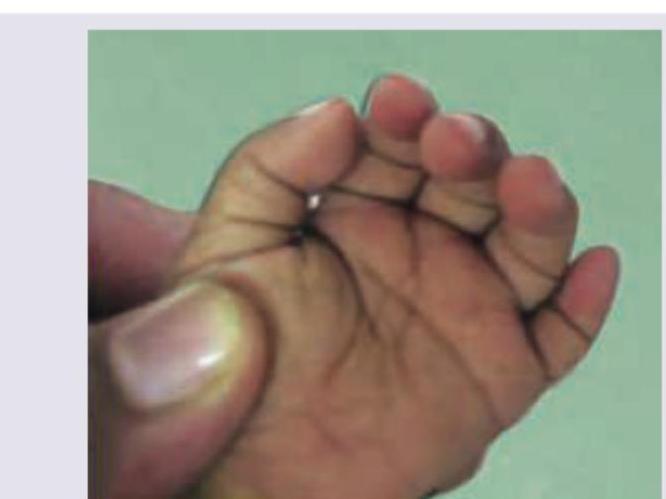
Child presents with strawberry tongue, fever for 5 days, cracked lips, Periungual peeling of the skin and bulbar congestion. Which of the following cardiac lesions will be seen in this child?
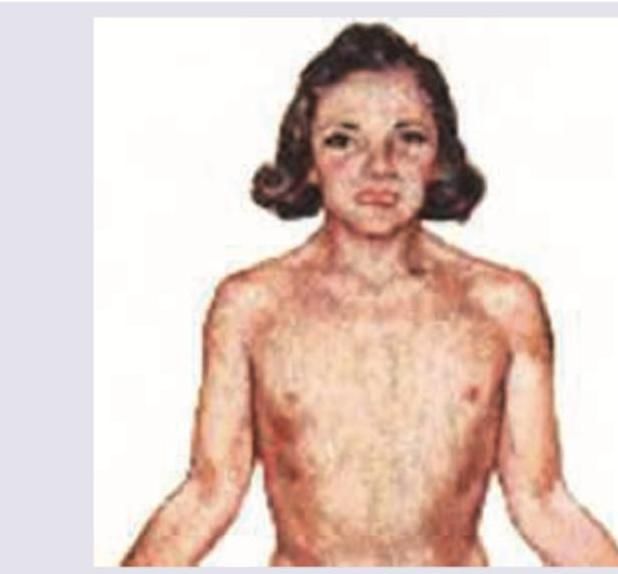
What is the expected karyotype in this child with the following findings and having pulmonic stenosis on Echocardiography?
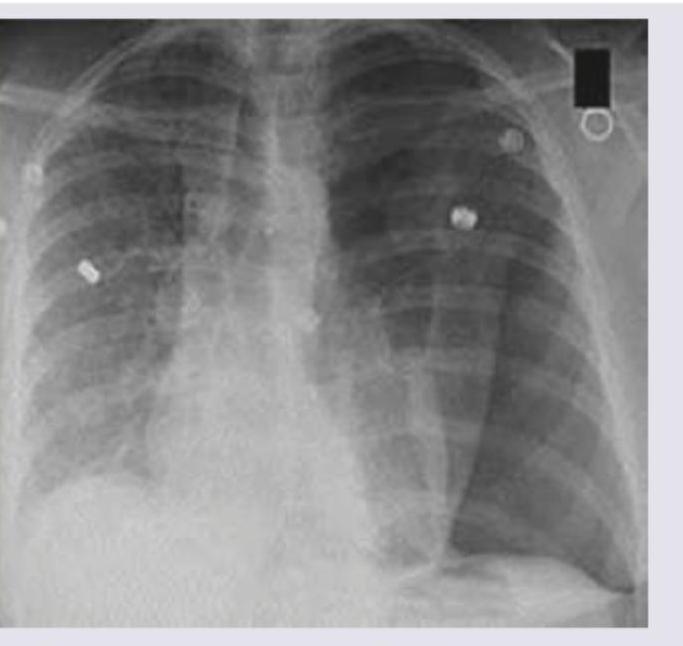
A 1-year-old child with severe acute malnutrition develops pneumonia which is not responding to treatment. Chest X-ray picture is given. What is the likely etiology?
Practice by Chapter
Congenital Heart Diseases: Cyanotic
Practice Questions
Congenital Heart Diseases: Acyanotic
Practice Questions
Rheumatic Heart Disease
Practice Questions
Kawasaki Disease
Practice Questions
Infective Endocarditis
Practice Questions
Myocarditis and Cardiomyopathies
Practice Questions
Arrhythmias in Children
Practice Questions
Heart Failure in Children
Practice Questions
Pulmonary Hypertension
Practice Questions
Systemic Hypertension
Practice Questions
Dyslipidemia in Children
Practice Questions
Cardiac Evaluation and Diagnostics
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
